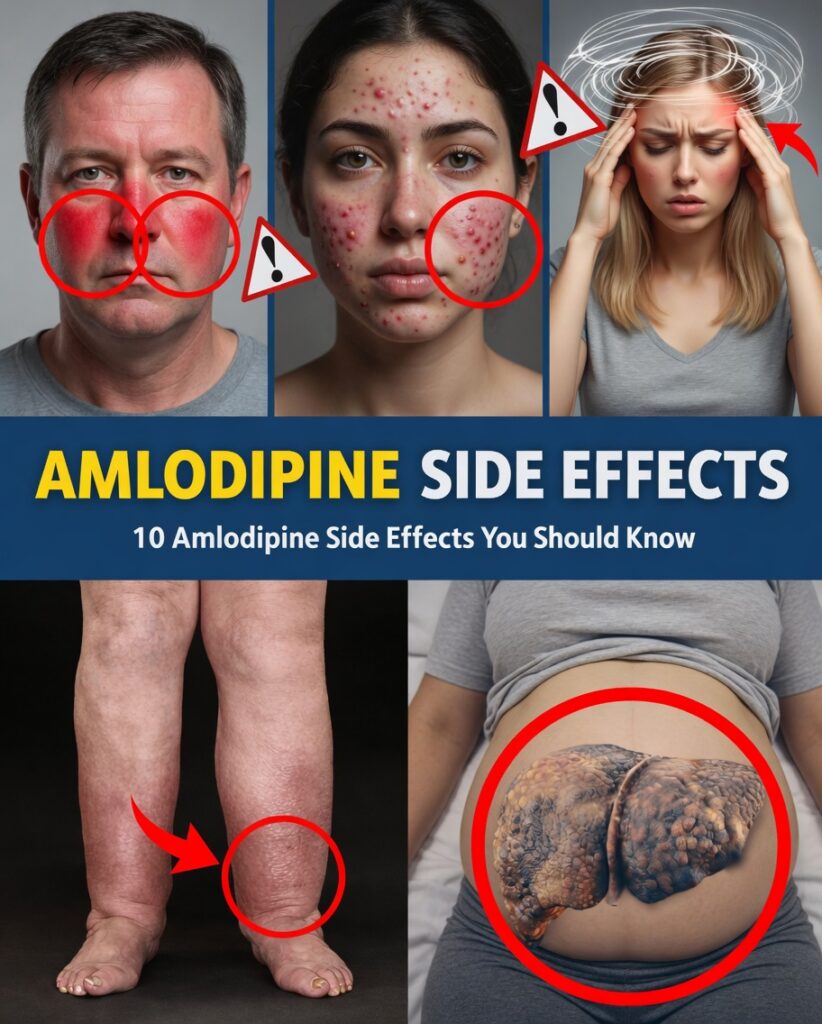
A Quiet Warning Sign Many Patients Miss
Last month, a retired man shared a story I can’t forget. He’d taken his daily blood pressure tablet for years without skipping a dose. Then, almost out of nowhere, his shoes started feeling snug, and his stamina steadily declined. At first, he assumed it was simply “getting older.” But as the swelling worsened and the fatigue began interfering with his daily walks, it became clear something else might be going on.
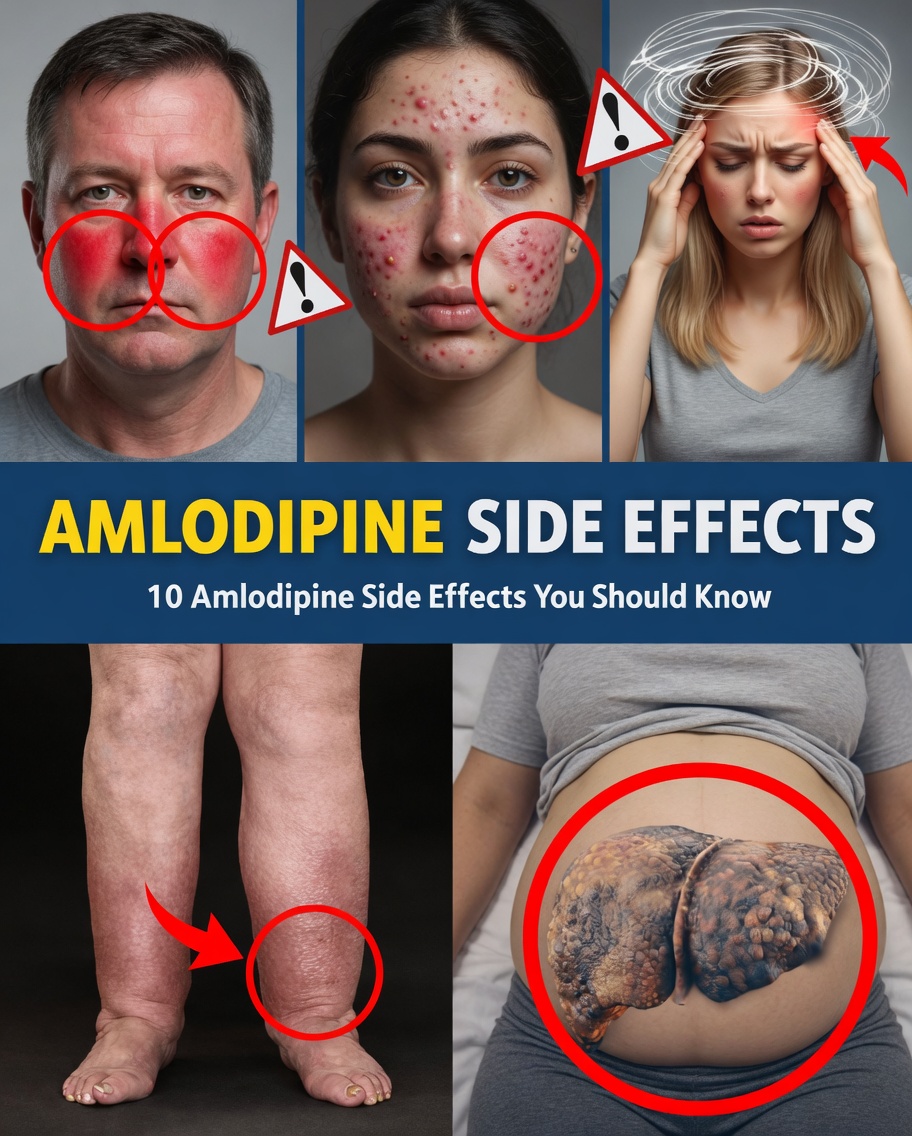
Stories like this are more common than many people realize. The uncomfortable reality is that medication-related changes can be subtle—and easy to overlook. Learning to recognize what your body may be signaling can completely change the quality of the conversation you have with your doctor. One particular sign near the end often surprises even long-term patients.
Why Amlodipine Matters for Adults Over 50
In the United States, many adults over 50 take amlodipine to control high blood pressure and protect cardiovascular health. It’s frequently described in studies as well tolerated. Still, both research and patient experiences show that certain side effects may occur more often than people expect.

The most important takeaway
Recognizing potential side effects is not the same as quitting a medication. The goal is to notice changes early so you and your clinician can review them calmly, adjust if needed, and stay on the safest plan.
Below are some of the most commonly overlooked reactions people report.
1) Swollen Ankles and Legs (Peripheral Edema)
One of the best-known issues is swelling in the feet, ankles, or lower legs—known clinically as peripheral edema.
For many older adults, it begins gradually:
- Shoes feel tighter than usual
- Socks leave deeper indentations
- Walking can feel heavier or more tiring

Cardiovascular research suggests swelling affects a meaningful portion of patients, especially at higher doses.
Why it can happen
Amlodipine relaxes blood vessels to improve blood flow. In some individuals, that relaxation can encourage fluid to shift into surrounding tissues, particularly in the lower legs.
Commonly reported signs include:
- Ankles that look puffy later in the day
- Sudden tightness in footwear
- Legs feeling heavy after standing
In most cases, this swelling isn’t dangerous—but it can reduce comfort and mobility. That’s why many clinicians prefer patients to mention it early rather than “wait it out.”
2) Unexpected Tiredness and Lower Stamina
Have you felt unusually worn out—even after sleeping well?
Some people notice a slow decline in energy after starting or adjusting blood pressure medication. The shift is often subtle:
- Regular walks become shorter or less frequent
- Gardening, errands, or chores feel harder than before
Clinical observations suggest fatigue occurs in a smaller share of users. The exact cause isn’t always straightforward. Blood pressure changes, circulation differences, and personal sensitivity can all contribute.
A key point
Medication-related fatigue can easily be mistaken for normal aging. Tracking your energy level after prescription changes can help your doctor identify patterns sooner.
3) Dizziness or Lightheaded Episodes
Another occasionally reported effect is dizziness, which can be especially important for older adults because balance and fall risk matter more with age.
Patients often describe:
- Brief lightheadedness when standing up
- A mild “spinning” sensation
- Feeling slightly unsteady while walking

Research suggests dizziness appears in a minority of patients, particularly when blood pressure drops more than expected. This doesn’t automatically mean the medication is unsafe—it often means symptoms should be monitored and discussed during follow-ups so treatment can be refined if necessary.
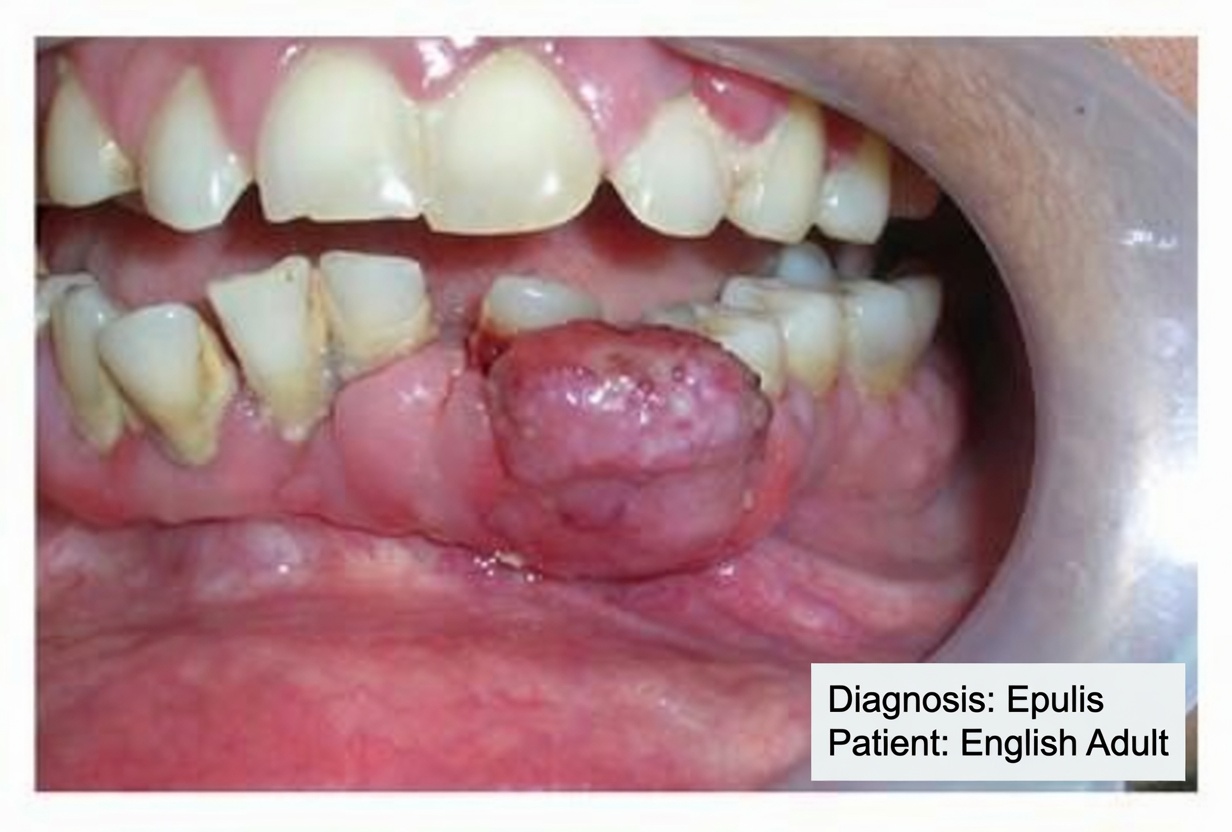
4) Gum Changes That Many People Don’t Expect
This next one surprises a lot of patients: some people using certain blood pressure medications notice gum changes over time. Dentists refer to this as gingival overgrowth.
It may look like:
- Gums appearing thicker around teeth
- Flossing becoming more difficult
- Gum tissue covering more of the tooth surface

Dental studies have documented this effect in a small percentage of people taking certain calcium channel blockers, including amlodipine.
Helpful habits often include:
- Consistent oral hygiene
- Regular cleanings
- Routine dental checkups
- Gentle daily flossing
5) Palpitations and Flushing Sensations
Some patients report episodes where the heart feels like it’s beating harder or faster than usual—known as palpitations. Others notice flushing, such as a sudden warmth or redness in the face that fades after a short time.
Typical descriptions include:
- A warm sensation across the face
- A temporary “pounding” heartbeat
- Sudden facial or skin redness

These experiences are usually brief and not harmful, but they can feel unsettling. Bringing them up during routine visits helps your clinician decide whether monitoring or dosage adjustment is appropriate.
6) Digestive Upset, Muscle Cramps, and Sleep Changes
Medication effects don’t always show up where you expect. Some people report:
- Mild nausea or stomach discomfort
- Muscle cramps (often at night)
- Restless sleep or sleep disruption
Examples include:
- Nighttime leg cramps
- Mild digestive upset
- Restless or lighter sleep
These reactions vary widely. Your age, dose, overall health, and other medications can all influence how your body responds.
Quick Overview of Commonly Reported Effects
- Ankle/leg swelling: puffy feet, tight shoes (more common at higher doses)
- Fatigue: low energy, reduced stamina (often noted by older adults)
- Dizziness: lightheadedness, especially when standing
- Gum changes: thickened gums (more likely with long-term use)
- Palpitations: brief racing or pounding heartbeat (can be dose sensitive)
- Flushing: sudden facial warmth or redness (reported more often by some women)
Practical Steps to Monitor Side Effects (Without Panic)
Many doctors recommend simple habits that make it easier to spot meaningful changes:
- Keep a brief symptom journal (what you felt, when it started, what changed)
- Measure blood pressure regularly as advised
- Report new or worsening symptoms during appointments
- Maintain routine dental visits and cleanings
- Stay hydrated and keep active within your comfort level
These steps don’t replace medical care—they support clearer, more productive conversations with your healthcare provider.
Conclusion: Awareness Beats Fear
Millions of Americans use amlodipine to support healthy blood pressure and heart function. For many, it works well for years with minimal issues. However, quiet signals—like ankle swelling, fatigue, dizziness, or gum changes—can develop gradually.
Noticing these early gives you and your doctor more options and more control over your care plan. The strongest tool isn’t fear—it’s awareness. When you understand what your body is doing, it becomes easier to make confident, informed health decisions.
Frequently Asked Questions
Is ankle swelling from blood pressure medication common?
Ankle swelling is a commonly reported side effect with certain blood pressure medications, including amlodipine. Research suggests it may occur in a noticeable minority of users, especially at higher doses. A doctor can help determine the best next step.
Should I stop amlodipine if I notice side effects?
You should not stop any prescription medication without medical guidance. If side effects appear, contact your healthcare provider so they can evaluate symptoms and review your treatment plan safely.
Are side effects the same for everyone?
No. Response varies based on factors such as age, dosage, overall health, and other medications you may be taking.