Insulin Resistance May Be More Than a Blood Sugar Problem
You may have already tried the standard advice for insulin resistance: reducing carbohydrates, tracking calories, and exercising consistently. Yet despite your efforts, the fatigue remains, weight loss feels painfully slow, and your energy never seems to recover. That experience can be discouraging, especially when even ordinary daily activities begin to feel draining.
There is, however, a promising shift in how we understand insulin resistance. Newer insights suggest the issue may go deeper than diet alone and involve what is happening inside your cells. More specifically, your mitochondria—the tiny structures responsible for cellular energy—may play a major role in why insulin resistance can feel so difficult to overcome.

Why Insulin Resistance Is Not Just About Sugar or Overeating
Insulin resistance is often framed as a simple result of eating too much sugar or consuming excess calories. While those factors can matter, they do not explain the full picture. Current research indicates that insulin resistance is also connected to how effectively your cells convert available fuel into usable energy.
When that energy system is impaired, your body may struggle even if you are making healthy choices. In other words, insulin resistance can persist not only because of what you eat, but because your cells are not processing fuel efficiently. This is one reason many people feel tired, heavy, and stuck despite following conventional recommendations.
Mitochondria: The Cellular Batteries Behind Energy
Mitochondria are often described as the power plants of the cell, but it may be even more useful to think of them as biological batteries. They help store and release energy in a controlled way so your body can function smoothly throughout the day.
When mitochondrial function declines, insulin resistance can become more pronounced. Glucose may remain in the bloodstream instead of being converted into energy inside the cells. The result is a frustrating combination of low energy, poor stamina, and difficulty maintaining a healthy weight.
For many people with insulin resistance, this helps explain why caffeine only masks the problem rather than solving it. The real issue may be that the body is not generating energy efficiently at the cellular level.
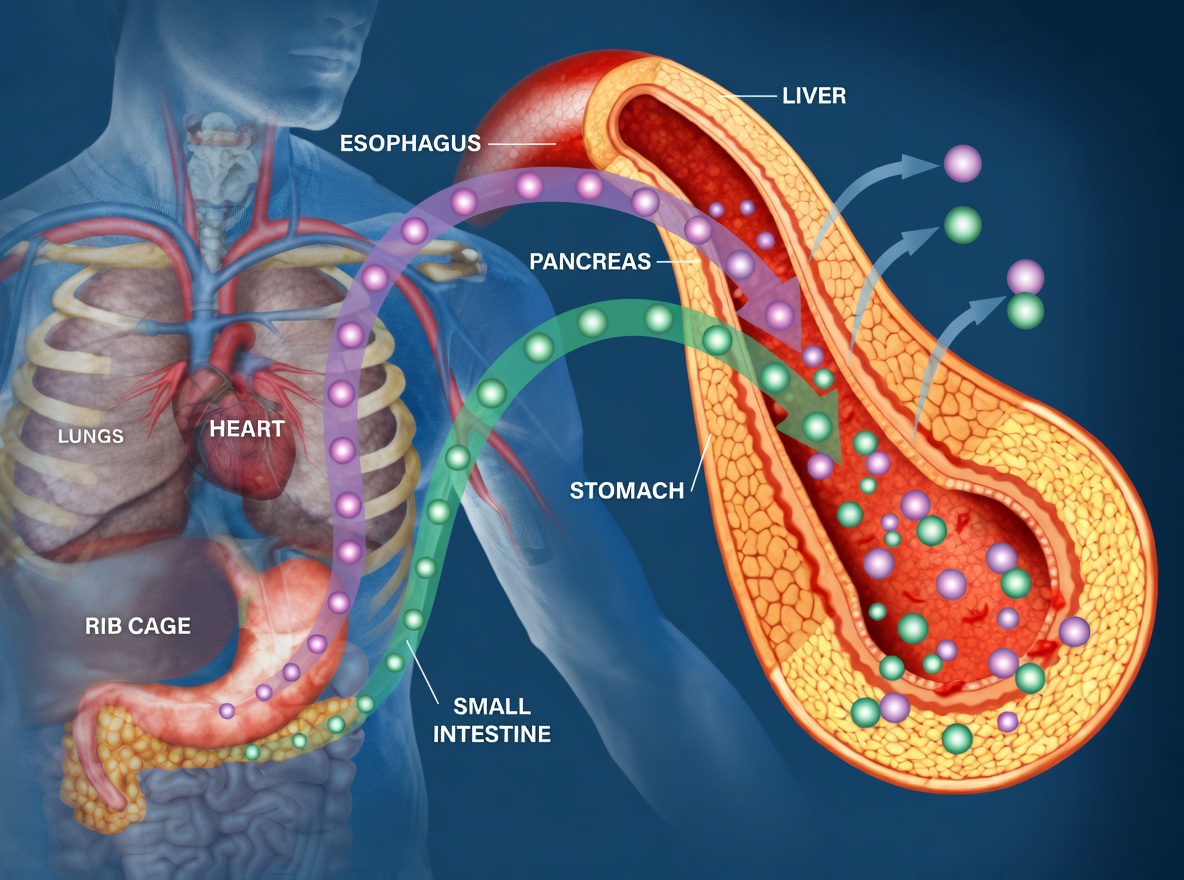
How Mitochondrial Dysfunction Can Lead to Fatigue and Weight Gain
One of the most common complaints in insulin resistance is feeling exhausted all the time while also struggling with stubborn body fat. Mitochondrial dysfunction may help connect these two symptoms.
If mitochondria are not working well, glucose is less likely to be used properly for energy. That unused fuel can contribute to fat storage, while your cells remain underpowered. This creates a difficult cycle: your body stores more energy than it can effectively burn, and you feel increasingly drained in the process.
That is why insulin resistance can make even simple health goals feel harder than they should. Your system is trying to function with weakened cellular energy production.
Inflammation: The Hidden Loop That Makes Insulin Resistance Worse
Inflammation is another important piece of the puzzle. When mitochondria are under stress, they can trigger inflammatory processes that further reduce insulin sensitivity. This creates a self-reinforcing cycle in which mitochondrial strain worsens insulin resistance, and insulin resistance places even more pressure on the mitochondria.
Poor nutrition can make this worse, especially when the body lacks key vitamins and minerals or relies too heavily on low-quality fats. These factors may damage mitochondrial membranes and increase oxidative stress, which further interferes with healthy energy production.
This ongoing loop helps explain why lifestyle changes sometimes seem ineffective at first. If inflammation and mitochondrial stress are not addressed, progress may feel slow or inconsistent.
Why Nutrient Density Matters More Than Calories Alone
Counting calories may help in some situations, but it often does not go far enough for insulin resistance. Mitochondria require specific nutrients to function well, and when those nutrients are missing, energy production can suffer.
Important nutrients for mitochondrial support include:
- B vitamins
- Magnesium
- Copper
- High-quality saturated fats
These compounds help maintain what some experts describe as mitochondrial “voltage,” or the ability of your cells to generate and transfer energy efficiently. If you are deficient in these nutrients, insulin resistance may worsen quietly in the background, even if your calorie intake looks reasonable on paper.
Choosing nutrient-dense foods can give your cells the raw materials they need to work better and may reduce some of the daily burden associated with insulin resistance.
The Emerging Quantum Perspective on Mitochondria
An especially fascinating area of research looks at mitochondria through the lens of quantum mechanics. Scientists are exploring how mitochondria may rely on proton tunneling, an ultra-efficient process involved in producing cellular energy.
In insulin resistance, this highly refined mechanism may become disrupted. When energy generation starts to break down at such a deep biological level, symptoms like fatigue, poor focus, and brain fog may become even more noticeable.
While this science is still evolving, it highlights an important idea: insulin resistance may be far more complex than surface-level issues like sugar intake alone.

Mitochondrial Biogenesis: Building New Cellular Energy Capacity
One encouraging concept is mitochondrial biogenesis, which refers to the creation of new mitochondria. Supporting this process may help your body respond better to insulin resistance by improving cellular energy capacity over time.
Several strategies may help stimulate mitochondrial renewal:
- Exercise at a moderate intensity after an overnight fast.
- Use intermittent fasting windows of around 12 to 18 hours several times per week.
- Prioritize nutrient-rich meals during your eating periods to help rebuild cellular function.
These approaches may encourage your body to create healthier, more efficient mitochondria. Over time, that may help reduce some of the fatigue and metabolic stress linked to insulin resistance.
Pattern Interrupts: A Smarter Alternative to Constant Restriction
Many people approach insulin resistance with nonstop dieting, but endless restriction can sometimes backfire. A more effective strategy may be to use what could be called “pattern interrupts.”
This means changing your routine in a deliberate way to challenge and strengthen mitochondrial function. Examples include:
- Alternating fasting days with regular eating days
- Using short low-carb phases
- Adding occasional fasted workouts
The body often responds well to variation. Instead of forcing the same rigid plan every day, strategic changes can keep your cellular energy systems more adaptable. This may help break the frustrating plateaus that are so common with insulin resistance.
Nutrients and Supplements That May Support Mitochondria
If insulin resistance has left you feeling depleted, targeted nutritional support may help. Key nutrients that are often highlighted for mitochondrial health include:
- Magnesium: around 500 to 800 mg daily
- Copper from whole food sources
- B vitamins
- Quality saturated fats such as those found in coconut oil or grass-fed butter
These nutrients may help stabilize mitochondrial membranes and support smoother energy flow. In turn, this may address one of the foundational issues involved in insulin resistance rather than focusing only on symptoms.
Red Light Therapy and Sauna for Gentle Mitochondrial Support
Red light therapy, near-infrared light, and sauna use are increasingly being discussed as supportive tools for mitochondrial function. These therapies appear to place mild, beneficial stress on the body, which may help mitochondria adapt and work more effectively.
Some people notice gradual improvements in energy when they include these practices regularly. While they are not magic solutions, they can be a simple, low-effort addition to a broader insulin resistance strategy.
Why Your Eating Window Matters
Frequent snacking or constant grazing can place a continual demand on your mitochondria. Over time, this may worsen insulin resistance and contribute to the familiar cycle of energy highs and crashes.
A more supportive approach may be to eat within a defined daily window, such as 7 AM to 7 PM, and include one or two longer fasting periods each week. Giving your body a break from digestion may allow mitochondria time to recover and function more efficiently.
This kind of structure can support better metabolic balance without requiring an extreme or unsustainable diet.

A New Way to Think About Insulin Resistance
Insulin resistance does not have to feel like a never-ending struggle. Looking beyond calories and carbohydrates to support mitochondrial health may offer a more complete and practical path forward. Nutrient-dense meals, well-timed fasting, exercise, and gentle therapies like red light or sauna may all help your cells produce energy more effectively.
Small, steady steps can make a meaningful difference. By giving your cellular “batteries” what they need, you may begin to feel more energized, more resilient, and better able to support a healthier metabolism.
Frequently Asked Questions
How are mitochondria connected to insulin resistance?
Mitochondria generate energy for your cells. When they are not functioning well, your body may struggle to use fuel efficiently, which can contribute to insulin resistance, fatigue, and difficulty managing weight.
What are some simple ways to support mitochondria with insulin resistance?
Start with nutrient-dense foods, structured intermittent fasting, and consistent movement. Some people also benefit from adding red light therapy or sauna sessions as part of their routine.
Can exercise alone reverse insulin resistance by improving mitochondria?
Exercise is valuable, but it may work best when combined with nutrient support and smart fasting strategies. Together, these habits may better encourage mitochondrial biogenesis and provide stronger long-term support for insulin resistance.