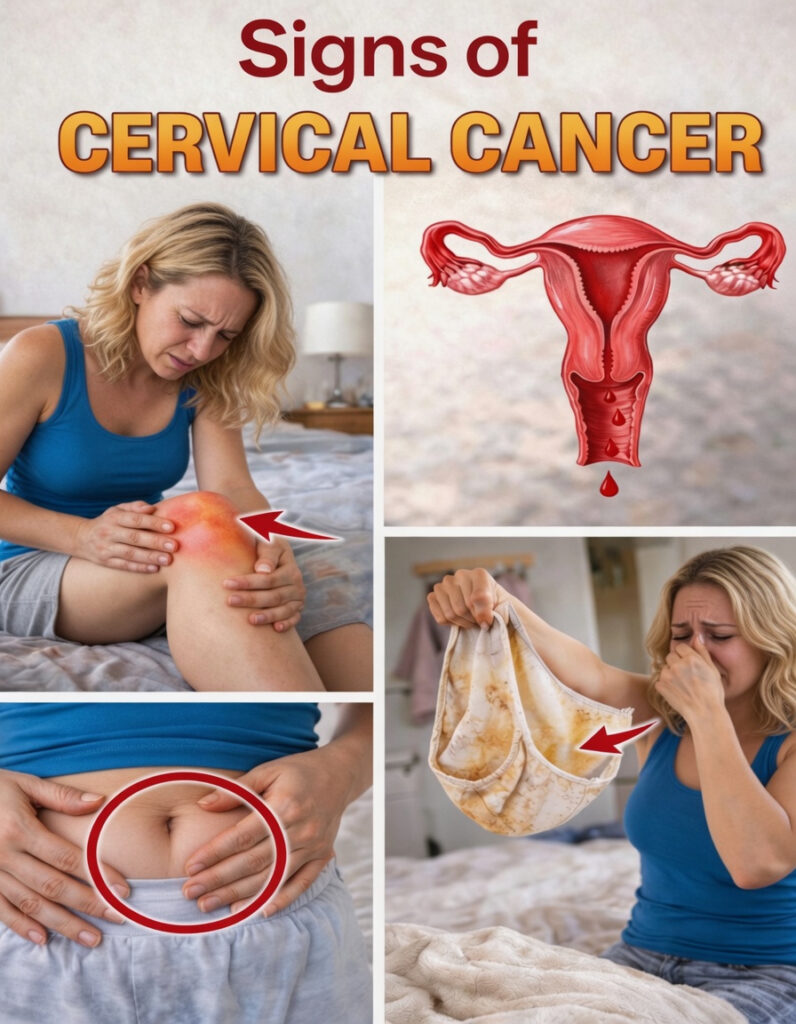
Subtle Cervical Cancer Signs Women Should Not Ignore
Many women dismiss irregular spotting, unusual discharge, or persistent aches as stress, hormones, or simply part of everyday life. However, these small body changes can sometimes signal a more serious health issue that should not be overlooked. Uncertainty about what is normal can be stressful, especially when unexplained symptoms start interfering with daily comfort and peace of mind. The reassuring part is that awareness and regular medical screening can make a major difference.
What many women do not realize until much later is that one of the most important warning signs can show up during ordinary moments. Recognizing it early may help you seek care sooner and prevent problems from becoming more serious.
Why Early Awareness Is So Important
Cervical cancer can develop with little to no noticeable symptoms at first. That is why organizations such as the Mayo Clinic and the Centers for Disease Control and Prevention strongly recommend routine screening rather than waiting for obvious symptoms.
When changes do appear, they are often easy to explain away as menopause, stress, or a minor infection. Still, noticing these shifts early gives you a better opportunity to speak with your doctor and get proper evaluation. This is not about creating fear. It is about staying informed and taking control of your health.
9 Common Warning Signs Women Often Miss
The symptoms below are based on trusted medical guidance. Keep in mind that they do not automatically mean cervical cancer, since many other conditions can cause similar issues. They are simply signs that deserve medical attention.
1. Bleeding After Sex
Even mild spotting following intercourse can be unexpected. Some women assume it is caused by dryness or friction, but it is one of the first warning signs healthcare experts often mention.
2. Bleeding Between Periods
Unexpected bleeding outside your normal menstrual cycle may be blamed on stress or birth control. Even so, it is an important change to monitor because it interrupts your usual pattern.
3. Bleeding After Menopause
If you have gone 12 months without a period, any bleeding afterward should be checked by a doctor. Many women are caught off guard by this and may assume it is harmless.
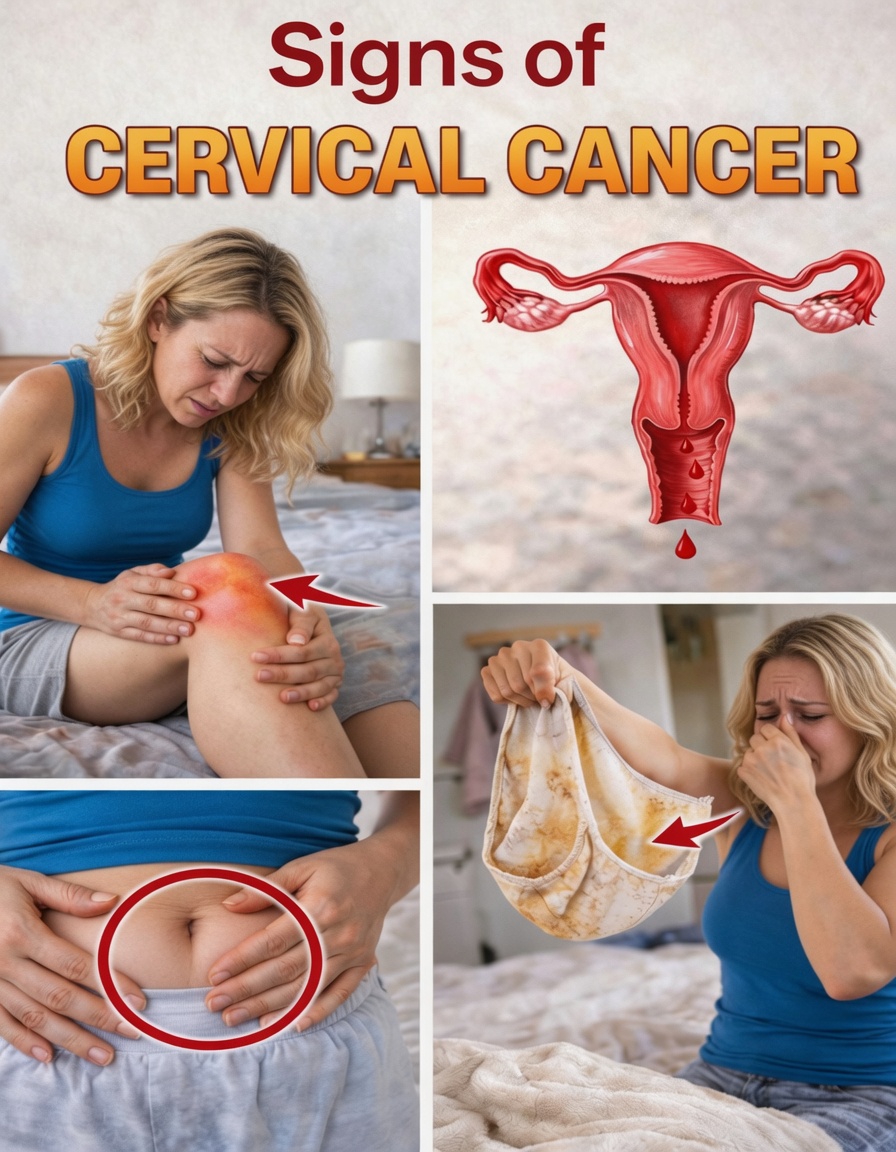
4. Heavier or Longer Periods Than Usual
A menstrual flow that suddenly becomes stronger or lasts significantly longer can be easy to dismiss as age-related change or lifestyle-related. Tracking these differences can help identify unusual patterns early.
5. Unusual Vaginal Discharge
Discharge that is watery, pink, brown, or has a strong unpleasant odor, especially between periods or after menopause, should not be ignored. The American Cancer Society identifies this as a common early symptom.
6. Pain During Intercourse
Sex should not suddenly become painful without explanation. If discomfort or sharp pain appears and continues, it is worth discussing openly with your healthcare provider.
7. Ongoing Pelvic or Lower Abdominal Pain
A lingering ache in the lower abdomen or pelvic area is often mistaken for digestive trouble or muscle strain. But if it continues for weeks, it deserves attention.
8. Lower Back, Leg, or Knee Pain
Pain that spreads into the lower back, legs, or even around the knees can appear as the condition becomes more advanced. In some cases, swelling in one leg may happen as well.
9. Trouble Urinating or Changes in Bowel Movements
Difficulty emptying the bladder, pressure while urinating, or unexplained changes in bowel habits may not seem related at first. However, they can sometimes be part of a larger medical issue and should be addressed promptly.

What You Should Do Next
Recognizing symptoms is only the first step. Taking action early is where the real benefit begins.
5 Practical Steps You Can Start Today
These simple habits can support cervical health and help you stay proactive.
-
Book your next screening
- Pap tests and HPV tests are fast and are generally recommended every 3 to 5 years for most women between ages 21 and 65.
-
Keep track of symptoms
- Use your phone or a health app to record bleeding, discharge, pain, or anything unusual for at least two weeks before your appointment.
-
Talk about your medical and family history
- Let your doctor know if there is a history of HPV, abnormal Pap results, or cervical conditions.
-
Ask about the HPV vaccine
- If you are eligible, the vaccine may still offer protection for many adults under age 45 against the primary cause of cervical cancer.
-
Support your overall health
- Eat more fruits and vegetables, stay physically active, and avoid smoking to help your immune system function well.
Small steps like these can build confidence and help you feel more in control of your health.
How Screening Can Change the Outcome
One of the most important facts to understand is that many cervical changes are discovered long before symptoms begin. Routine pelvic exams and modern screening tests can detect abnormal cells years in advance. That is why cervical cancer is often described as one of the most preventable cancers when women stay consistent with check-ups.
You do not need to live in constant worry. You need reliable information and a plan you can follow.
What This Means for You Right Now
Paying closer attention to your body does not mean overreacting to every symptom. It means becoming a stronger advocate for your own well-being. Many women who catch health issues early later say the same thing: they wish they had recognized the signs sooner, but they are grateful they finally took action.
Choose one step this week. Schedule a screening. Start a symptom log. Have the conversation you have been putting off. Your future self may be grateful you did.
FAQ About Cervical Cancer Symptoms
Can these symptoms be caused by something other than cervical cancer?
Yes. Many of these signs can also result from infections, fibroids, endometriosis, or hormone-related changes. Only a qualified healthcare provider can determine the exact cause through proper testing.
How often should screening be done if I feel fine?
In general, women ages 21 to 29 are often advised to have a Pap test every 3 years. Between ages 30 and 65, Pap testing combined with HPV testing every 5 years is common. Your doctor may adjust this schedule based on your personal health history.
Can I reduce my risk in addition to getting screened?
Yes. The HPV vaccine, avoiding smoking, practicing safer sex, and maintaining a healthy weight may all help lower your risk. Speak with your healthcare provider about the options that best fit your situation.
Disclaimer
This article is intended for informational and educational purposes only. It does not replace professional medical advice, diagnosis, or treatment. If you notice concerning symptoms or changes in your body, consult a qualified healthcare provider. Every person’s health needs and medical situation are different.