9 Early Warning Signs of Cervical Cancer Many Women Overlook
Many women notice small changes in their bodies during everyday life and assume they are caused by stress, hormones, or minor health concerns. Because these shifts can seem harmless, they are often ignored. Still, some symptoms deserve closer attention and a discussion with a healthcare professional. Being aware of what your body may be signaling can help you take a more active role in protecting your health.
Why Recognizing Cervical Cancer Symptoms Early Matters
Cervical cancer develops in the cervix, which is the lower part of the uterus. In many cases, the condition causes no clear symptoms at first. That is why routine screening, including Pap tests and HPV testing, is so important, as emphasized by trusted medical organizations such as the Mayo Clinic.
When symptoms do appear, they may be mild, unclear, or easy to confuse with more common issues. Knowing the possible warning signs can help you seek medical advice sooner, without jumping to conclusions.
9 Early Signs of Cervical Cancer You Should Not Ignore
Below are nine symptoms that are often missed or dismissed. These signs do not automatically mean cancer, since many can also be linked to less serious conditions. However, they are good reasons to schedule a medical evaluation rather than try to diagnose yourself.
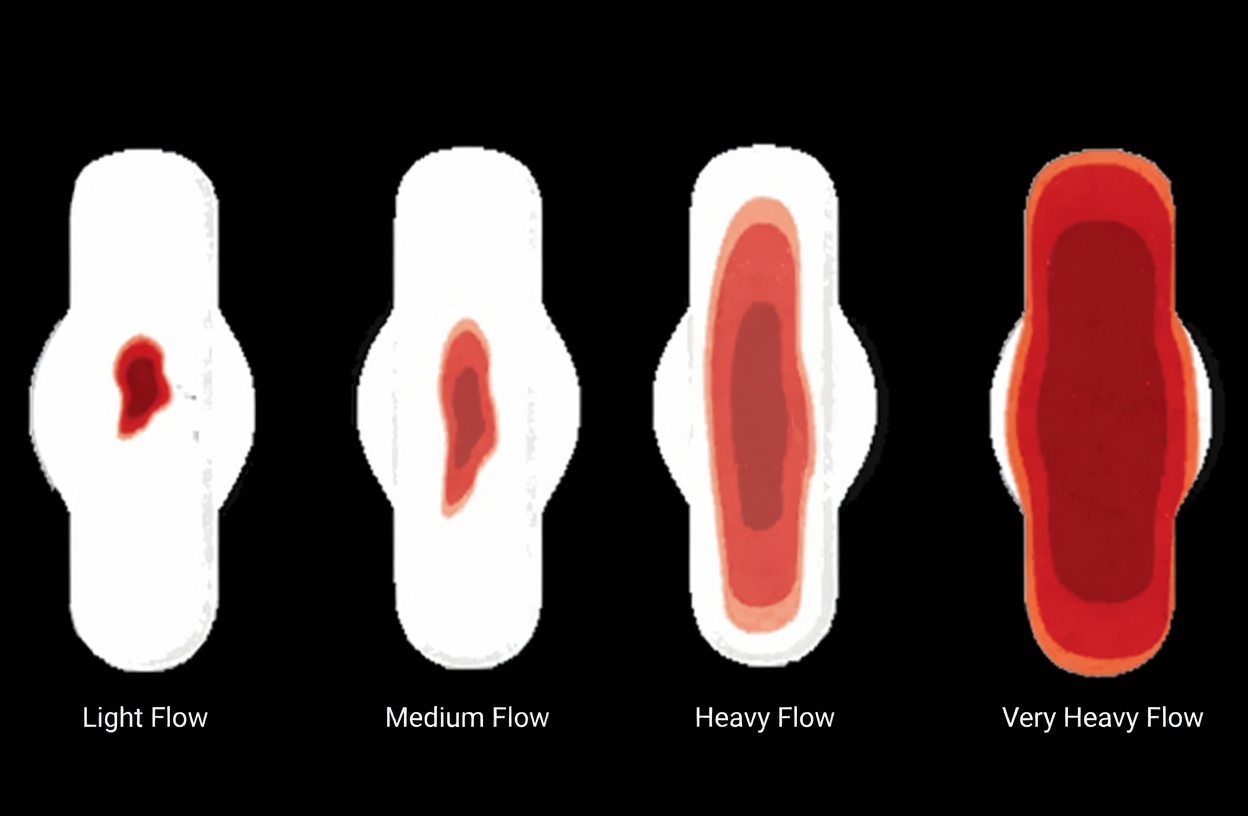
1. Unusual Vaginal Bleeding
Unexpected bleeding is one of the most well-known warning signs, yet it is still frequently brushed aside. This may include:
- Bleeding between periods
- Bleeding after sex
- Menstrual bleeding that is heavier or lasts longer than usual
- Bleeding after menopause
Even light spotting can matter, especially if it is new or different for you.
2. Changes in Vaginal Discharge
A noticeable difference in discharge can also be a signal. You may observe changes in:
- Color
- Texture
- Amount
- Odor
It may appear watery, pink, brown, or blood-tinged, or it may develop a strong smell. If the change continues, it should be mentioned to your doctor.
3. Pain During or After Sex
Pain or discomfort during intercourse can happen for several reasons, including dryness or infection. But if it keeps happening or becomes more intense, it should not be ignored.
4. Ongoing Pelvic Pain or Pressure
A dull ache, pressure, or persistent discomfort in the pelvic area that is not related to your menstrual cycle may seem minor at first. Many women assume it is just a normal part of daily life. If it does not go away, it is worth getting checked.
5. Lower Back Pain Without a Clear Cause
Lingering lower back pain can sometimes be connected to problems in the pelvic region. If the pain is not linked to exercise, lifting, or another obvious cause, it may be worth discussing with your healthcare provider.
6. Leg Pain or Swelling
This symptom often surprises women. Pain or swelling in one or both legs can happen when pelvic structures affect nerves or lymphatic drainage. While there are many possible explanations, persistent swelling or discomfort should be evaluated.
7. Unexplained Fatigue
Feeling unusually tired despite getting enough rest can be a vague symptom, but it still matters. On its own, fatigue can have many causes. When it appears alongside other changes, it becomes more meaningful.
8. Changes in Urination
Needing to urinate more often, feeling sudden urgency, or experiencing pain during urination can sometimes signal a pelvic issue. These symptoms are commonly mistaken for a urinary tract problem, so ongoing changes should not be overlooked.
9. Bloating or Changes in Bowel Habits
Persistent abdominal bloating or unexplained bowel changes, such as constipation or diarrhea, may occasionally be linked to cervical cancer or other pelvic conditions. If these symptoms continue without a clear dietary cause, they deserve attention.

Quick Checklist of Symptoms to Watch
Keep this simple list in mind:
- Bleeding outside your usual menstrual cycle
- Unusual, bloody, or foul-smelling discharge
- Pain during or after intercourse
- Ongoing pelvic pressure or pain
- Lower back discomfort with no obvious reason
- Leg swelling or pain
- Fatigue that does not improve
- Changes in urination
- Bloating or bowel changes that persist
Using a checklist like this can make it easier to notice patterns in your day-to-day health.
What You Can Do Right Now
The good news is that there are practical steps you can take today to stay proactive.
Track Any Changes
Write down symptoms in a notebook or log them in an app. Include:
- The date
- How long the symptom lasted
- How severe it felt
- Anything that seemed to trigger it
This can be extremely helpful when speaking with your doctor.
Schedule Routine Screenings
If it has been a while since your last well-woman exam, Pap test, or HPV screening, consider making an appointment. Screening recommendations vary depending on your age, health history, and risk factors, so ask your provider what schedule is right for you.
Support Your Reproductive Health
Healthy habits can also make a difference. Consider focusing on:
- Avoiding smoking
- Eating a balanced diet
- Following safe sex practices
- Staying current with recommended vaccines
One of the most important habits of all is making cervical cancer screening a regular, non-negotiable part of your routine. Like annual physicals, these check-ups can detect issues before symptoms ever start.
Prevention Strategies Supported by Research
Research from major health organizations shows that the HPV vaccine is highly effective in preventing the strains of HPV responsible for most cervical cancer cases. If you are in the recommended age group, ask your doctor whether vaccination is appropriate for you.
Other prevention steps include:
- Practicing safe sex
- Avoiding tobacco use
- Keeping up with routine gynecologic care
Still, regular screening remains one of the strongest tools for early detection and better outcomes.
Frequently Asked Questions About Cervical Cancer Symptoms
If I have one of these symptoms, does it mean I have cervical cancer?
No. Many of these symptoms can be caused by noncancerous conditions such as infections, hormonal changes, or other reproductive health issues. A medical evaluation is the only way to determine the cause.
How often should cervical cancer screening be done?
Screening frequency depends on your age, personal history, and risk level. In general, Pap testing often begins around age 21, and HPV testing may be added later. Your healthcare provider can recommend the best plan for you.
Can lifestyle choices reduce the risk?
Yes. While risk cannot be eliminated entirely, staying up to date on HPV vaccination, avoiding smoking, and practicing safe sex can help reduce your chances, especially when combined with regular screening.
Final Thoughts
Understanding these early warning signs of cervical cancer can help you respond sooner when something does not feel right. Paying attention to your body is not overreacting; it is part of taking care of yourself. If you notice any ongoing or unusual symptoms, talk to your doctor and get the answers you need. Awareness and early action can make a real difference.
Disclaimer
This article is for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or another qualified healthcare provider with any questions about a medical condition.