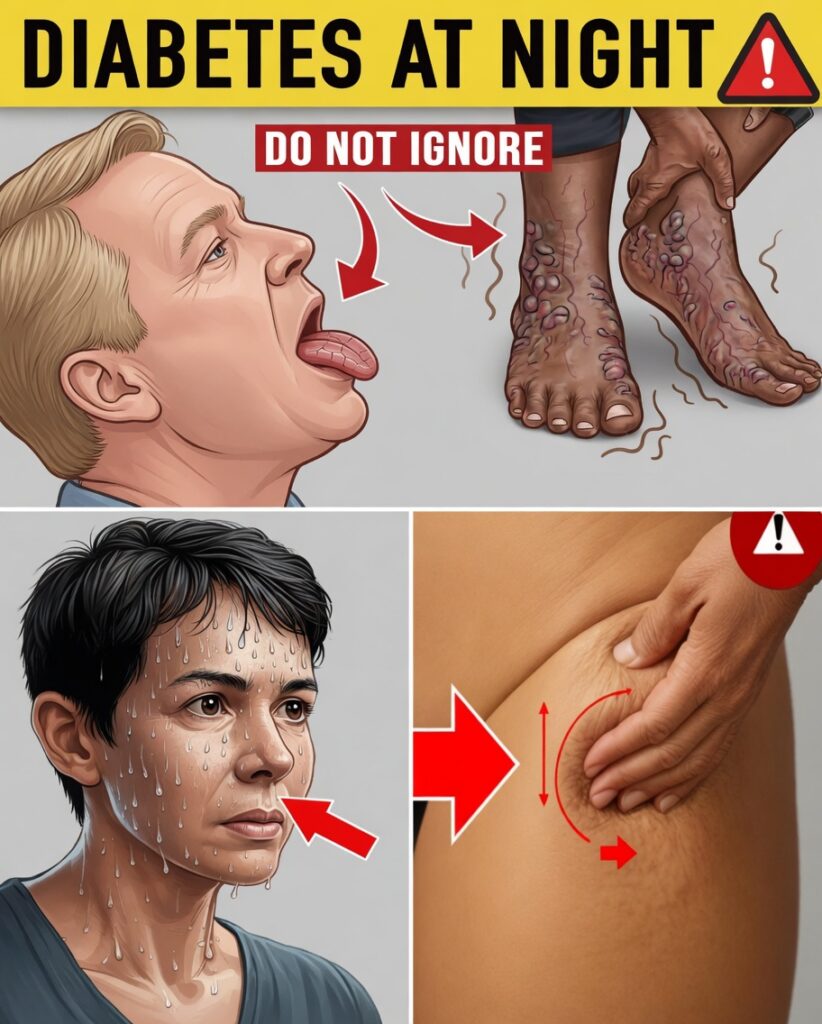
Disrupted sleep from repeated wake-ups, discomfort, or unexplained restlessness can leave many adults feeling wiped out the next day—especially when possible nighttime symptoms of diabetes aren’t recognized. These changes often develop gradually, quietly contributing to persistent fatigue and a lower quality of life. Noticing consistent night patterns may help you start an earlier, more informed conversation with a healthcare professional.
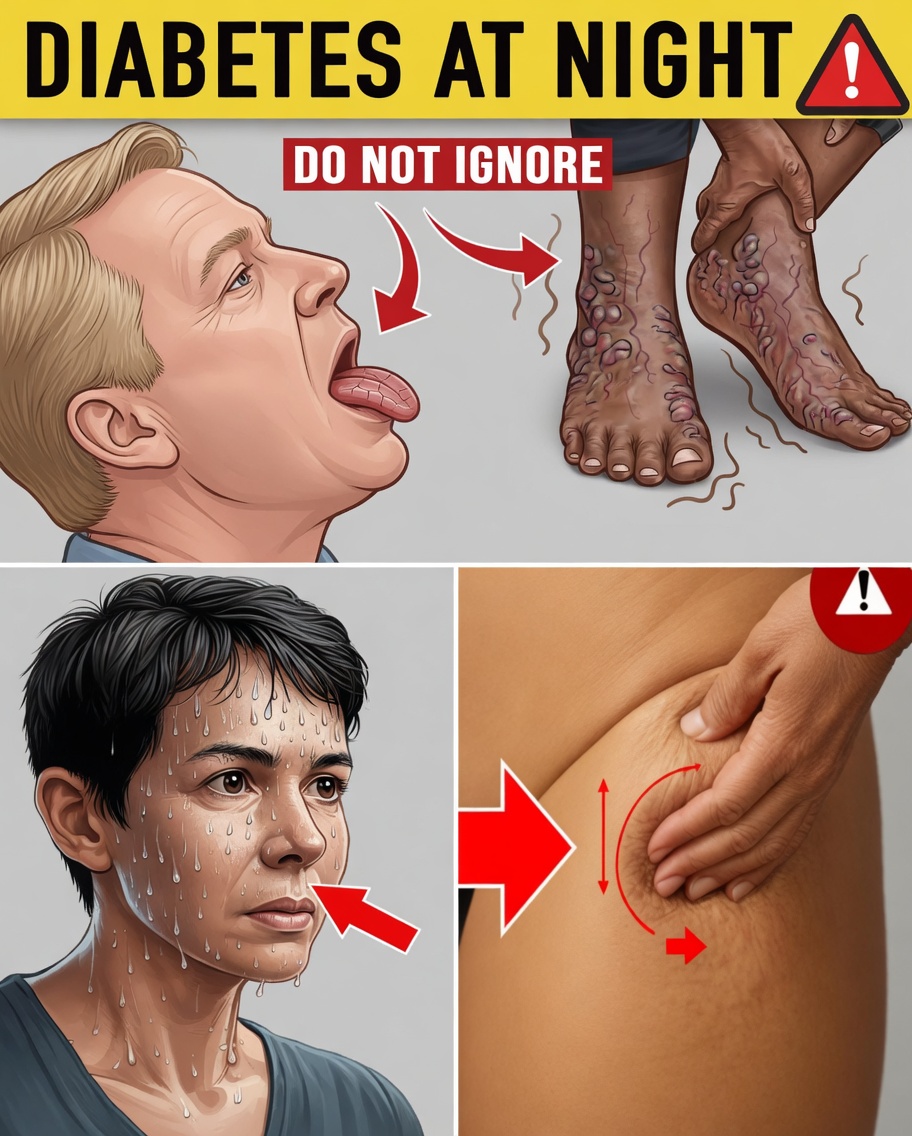
Why Nighttime Symptoms of Diabetes Matter
Blood sugar can shift significantly overnight, and those fluctuations may affect sleep without the usual daytime cues. For many people, sleep disruption linked to diabetes symptoms at night leads to more stress, reduced energy, and difficulty concentrating the following day.
Studies have shown relationships between poorly controlled glucose and disturbed sleep. Identifying and addressing potential nighttime symptoms of diabetes sooner may support more restorative rest and better overall well-being.

Common Nighttime Symptoms of Diabetes
Frequent Nighttime Urination (Nocturia)
Waking up several times to urinate can break up sleep cycles and make it hard to feel rested. One common reason is that high blood sugar can pull more fluid into the urine, increasing bathroom trips.
When nocturia becomes a regular pattern, it often results in fragmented sleep and morning grogginess. Some people notice fewer interruptions when glucose levels are monitored and managed consistently.

Excessive Thirst at Night
Strong thirst that triggers repeated trips for water may be a sign of dehydration related to elevated glucose. As a potential nighttime symptom of diabetes, it can create a loop—drinking more leads to more nighttime urination, which further disrupts sleep.
The result is often a drained, “never fully rested” feeling the next morning.
Night Sweats
Waking up sweaty enough to dampen pajamas or bedding can be associated with blood sugar dropping overnight, which may trigger adrenaline-related responses.
These nighttime diabetes symptoms can also cause chills afterward, making it even harder to fall back asleep.
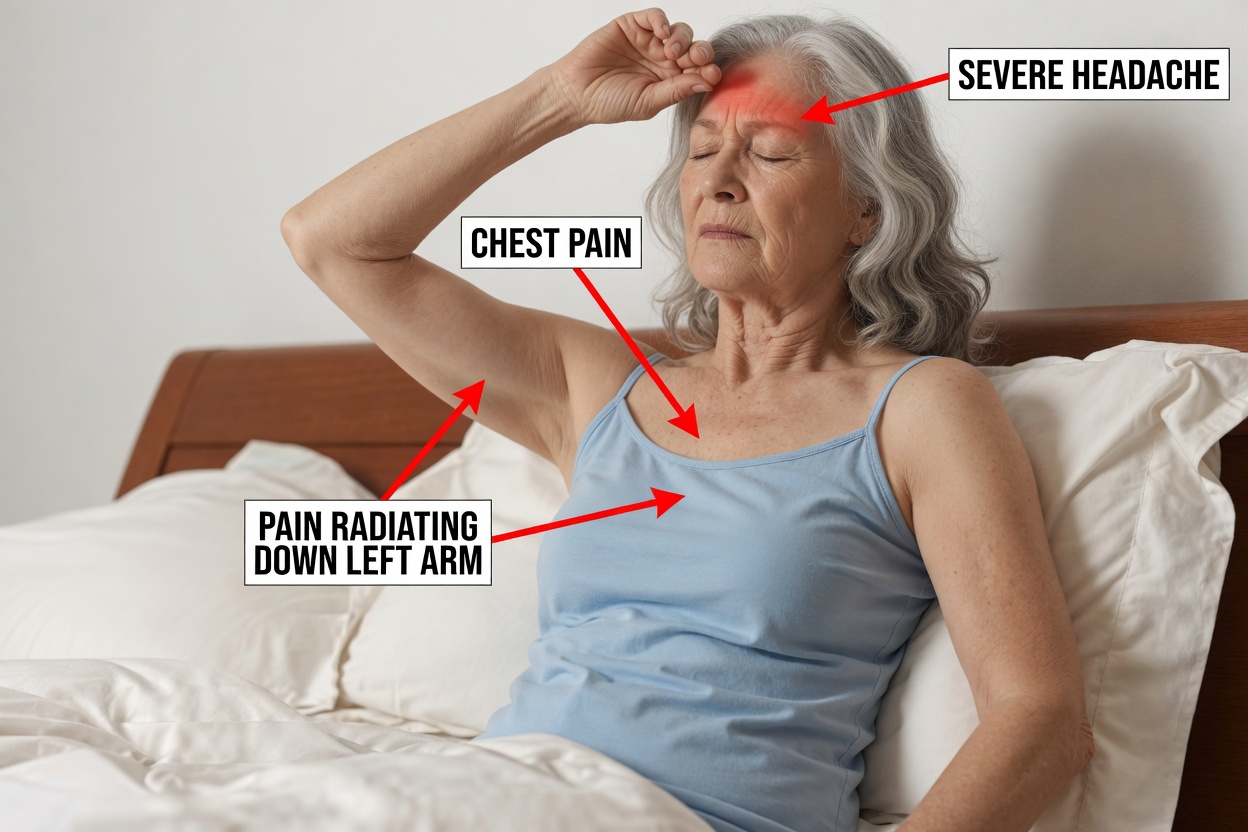
Restless Legs or Tingling Sensations
An uncomfortable urge to move the legs, pins-and-needles sensations, or tingling may be linked to nerve changes that can occur with prolonged high blood sugar.
Many people find these sensations intensify when lying down, making it difficult to relax and drift off.
Leg Cramps at Night
Sudden, painful cramps in the calves or feet can jolt someone awake and create anxiety about going back to sleep. In some cases, they may be connected to fluid or electrolyte shifts that can accompany blood sugar imbalance.
Experiencing cramps as potential nighttime symptoms of diabetes can add to overall sleep frustration.

Disrupted Breathing or Snoring Concerns
Sleep apnea is more common among people with diabetes and can cause breathing pauses that lead to repeated micro-awakenings. Even if you don’t fully wake up, these interruptions can reduce sleep quality.
This possible connection between sleep apnea and diabetes often contributes to daytime sleepiness and reduced mental clarity.
Signs of Low Blood Sugar Overnight
Overnight lows can occur quietly during sleep. Symptoms may include shaking, sweating, confusion, or a sudden feeling of alarm.
When appropriate, monitoring tools and clinician-guided plans can help manage these potential nighttime symptoms of diabetes more safely.

Nighttime Symptoms vs. Supportive Tracking Steps
| Symptom | Why It Disrupts Sleep | Gentle Monitoring Tips | Potential Benefit |
|---|---|---|---|
| Frequent urination | Multiple wake-ups break sleep cycles | Track how often you wake; note evening fluids | Fewer interruptions |
| Excessive thirst | Encourages repeated drinking and waking | If advised, check glucose before bed | Improved hydration balance |
| Night sweats | Damp sheets, chills, difficulty resettling | If on glucose-lowering meds, keep clinician-approved carbs nearby | More stable nights |
| Restless legs/tingling | Urge to move, discomfort when lying down | Light evening walks or stretching | Easier relaxation |
| Leg cramps | Sudden pain that wakes you abruptly | Hydration + gentle calf/foot stretches | Reduced frequency |
| Disrupted breathing/snoring | Repeated arousals reduce deep sleep | Discuss screening options with a doctor | Better oxygen flow and sleep quality |
| Low blood sugar signs | Adrenaline surges, sweating, confusion | Use alerts/monitors if recommended | Safer overnight management |
A Simple Timeline for Observing Nighttime Symptoms
| Timeframe | Focus | Simple Actions | What to Note |
|---|---|---|---|
| Week 1 | Awareness | Record wake-ups and symptoms each night | Early patterns |
| Weeks 2–4 | Monitoring | If applicable, check bedtime glucose as advised | Changes in frequency and intensity |
| Ongoing | Consultation | Share notes with a healthcare provider | Personalized guidance and next steps |
Practical Ways to Track Nighttime Symptoms of Diabetes
These approachable habits can make your observations more useful:
- Keep a basic sleep journal and record any nighttime symptoms of diabetes (time, what happened, and how long you were awake).
- If recommended by a clinician, check blood sugar at bedtime and note the result.
- Reduce large amounts of fluids late in the evening to help limit bathroom trips.
- Bring ongoing sleep disruption to a doctor promptly—especially if it’s worsening.
- Stick with consistent sleep and meal routines to support steadier nights.
Many people find that tracking nighttime diabetes symptoms leads to more productive conversations and clearer next steps.
Conclusion: Notice Night Patterns to Support Better Health
Paying attention to possible nighttime symptoms of diabetes—such as frequent urination, night sweats, tingling, or breathing disruptions—can be a valuable signal to seek medical guidance. Not everyone will experience the same symptoms, but awareness can encourage earlier action and better sleep. Small, consistent observations often support improved rest and long-term well-being when paired with professional care.
Frequently Asked Questions
-
When should I see a doctor about nighttime symptoms of diabetes?
If sleep disruptions continue, intensify, or interfere with daily life, schedule an evaluation with a healthcare provider. -
Can lifestyle changes improve nighttime symptoms of diabetes?
Healthy routines may help support sleep and glucose stability, but changes should be guided by medical advice—especially if you use diabetes medications. -
Are nighttime symptoms of diabetes the same for everyone?
No. Symptoms and severity vary, which is why individualized assessment is important.
Medical disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider for guidance on diabetes symptoms, blood sugar management, or sleep concerns.