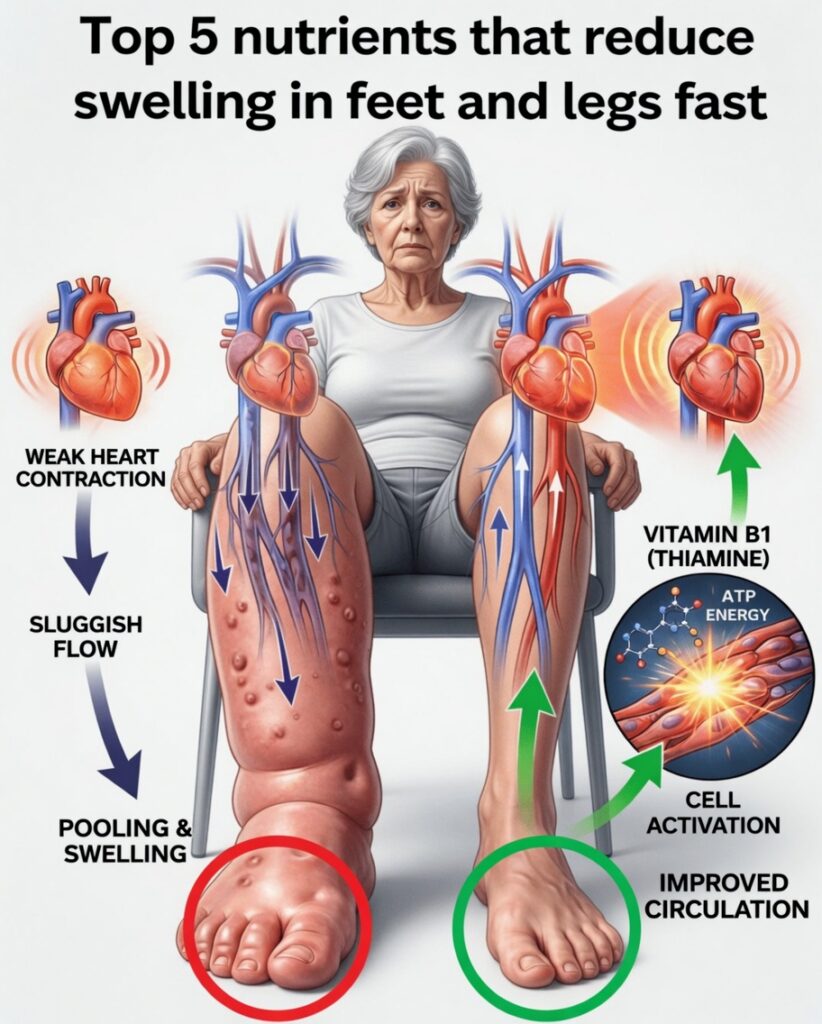
Swollen Feet and Legs: Why It Happens and Which Nutrients May Help
Swelling in the feet and legs can make everyday movement feel harder than it should. That tight, puffy sensation may build throughout the day, leaving your ankles looking larger, your shoes feeling snug, and your legs feeling heavy. Beyond discomfort, swelling can affect sleep, confidence, and overall quality of life.
The encouraging news is that, alongside healthy lifestyle choices, certain nutrients may support your body’s natural fluid balance and help reduce swelling in feet and legs when included as part of a balanced diet.
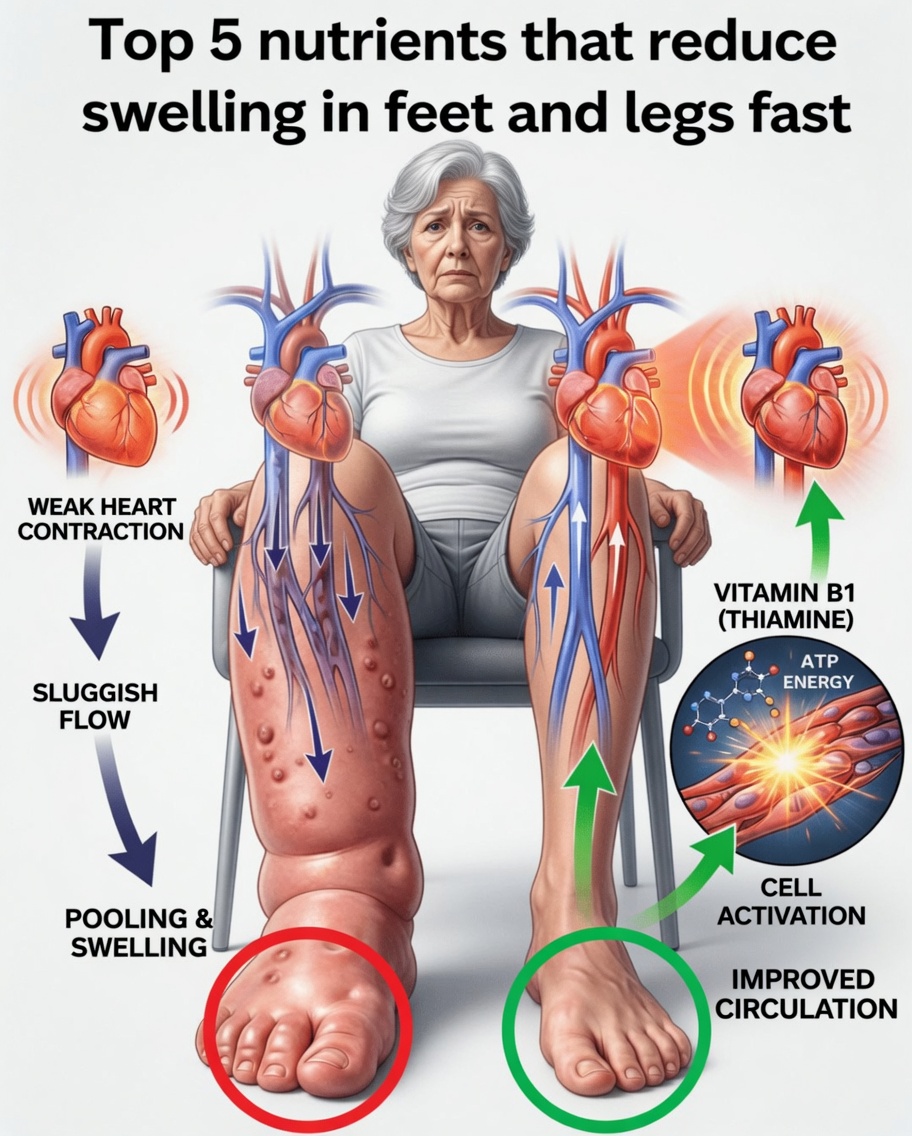
What Is Swelling in the Feet and Legs (Edema)?
Swelling in the lower body—often called edema—occurs when extra fluid collects in tissues, most commonly in the feet, ankles, and lower legs. It may show up after long hours of sitting or standing, but it can also be linked to broader factors such as circulation issues or inflammation.
Supporting the body with targeted nutrition may help address some of the underlying contributors to swelling in feet and legs.

Common Lifestyle Causes of Swelling in Feet and Legs
Daily routines can strongly influence fluid buildup in the lower extremities. Some of the most frequent contributors include:
- Long periods of sitting or standing, which increase pressure in leg veins and make upward blood flow more difficult
- Excess body weight, which adds strain to the circulatory system
- High-sodium diets, which can encourage water retention
- Processed-food patterns, which may lead to nutrient gaps that make swelling worse over time

The Top 5 Nutrients That May Reduce Swelling in Feet and Legs
Studies and clinical observations point to several nutrients that may support circulation, vessel health, inflammation balance, and fluid regulation—all key areas involved in edema.

1. Omega-3 Fatty Acids (EPA and DHA)
Omega-3s, especially EPA and DHA, are widely recognized for helping the body maintain a healthy inflammatory response. When inflammation contributes to swelling in the feet and legs, adequate omega-3 intake may support more comfortable mobility and healthier fluid dynamics.
Many people fall short on omega-3s through food alone, which may be one reason swelling persists.
Best food sources include:
- Fatty fish: salmon, mackerel, sardines, herring
- Plant sources: flaxseed, chia seeds (note: conversion to EPA/DHA is limited)
Higher omega-3 intake is also associated with cardiovascular support, which may indirectly benefit lower-leg comfort.

2. Potassium
Potassium plays a central role in electrolyte and fluid balance. When potassium is low, the body may retain more sodium and water, increasing the likelihood of swollen feet and legs—often felt as heaviness or tightness.
Improving potassium intake through whole foods can help support natural fluid movement.
Potassium-rich foods:
- Avocados
- Sweet potatoes and white potatoes
- Spinach and other leafy greens
- Bananas and beets
For best results, include a mix of potassium foods across meals rather than relying on just one source.

3. Vitamin D
Vitamin D supports multiple systems involved in swelling, including blood vessel function and inflammation regulation. Low vitamin D status has been observed in some people who experience swelling in the feet and legs, and deficiency is linked in research to broader circulation challenges.
Maintaining healthy vitamin D levels—through safe sunlight exposure and diet—may support vascular comfort.
Natural sources of vitamin D include:
- Fatty fish: salmon, tuna
- Egg yolks (often higher in pastured eggs)
- Fortified foods
- Mushrooms exposed to sunlight

4. Vitamin C
Vitamin C is essential for making collagen, a structural protein that helps keep blood vessels strong and resilient. When vessel walls are weaker, fluid may leak more easily into surrounding tissues, contributing to swelling in feet and legs.
Vitamin C also functions as an antioxidant, supporting the body’s response to oxidative stress and inflammation.
Top vitamin C foods:
- Citrus fruits: oranges, grapefruit
- Bell peppers (especially red and yellow)
- Strawberries, kiwi, broccoli
Regularly eating vitamin C–rich produce can help support vessel integrity over time.

5. Vitamin B1 (Thiamine)
Thiamine (vitamin B1) helps convert food into energy and supports nerve function and heart health—all relevant to healthy circulation. In more significant deficiency states, circulation can be affected, potentially contributing to fluid buildup and swelling in the lower limbs. Research has also identified thiamine deficiency in some people experiencing heart-related edema.
Good thiamine sources include:
- Pork and fish
- Seeds: sunflower, flax
- Legumes, whole grains, and nutritional yeast
Consistent intake may support efficient energy metabolism and circulatory function.
Simple Daily Habits That Can Support Comfort
Nutrition works best when paired with practical routines that reduce fluid pooling:
- Elevate your legs above heart level for 15–20 minutes, a few times daily
- Stay gently active with walking, ankle circles, or light stretching
- Wear comfortable, non-restrictive shoes
- Cut back on high-sodium processed foods
These steps, combined with nutrient-dense meals, may help your legs feel lighter and less tight.
Conclusion: Small Nutrition Shifts, Noticeable Relief
Adding more omega-3 fatty acids, potassium, vitamin D, vitamin C, and vitamin B1 through whole foods may support your body’s natural ability to manage swelling in feet and legs. With steady, balanced choices, many people experience better daily comfort.
A practical approach is to start slowly—add one or two nutrient-rich foods each week and track how your body responds.
Frequently Asked Questions
Is swelling in feet and legs always a serious problem?
Mild swelling can be common, especially after long periods of standing, sitting, or hot weather. However, persistent, worsening, sudden, or one-sided swelling should be discussed with a healthcare professional to rule out underlying conditions.
How long does it take for diet changes to help with swelling?
Response time varies. Some people notice changes within a few weeks when consistent nutrition improvements are combined with supportive habits like movement and leg elevation.
Should you use supplements for these nutrients?
Whole foods are generally the best foundation. If you suspect a deficiency (especially vitamin D or thiamine), consider speaking with your clinician about testing and personalized supplementation.