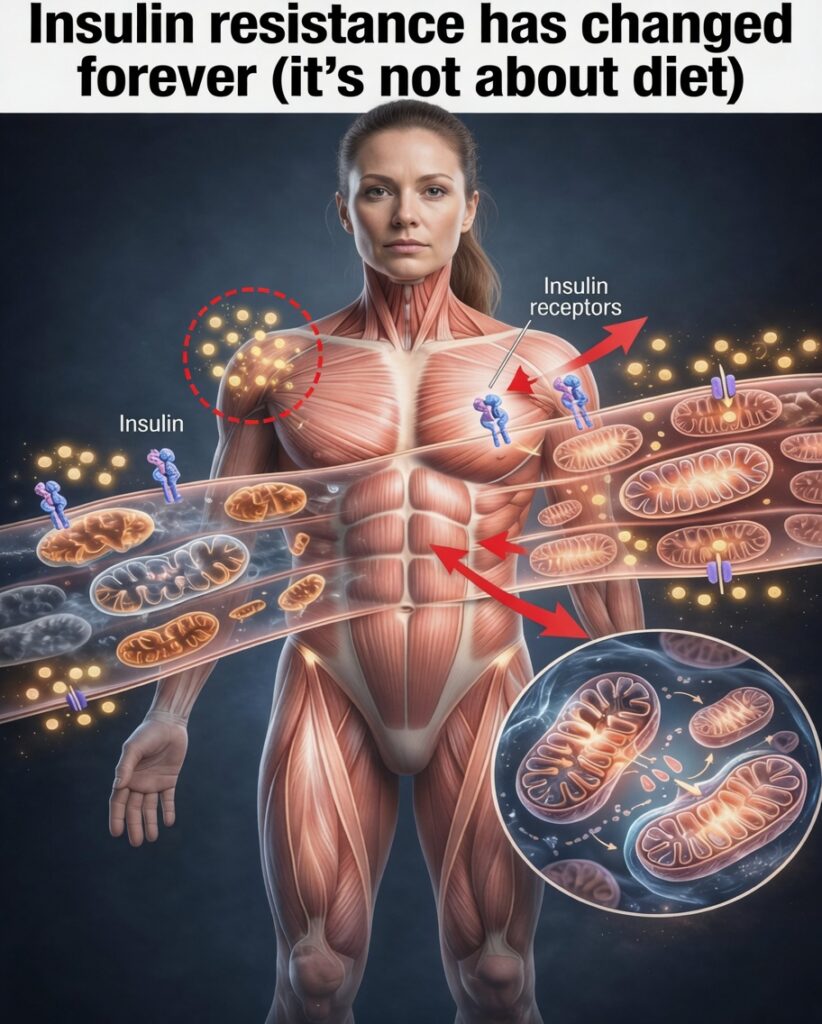
Feeling Stuck With Insulin Resistance? The Missing Piece May Be Inside Your Cells
If you’re living with insulin resistance, you may have already tried “doing everything right”—cutting carbs, tracking calories, exercising consistently—yet the scale barely moves and your energy stays low. Over time, that grind can feel defeating, especially when your effort doesn’t match your results.
For many people, the real issue isn’t just willpower or diet strategy. A growing body of discussion points to something deeper: cellular energy and mitochondrial health. When your cells can’t efficiently produce and use energy, insulin resistance may become harder to shift—no matter how strict your plan looks on paper.
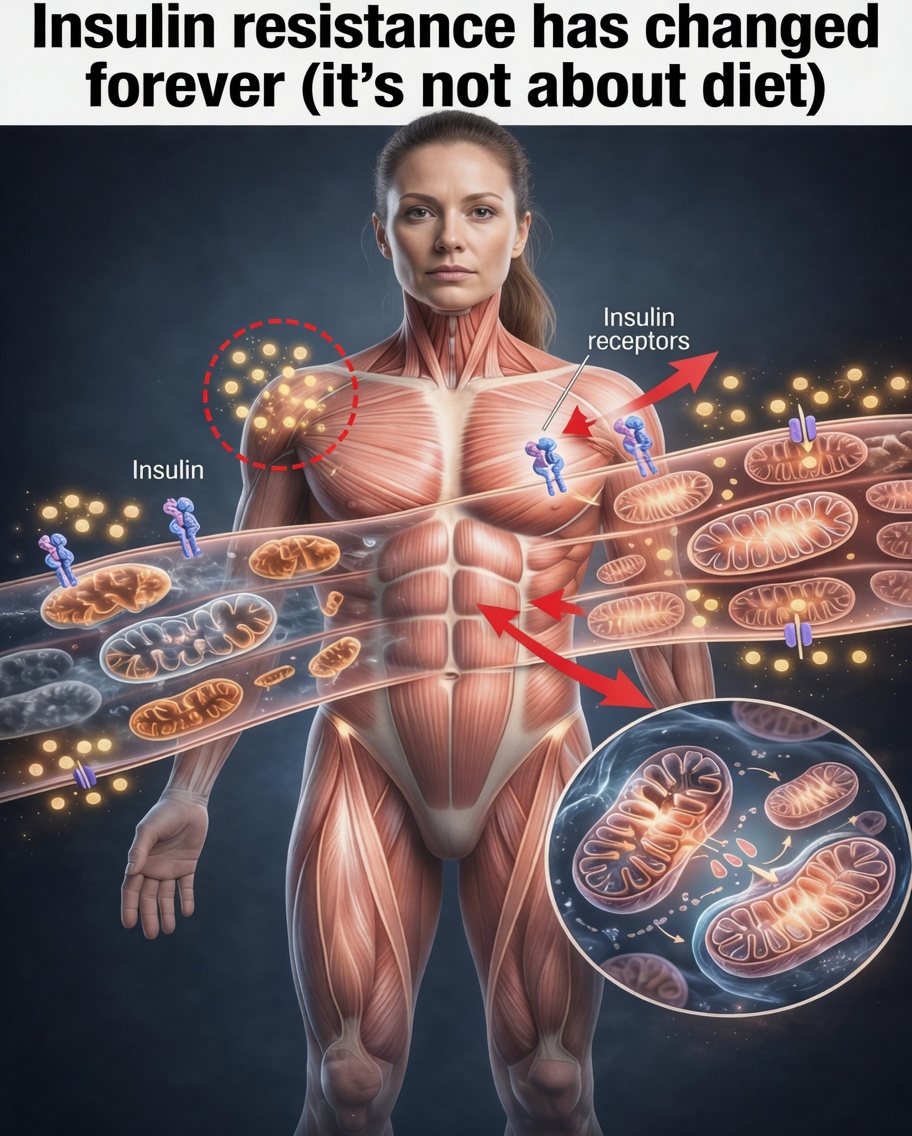
Insulin Resistance and Mitochondrial Health: Why Energy Production Matters
Traditional advice often focuses on sugar, carbs, and calorie reduction. While those factors can help, insulin resistance may also reflect how well your cells process fuel. That’s where mitochondria come in.
Mitochondria are the energy-producing structures inside your cells. When they’re functioning well, your body can convert nutrients into usable energy more effectively. When mitochondrial function declines, cells may struggle to handle glucose efficiently—potentially contributing to:
- Persistent fatigue
- Slower metabolic output
- Greater difficulty losing weight
- A cycle that reinforces insulin resistance over time
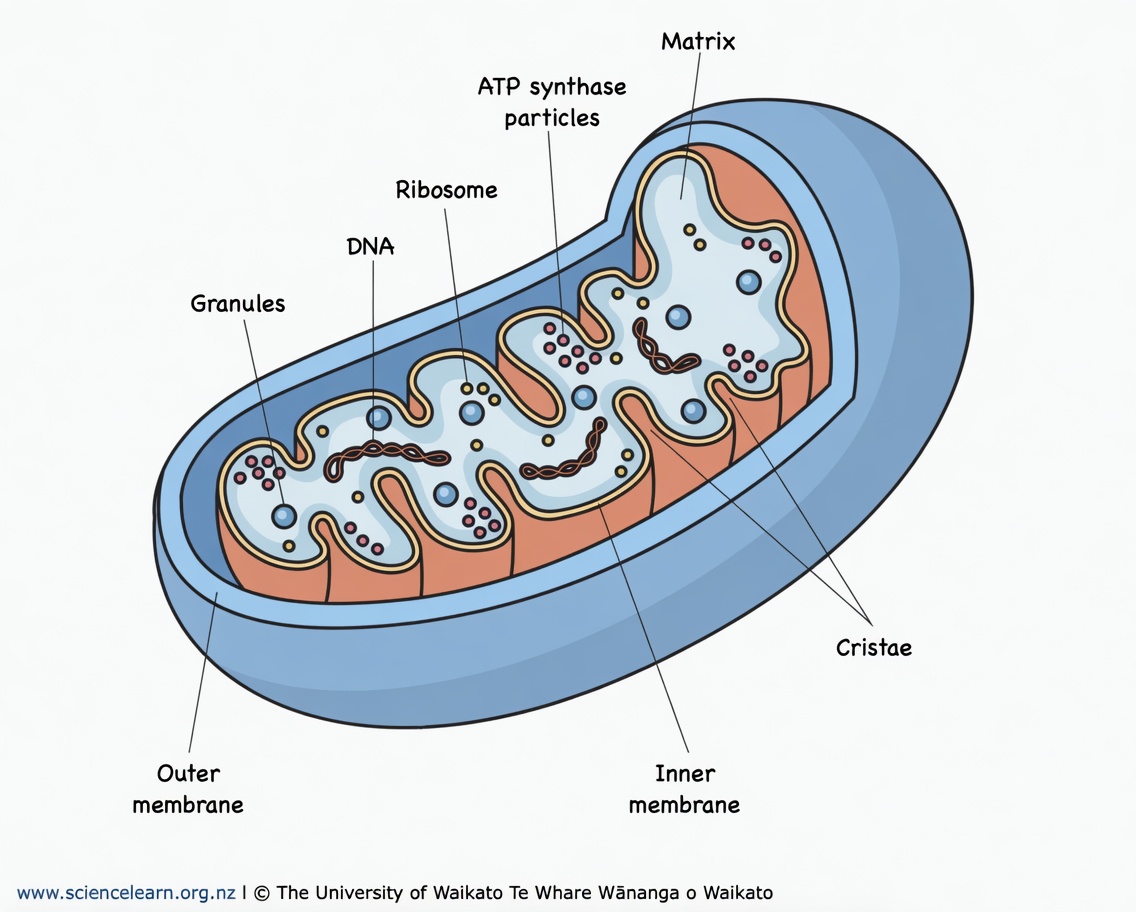
Mitochondria Are Not Just “Energy Factories”—They Influence Insulin Sensitivity
A simple way to picture mitochondria is like rechargeable batteries that power nearly every function in the body. In insulin resistance, those “batteries” may not charge well, discharge well, or adapt well to demand.
When mitochondria are underperforming, glucose may be processed less efficiently. That can amplify the common experience many people report with insulin resistance: you’re trying hard, but progress feels stalled and daily energy feels limited.
Supporting mitochondrial function may help cells use fuel more effectively, which can make insulin resistance easier to manage as part of a broader approach.
The Inflammation Loop: How Mitochondrial Stress Can Worsen Insulin Resistance
Inflammation often acts like fuel on the fire for insulin resistance. One proposed mechanism involves mitochondrial membrane damage, which may occur with low-quality, nutrient-poor diets and unstable fats. When mitochondrial membranes lose integrity, energy production can become “leaky,” increasing oxidative stress.
That oxidative stress can raise inflammation, and inflammation can further reduce how well cells respond to insulin—creating a reinforcing loop that may lead to:
- More fatigue
- Less metabolic flexibility
- Increased difficulty improving insulin sensitivity
Interrupting this cycle often starts with protecting and supporting mitochondrial health, not just reducing calories.

Why Food Quality Can Matter More Than Just Calorie Counting
For insulin resistance, calorie reduction alone doesn’t always solve the underlying problem—especially if the diet lacks nutrients that mitochondria rely on.
Nutrient density supports mitochondrial performance, including the minerals and fats needed for stable cellular membranes and efficient energy pathways. In practical terms, a dietary pattern centered on whole, minimally processed foods can better supply the building blocks that support cellular energy production over time.
A useful shift in mindset is moving from “How little can I eat?” to “How well can I nourish my cells?”

Emerging Research: Quantum Processes and Mitochondrial Energy
Some researchers exploring mitochondrial function discuss advanced mechanisms such as quantum tunneling, where particles (such as protons) move in highly efficient ways during energy production.
While this area is still evolving, the big takeaway for insulin resistance is straightforward: energy generation inside cells may be more complex than calorie math alone. If those fine-tuned processes are disrupted, overall efficiency can drop—potentially contributing to low energy and poor glucose handling.
These insights don’t replace nutrition and lifestyle basics, but they broaden how we think about why insulin resistance can feel so resistant to change.
Practical Strategies That May Support Mitochondrial Renewal
One promising concept is mitochondrial biogenesis—the process of creating newer, more efficient mitochondria. Supporting biogenesis may help improve how cells meet energy demands that are often challenging in insulin resistance.
Evidence-based strategies that may encourage mitochondrial renewal include:
- Regular exercise (some people do well with workouts in a fasted state)
- Intermittent calorie restriction rather than chronic dieting
- Fasting windows of roughly 12–18 hours, a few times per week
- Nutrient-dense eating on non-fasting days
These approaches act as “pattern interrupts,” giving mitochondria a reason to adapt—potentially improving resilience and energy handling.

Nutrients Commonly Linked to Mitochondrial Support
Several nutrients are frequently discussed for their roles in mitochondrial pathways and cellular energy production. In the context of insulin resistance, they may provide foundational support:
- Magnesium (often referenced in the range of 500–800 mg/day from food and/or supplements)
- Copper, which supports certain enzyme functions
- B vitamins, involved in multiple energy-related pathways
- High-quality saturated fats (commonly cited sources include grass-fed butter or coconut oil)
Supplement needs vary widely, and food-first approaches are often recommended when possible.
Light and Heat: Advanced Tools Some People Use
Beyond diet and training, two additional tools are often explored for mitochondrial support:
- Red and near-infrared light therapy, which may help stimulate mitochondrial activity
- Sauna or heat exposure, a hormetic stressor that may encourage cellular adaptation
These are typically considered supportive add-ons—not replacements for nutrition, movement, and recovery habits.
Simple Routine Tweaks That Can Make a Difference
Mitochondria benefit from cycles of demand and recovery. One straightforward habit is setting a clear eating boundary, such as finishing food earlier in the evening, rather than grazing late into the night.
A sustainable starting point can look like:
- Reduce constant snacking
- Add consistent movement
- Build meals around nutrient-dense foods
- Use fasting or time-restricted eating gradually, if appropriate for you
Final Thoughts
If insulin resistance has kept you stuck despite serious effort, looking at mitochondrial health can offer a wider, more practical framework. By combining nutrient quality, smart stressors (exercise, fasting, heat/light where appropriate), and consistent routines, you may support better cellular energy—and make progress feel possible again.
Frequently Asked Questions
What is the link between mitochondria and insulin resistance?
Mitochondria generate cellular energy. When mitochondrial function is impaired, cells may struggle to process glucose efficiently, which can contribute to insulin resistance and persistent fatigue.
Can lifestyle habits improve mitochondrial health?
Many approaches may help, including exercise, intermittent fasting or time-restricted eating, nutrient-dense diets, and certain therapies such as red/near-infrared light or sauna use.
If mitochondria matter, is diet still important for insulin resistance?
Yes. Food quality provides essential nutrients and fats that support mitochondrial structure and energy pathways, working alongside movement and recovery strategies.
Medical Disclaimer
This article is for informational purposes only and does not diagnose, treat, cure, or prevent any condition. Always consult a qualified healthcare professional before changing your diet, exercise routine, or supplement plan.