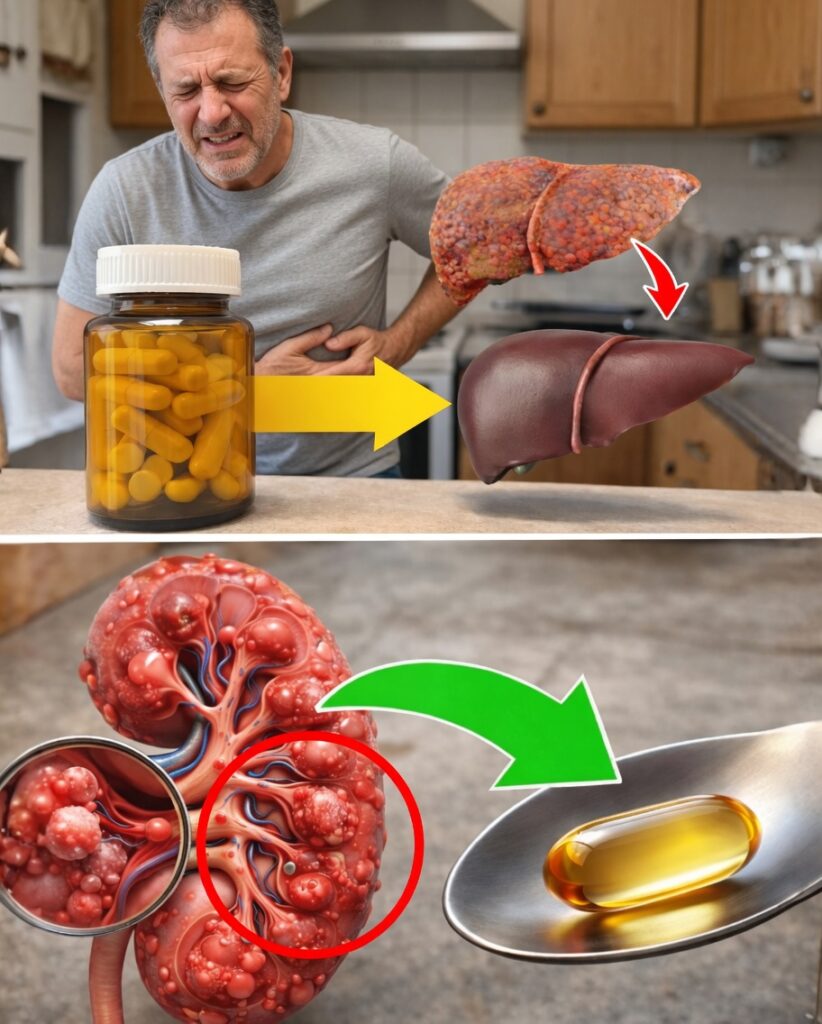
Many people add vitamins and supplements to their routine to support overall wellness, assuming they’re automatically safe. Yet when taken in large doses—or without the right guidance—certain products can place extra workload on key organs, especially the liver and kidneys, and may cause problems that only appear over time. With so much mixed advice online, it’s easy to feel unsure. A clearer understanding of how supplements affect these organs can help you choose more wisely. Stay with this guide to the end for a simple, surprising strategy that can reshape how you manage your supplement stack.
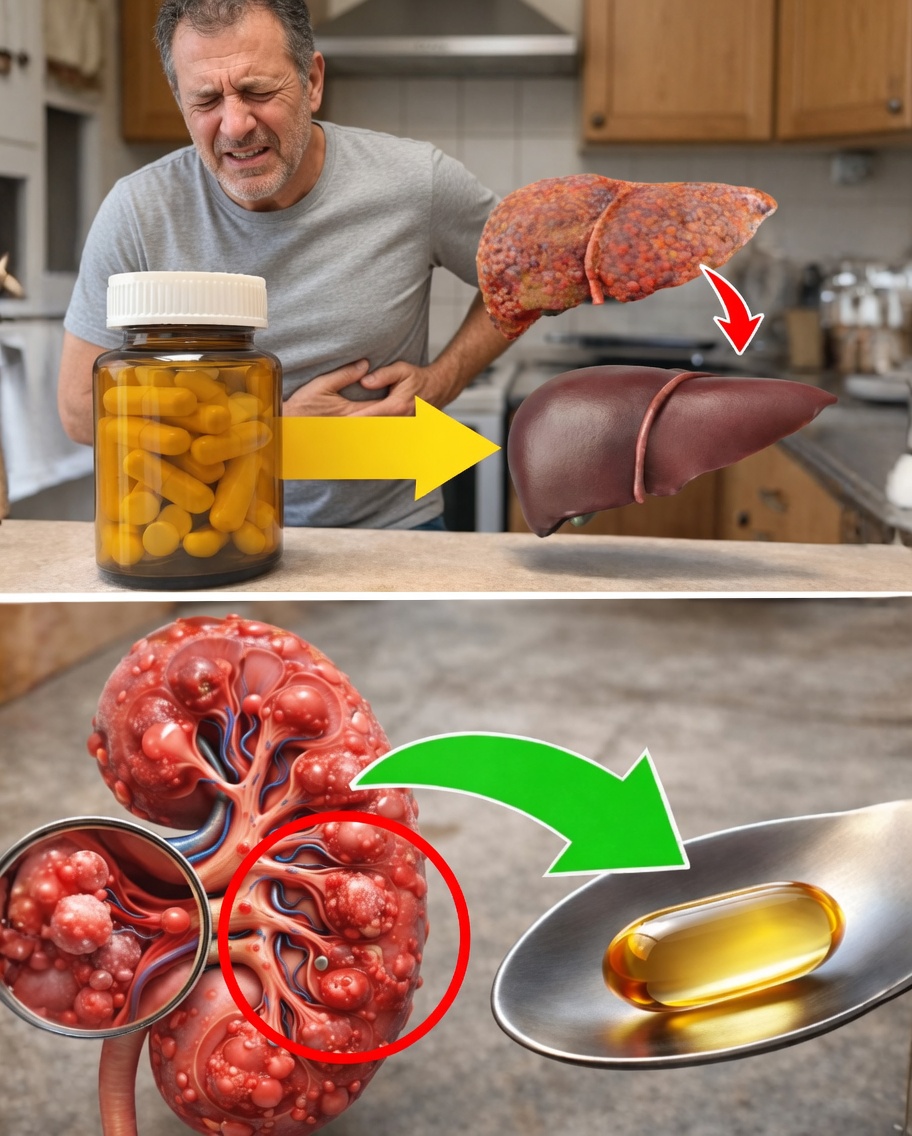
How Supplements Affect the Liver and Kidneys
Your body relies heavily on the liver and kidneys to process what you consume, including vitamins, minerals, herbs, and concentrated extracts.
- The liver helps break down compounds, transform them into usable forms, and prepare them for elimination.
- The kidneys maintain fluid and electrolyte balance while filtering waste products from the blood.
A key point: some nutrients are fat-soluble, which means they can be stored in body tissues rather than easily excreted. In certain situations—especially with high-dose supplementation—this storage can lead to build-up and increased stress on detoxification and filtration pathways.
Research and safety alerts from health organizations have noted that excessive intake of specific nutrients and botanical extracts may affect liver enzymes, kidney workload, or metabolic balance. This is not meant to discourage responsible supplement use—many products are helpful when used appropriately—but to highlight why dose, duration, and individual health status matter.
Your risk also depends on personal factors such as:
- Age
- Pre-existing liver or kidney conditions
- Medication use (and interactions)
- Genetics and metabolism
- Overall diet and hydration habits
Next, let’s look at specific supplements commonly discussed in connection with liver and kidney concerns.
9 Vitamins and Supplements to Use with Extra Caution
The following examples have been associated in studies or case reports with potential liver or kidney issues—typically in high doses, concentrated extracts, or susceptible individuals. Responses vary widely, so always speak with a qualified healthcare professional before starting, stopping, or combining supplements.
1. Vitamin A
Vitamin A supports vision, immune defense, and cell growth. Because it is fat-soluble, supplemental forms can accumulate—particularly in the liver—when taken in excess. Some evidence links high-dose vitamin A supplements (more than food sources) to liver stress.
- Why caution matters: possible liver accumulation; potential imbalance issues if intake is excessive.
- Safer approach: stay near the adult RDA (roughly 700–900 mcg per day). If pregnant or concerned about liver health, consider beta-carotene from plant foods, which the body converts as needed.
2. Vitamin D
Vitamin D is essential for calcium regulation and bone health, but too much supplementation can raise calcium levels, potentially increasing kidney strain. Some reports also note indirect metabolic effects that may influence liver markers in certain contexts.
- Why caution matters: excess vitamin D can contribute to high calcium, which may burden kidneys.
- Safer approach: consider a blood test before supplementing. Typical guidance is 600–800 IU/day unless your clinician recommends a different dose based on lab results.
3. Niacin (Vitamin B3)
Niacin supports energy metabolism, but higher-dose niacin (sometimes used for cholesterol management) has been associated with changes in liver enzymes in some studies. Kidney concerns may arise when intake is far above need, especially over time.
- Why caution matters: high doses may affect liver function markers.
- Safer approach: do not self-prescribe high doses. For everyday nutrition, rely on food sources (such as poultry and nuts) or standard multivitamin-level dosing unless medically directed.
4. Iron
Iron is crucial for oxygen transport and is often used for anemia. However, iron is not a “more is better” nutrient. Excess iron can accumulate, potentially contributing to oxidative stress—particularly in the liver—and may worsen issues in people with certain conditions.
- Why caution matters: iron overload can stress the liver; may complicate kidney issues in vulnerable individuals.
- Safer approach: supplement only with confirmed deficiency from bloodwork. General daily needs are often cited as around 18 mg for many women and 8 mg for many men, but individual needs vary.
5. Green Tea Extract
Green tea is widely used for antioxidant support, but concentrated green tea extracts (high in catechins such as EGCG) have been linked in some reports to liver-related concerns at high intakes, particularly in supplement form.
- Why caution matters: highly concentrated catechins may be harder on the liver in some people.
- Safer approach: brewed green tea is typically gentler than extracts. If using supplements, keep EGCG intake conservative (commonly suggested limits are under ~300 mg EGCG/day).
6. Turmeric (Curcumin)
Turmeric is valued for its anti-inflammatory properties, yet high-dose curcumin supplements may cause liver-related issues in sensitive individuals. Kidney concerns are less commonly reported but could occur depending on dose, duration, and individual factors.
- Why caution matters: high supplemental doses may increase liver processing demands in some users.
- Safer approach: use turmeric in food for routine support. If supplementing, choose reputable products and avoid extreme dosing (commonly around 500 mg/day unless professionally advised).
7. Ashwagandha
Ashwagandha is often used for stress and sleep support. Some reports associate it with elevated liver enzymes in a subset of users, especially with prolonged or high-dose use.
- Why caution matters: possible liver sensitivity in certain individuals.
- Safer approach: consider cycling (for example, several weeks on, then a break) and discontinue if unusual symptoms appear. Discuss with a clinician if you have underlying liver concerns.
8. Kava
Kava is used for relaxation and anxiety support, but it has been linked to serious liver toxicity in certain preparations and situations. While kidney effects are less emphasized, any supplement with known liver risk deserves careful evaluation.
- Why caution matters: documented potential for liver injury, depending on product type and individual factors.
- Safer approach: avoid mixing with alcohol or hepatotoxic medications. If used, prioritize quality-controlled products and limit duration.
9. Black Cohosh
Black cohosh is commonly taken for menopausal symptoms. Some users have reported liver-related issues, though the exact mechanism and individual susceptibility remain debated.
- Why caution matters: potential liver concerns in certain individuals.
- Safer approach: use standardized products, follow label directions, and consider periodic breaks rather than continuous long-term use.

Safe Ranges vs. Higher-Risk Intake (General Guide)
Below is a simplified overview based on common recommendations and reported concerns. These are general references, not personalized medical advice.
| Supplement | Typical Daily Amount (General) | Potential Concern at High Intake |
|---|---|---|
| Vitamin A | 700–900 mcg | Liver accumulation |
| Vitamin D | 600–800 IU | Elevated calcium and kidney strain |
| Niacin (B3) | 14–16 mg | Liver enzyme changes at high doses |
| Iron | 8–18 mg | Oxidative stress, possible overload |
| Green Tea Extract | <300 mg EGCG | Liver stress in concentrated doses |
| Turmeric/Curcumin | ~500 mg | Processing strain in sensitive users |
| Ashwagandha | ~300 mg | Possible liver enzyme elevation |
| Kava | Short-term only | Liver toxicity risk |
| Black Cohosh | As directed | User-specific liver reactions |
How to Support Liver and Kidney Health While Using Supplements
If you use supplements, the goal is not perfection—it’s sustainability and risk reduction.
- Prioritize food first: a varied diet (vegetables, fruit, legumes, whole grains, lean proteins) naturally balances nutrient intake.
- Choose quality-tested products: look for third-party verification (such as USP or NSF) when possible.
- Avoid overlap: multiple products can contain the same vitamins/minerals, unintentionally pushing you into high-dose territory.
- Hydrate consistently: adequate water intake supports kidney filtration.
- Exercise regularly: movement supports metabolic health, which can reduce strain on detox and elimination pathways.
Key Takeaways
Being cautious with these nine supplements does not mean avoiding them entirely. It means focusing on:
- Appropriate dosing
- Reliable product quality
- Awareness of your personal health context
- Professional guidance when needed
The unexpected strategy mentioned earlier: schedule a “supplement audit” every six months with your clinician or pharmacist. Reviewing your full stack—supplements, fortified foods, and medications—often reveals hidden duplication, unnecessary products, or safer alternatives.
FAQ
What if I think a supplement is affecting my health?
Stop the suspected product (unless a clinician has told you not to), track symptoms such as fatigue, nausea, itching, dark urine, or digestive changes, and contact a healthcare professional for evaluation and appropriate testing.
Are “natural” supplements always safer?
No. Natural ingredients can be potent, variable in concentration, and sometimes contaminated or mislabeled. Safety depends on dose, quality, interactions, and your health status.
How can I get nutrients without supplements?
Build meals around diverse whole foods—leafy greens, beans, nuts, seeds, fish or lean proteins, dairy or fortified alternatives, and whole grains—to cover many vitamin and mineral needs.
Educational purposes only. This content does not replace professional medical advice. Always consult a qualified healthcare provider before changing your supplement routine.