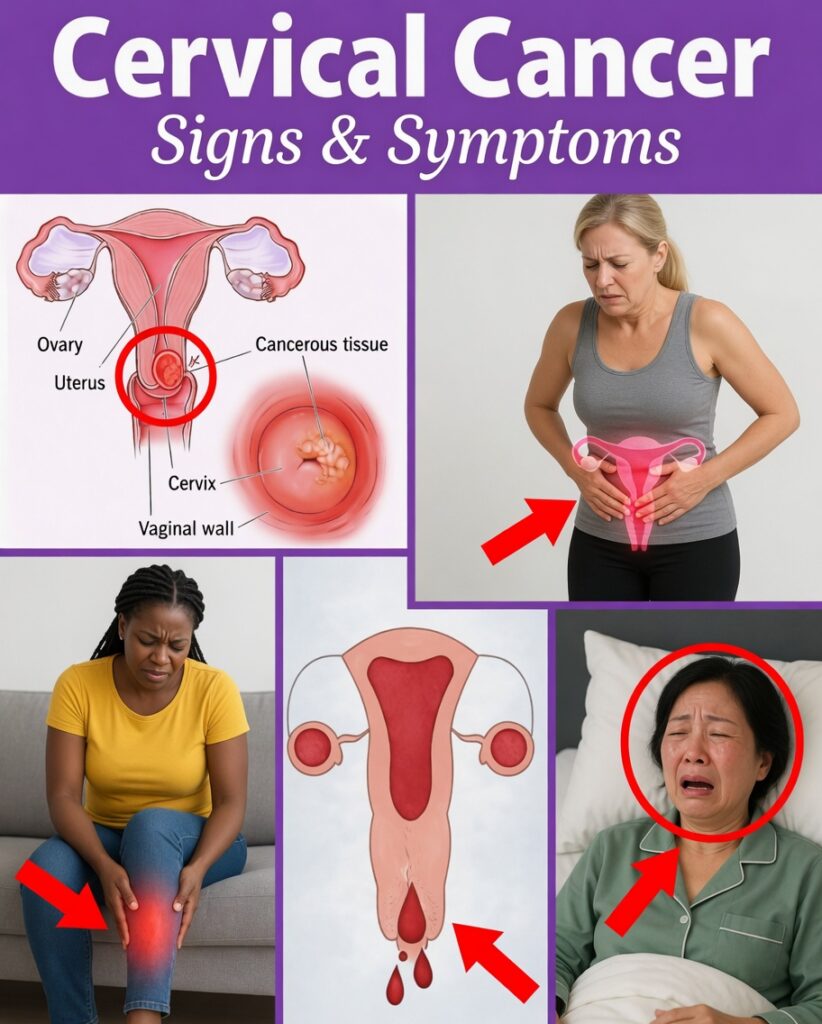
Subtle Early Warning Signs of Cervical Cancer You Should Know
You wake up with a vague sense of discomfort and chalk it up to a hectic schedule. A faint, unfamiliar smell after your morning shower, a sudden twinge while you’re moving through your day, and a quiet question starts to form in the back of your mind: Is something more serious going on with my health?
Moments that should feel ordinary can slowly turn into private worries, especially when you wonder whether these changes could be early warning signs of cervical cancer. The empowering part is this: understanding potential symptoms helps many women speak up sooner, ask clearer questions, and seek timely medical advice.
Recognizing what might be an early warning sign of cervical cancer won’t replace a professional diagnosis, but it can give you enough clarity to take the next step, talk to your doctor, and reclaim some peace of mind.
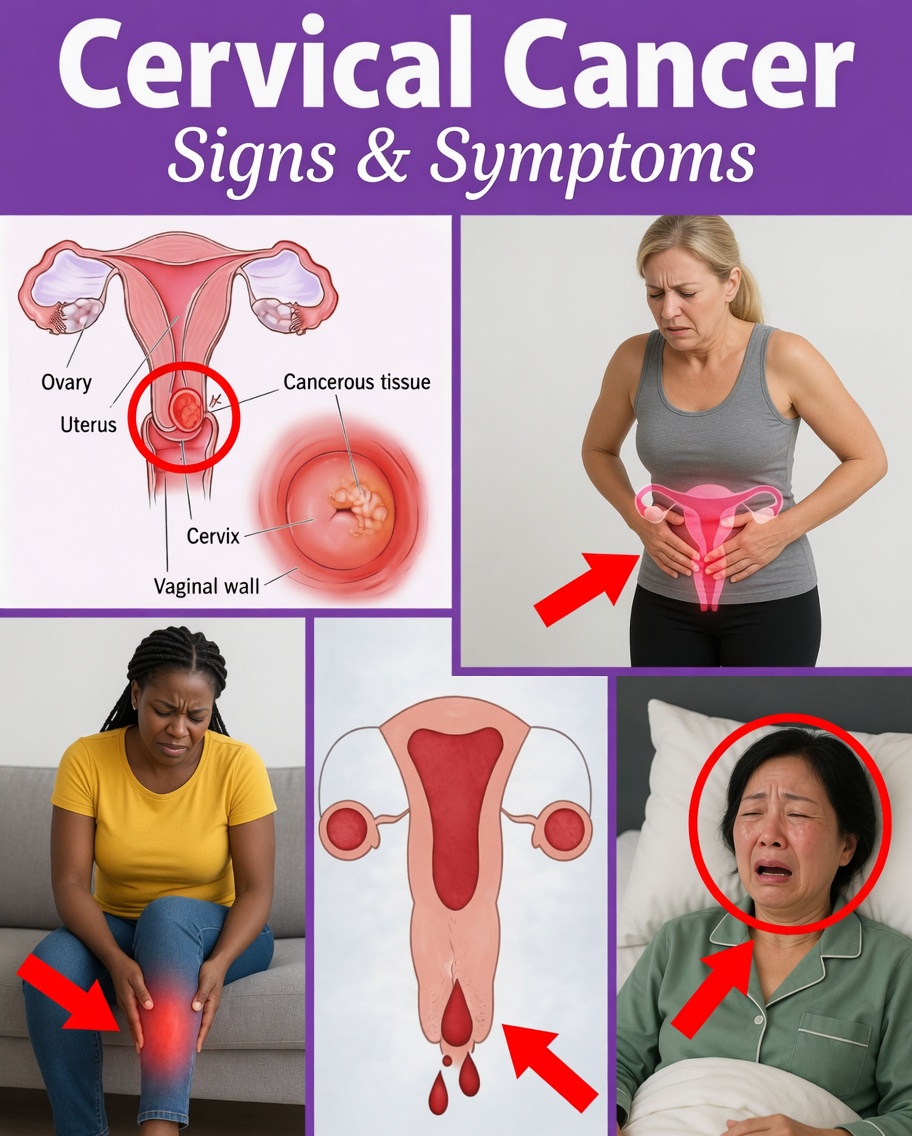
Sign 9: Unusual Vaginal Discharge That Feels Different
Sarah, a 48-year-old teacher from Chicago, first noticed a thin, watery discharge with a slight fishy smell during her evening shower. She felt a familiar knot of anxiety: her body seemed to be changing in ways she couldn’t explain. At first, she blamed hormones, but the persistent sticky texture kept distracting her and quietly raised fears about what this could mean for her future with her children.
Health organizations report that changes in vaginal discharge — becoming more watery, blood-tinged, or noticeably foul-smelling — can sometimes be among the early warning signs of cervical cancer. Yet many women assume it’s stress, perimenopause, or a minor infection and never mention it.
If your discharge suddenly looks, smells, or feels different from your norm and the change doesn’t go away, it’s worth bringing up with your doctor. A short conversation and proper testing can often provide answers and relief.
Sign 8: Pain or Discomfort During Intimacy
Lisa, 52, from New York, felt a sharp, scraping sensation during a romantic evening — as if sandpaper were brushing against sensitive skin. In an instant, she worried that something was threatening the closeness she shared with her partner. She assumed it was just vaginal dryness from aging, but the recurring ache left her anxious, withdrawn, and wondering if it could be connected to cervical changes she was ignoring.
Medical reviews note that pain during sex (dyspareunia) can be linked to inflammation, infections, hormonal shifts, or, in some cases, abnormalities in the cervix. Because it’s so common to blame it solely on “getting older,” many women never realize it could be an early sign of a deeper issue.
If intimacy starts to hurt — especially if it’s new for you or getting worse — it’s not something you need to silently endure. Talking with a healthcare professional can help uncover the cause and, in many cases, restore comfort and emotional ease.
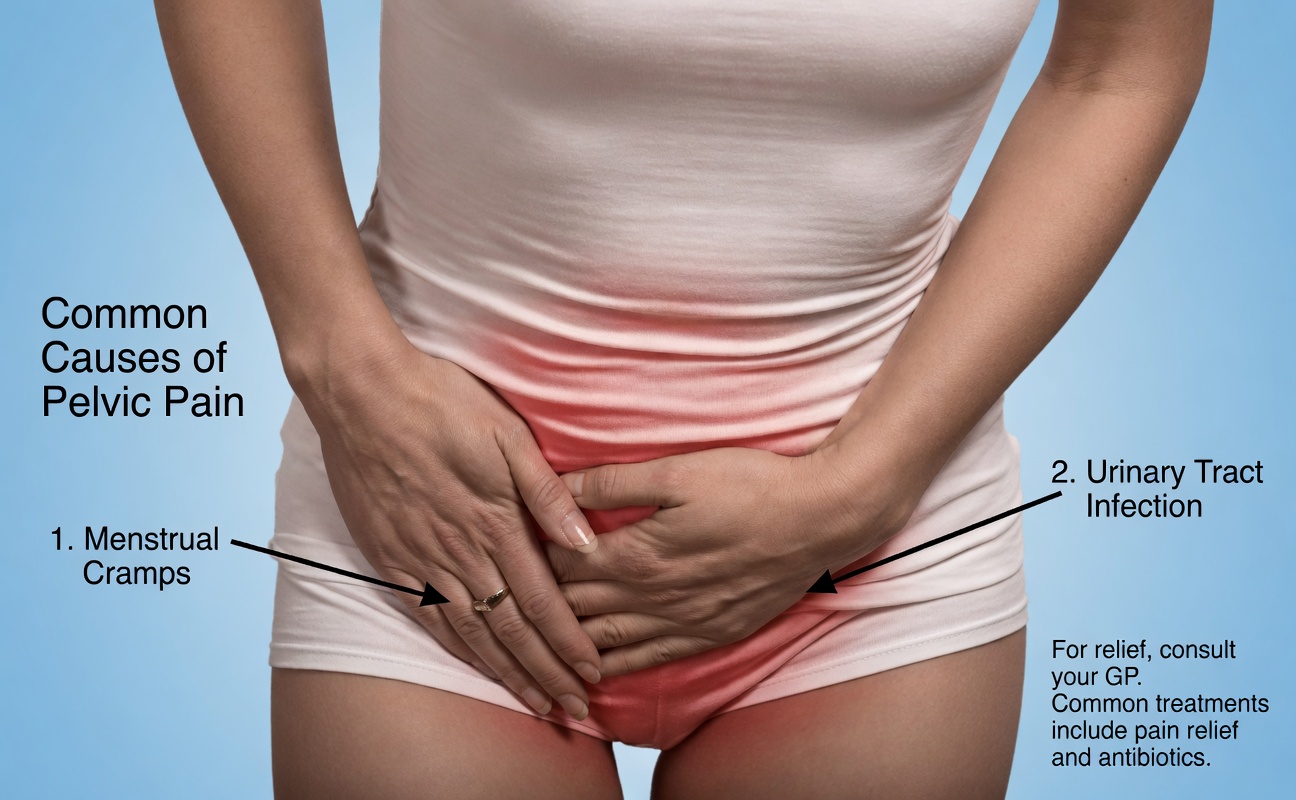
Sign 7: Abnormal Bleeding Between Periods
One afternoon, Emily, 46, from Texas, noticed unexpected blood on her underwear. A wave of fear hit as she wondered if irregular bleeding could be an early warning sign of cervical cancer. She tried to dismiss it as stress or a one-time fluke, but the spotting kept returning, interrupting her routine and quietly feeding her worry about missing precious time with her family.
Trusted health authorities highlight that bleeding between periods, after sex, or after menopause can sometimes be associated with cervical cell changes. While hormonal shifts, fibroids, or other conditions are also common causes, any unusual bleeding pattern deserves attention.
If your cycle suddenly changes — spotting between periods, heavier flows, or bleeding after intercourse — start tracking when it happens and how often. Sharing those details with your doctor can support a faster, more accurate evaluation.

Sign 6: Persistent Pelvic Pain That Lingers
Maria, 50, from California, described a dull, dragging ache low in her abdomen, like carrying a heavy weight after a long day. She assumed it was from overdoing it at yoga, but the constant pressure began to disturb her sleep and drain her energy, leaving her worried that something more serious might be slowly undermining her ability to keep up with her grandchildren.
Clinical research shows that persistent pelvic pain can be related to several conditions — including endometriosis, infections, fibroids, or, in some cases, cervical or other gynecologic cancers. What sets it apart is that the discomfort doesn’t fully go away and gradually affects daily life.
If pelvic pain keeps returning or never really disappears, don’t ignore it or label it “normal.” Early evaluation can rule out many causes, catch potential problems sooner, and help you feel more in control of your health.
Sign 5: Unexplained Fatigue That Drains Your Energy
Anna, 47, from Florida, found herself completely worn out by midday. She pushed through errands with a deep, bone-level tiredness that made even small tasks feel overwhelming. At first she blamed poor sleep or a busy schedule, but the exhaustion kept returning, silently raising questions about whether something in her body — including possible cervical changes — might be contributing.
Studies show that when the body is fighting illness or dealing with chronic changes, fatigue can be an early symptom. This kind of tiredness doesn’t fully improve with rest and may be accompanied by other subtle signs, like weight changes or unusual bleeding.
If you’re constantly exhausted, even after good sleep and lighter days, and especially if it comes with other symptoms, it’s worth mentioning to your doctor. Identifying the cause early can help you protect your energy and your long-term health.

Sign 4: Sudden Weight Loss Without Trying
Rebecca, 49, from Seattle, noticed the number on the scale dropping even though she hadn’t changed her diet or exercise routine. At first it felt like a pleasant surprise, but as her clothes started to hang loosely, excitement shifted to concern. She couldn’t shake the uneasy thought that unexplained weight loss might be a sign something serious was happening inside her body.
Health experts note that unintentional weight loss can sometimes signal underlying conditions, including hormonal issues, digestive problems, or cancers such as cervical cancer in more advanced stages. The key is that the weight comes off without effort — no new workout plan, no deliberate diet changes.
If pounds are slipping away and you don’t know why, especially alongside other symptoms, do not ignore it. Document the changes and discuss them with your healthcare provider so you can address the cause sooner rather than later.
Sign 3: Lower Back Pain That Won’t Quit
Sophia, 51, from Boston, rubbed her aching lower back after sitting at her desk for hours. She assumed poor posture was to blame, but the steady throbbing continued even when she stretched, walked, or lay down. The pain began to interfere with her gardening and her time with loved ones, and she started to wonder if it was more than just a typical backache.
Medical literature notes that ongoing lower back pain can have many causes — muscle strain, spinal issues, or arthritis — but in some cases, it may be linked to pressure from pelvic or cervical changes. The concern rises when the discomfort feels deep, persistent, and doesn’t respond to usual home remedies.
If your lower back pain lingers for weeks, worsens, or appears alongside pelvic discomfort, unusual bleeding, or other symptoms, seek a professional evaluation. You don’t have to live with daily pain without clear answers.

Sign 2: Swelling in the Legs or Feet
Laura, 53, from Atlanta, noticed that by evening her ankles were puffy and her shoes felt tight. She felt self-conscious about the swelling and started covering her legs, wondering if something more serious might be affecting her circulation. She blamed long hours standing at work, but the swelling persisted even on resting days, quietly increasing her concern.
Experts explain that swelling in the legs or feet (edema) can occur for many reasons — vein issues, heart or kidney problems, medications — and in some cases, it can be related to changes in lymphatic drainage due to pelvic or cervical conditions. When swelling is new, persistent, or appears without a clear reason, it should be checked.
If your lower legs or feet regularly swell and the cause isn’t obvious, make a note of when it happens and how severe it is. Sharing that with your doctor can help them determine whether further testing is needed.
Sign 1: Urinary Problems Like Frequent Urges or Burning
Karen, a 45-year-old nurse from Denver, began experiencing sudden, urgent needs to urinate, often accompanied by a burning sensation. These episodes disrupted her shifts, forced her to run to the restroom repeatedly, and left her feeling overwhelmed and isolated. She initially assumed it was just another urinary tract infection, but treatment didn’t fully resolve the symptoms, and the worry that something deeper might be wrong started to grow.
Urinary changes — such as needing to go more often, feeling urgency, pain or burning when urinating, or difficulty emptying the bladder — are commonly caused by infections or bladder conditions. In some cases, especially when persistent and combined with other symptoms like pelvic pain or abnormal bleeding, they may also be associated with cervical or other pelvic issues.
If urinary problems keep returning or don’t improve with standard treatment, it’s important to follow up. Ask for a more thorough evaluation rather than repeatedly assuming it’s “just another UTI.”

Moving Forward: Listening to Your Body and Taking the Next Step
Many of these signs — unusual discharge, pain during sex, irregular bleeding, pelvic or back pain, fatigue, weight loss, swelling, or urinary changes — can be caused by conditions that are not cancer. But when something feels “off” and persists, your body is asking for attention.
Noticing patterns, writing down symptoms, and scheduling a check-up are powerful steps you can take today. Early detection of cervical changes, especially through regular screening like Pap tests and HPV tests as recommended by your doctor, can make a significant difference in outcomes.
You know your body better than anyone. If something doesn’t feel right, trust that instinct, ask questions, and seek professional guidance — you deserve clarity, reassurance, and a plan that supports your long-term health.