The Scary Discovery Many Parents Dread
You part your child’s hair and spot a red, ring-shaped patch on the scalp—plus hairs that look like they’ve snapped off near the root. It’s instantly alarming. Questions race through your mind: Is this dangerous? Will it spread? Did I miss something earlier? Feeling worried (or even a little guilty) is common, especially when your child is uncomfortable.
The good news: in many cases, there’s a clear explanation and a safe, effective path to treatment—without panic. The sections below cover what’s most likely happening and what to do next.

Why a Red Ring Appears and Hair Breaks Off
A circular red scalp patch paired with hair breakage is most commonly linked to a fungal infection of the scalp, widely known as scalp ringworm. Despite the name, it has nothing to do with worms. It’s caused by fungi that tend to multiply in warm, humid conditions, and children are more susceptible because their immune defenses are still developing.
Here’s why the symptoms look so specific:
- Redness happens because the body creates inflammation around the infected area.
- Hair breaks because the fungus weakens the hair shaft close to the scalp, so strands snap off rather than shedding normally.
Understanding this pattern helps you respond calmly and avoid unnecessary fear.
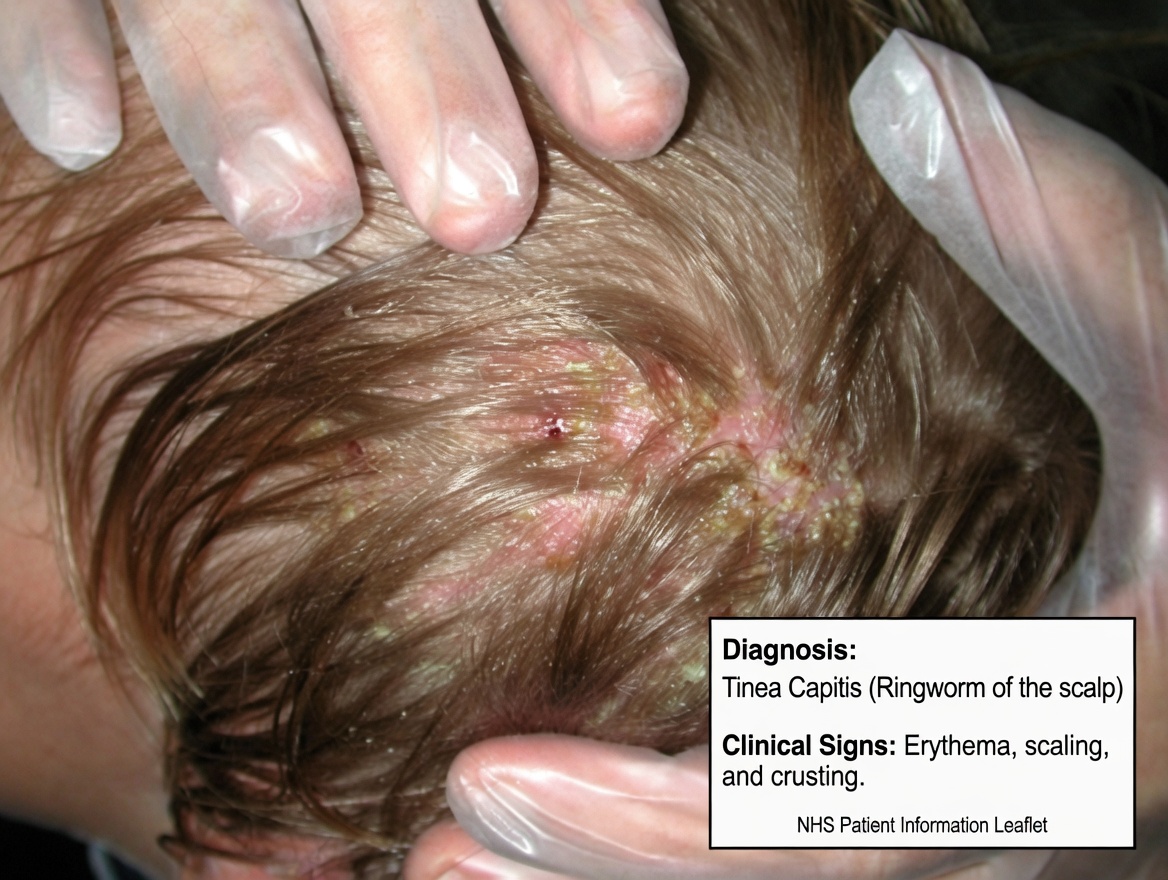
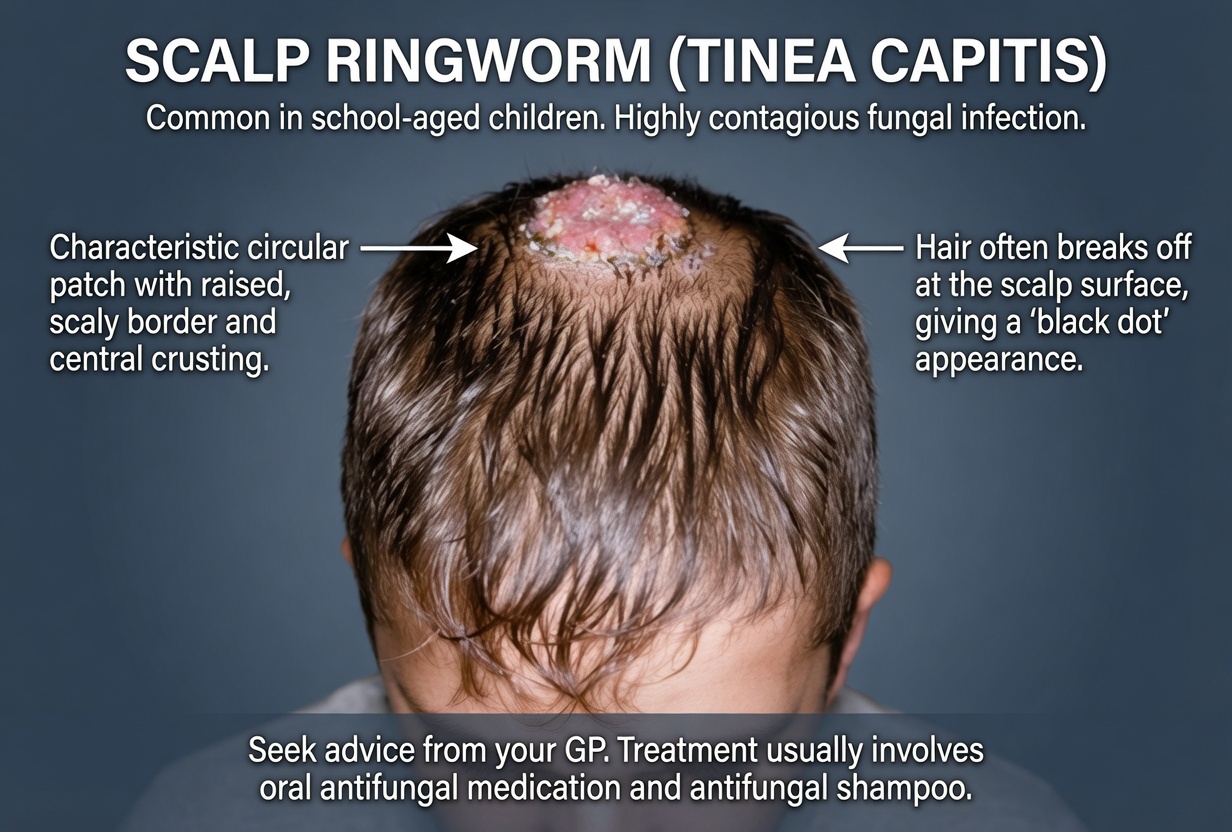
Identifying Scalp Ringworm (Tinea Capitis)
The medical term for scalp ringworm is tinea capitis, and it’s one of the most frequent scalp infections in school-age children. It spreads easily through everyday contact, including:
- Direct skin-to-skin contact with someone infected
- Contact with pets that carry fungal organisms
- Sharing items such as hats, combs, brushes, hair clips, or hair ties
- Using contaminated hair tools
Common signs parents notice include:
- Round, red patches that may look scaly
- Itching or a mild burning sensation
- “Black dots” where hair has broken off at the scalp
- Patchy thinning or visible bald spots
Because it can move quickly through classrooms, sleepovers, and playgrounds, early recognition helps protect other children as well.

How to Tell Ringworm Apart from Other Scalp Problems
Several conditions can resemble each other at first glance. Parents often mix up tinea capitis with the following:
- Dandruff: flakes (white or yellow) but typically no ring-shaped red patch and no hair snapping
- Eczema: red, irritated skin and dryness, but it usually doesn’t form a distinct circular “spreading ring”
- Head lice: intense itching with visible lice or nits, but usually no circular bald patches or localized hair breakage
What most strongly points toward scalp ringworm is the rounded, expanding pattern plus broken hairs in the affected area.
When to Get Medical Help Right Away
Arrange urgent medical care if you see any of the following:
- Fever above 38°C (100.4°F)
- Noticeable swelling or significant scalp pain
- Pus, oozing, or thick crusting
- The patch spreads rapidly over a short time
- Your child seems unusually tired, weak, or generally unwell
Even when you’re not fully sure what it is, it’s safest to have a pediatrician evaluate the scalp.
Safe Steps You Can Take at Home While Waiting
While you’re booking an appointment or waiting to be seen, these actions can reduce irritation and limit spread:
Gentle cleansing
- Wash with a mild shampoo and lukewarm water
- Avoid aggressive rubbing or scrubbing over the patch
Reduce scratching
- Keep your child’s hands busy with games, reading, or storytelling
- Scratching can spread the infection and may introduce bacteria into irritated skin
Hygiene and laundry control
- Wash pillowcases, bedding, hats, and hair accessories in hot water
- Dry items thoroughly to reduce lingering fungal spores
What to Avoid (Even If Social Media Promises a “Quick Fix”)
Some popular home remedies can irritate the scalp and worsen inflammation. Avoid:
- Applying vinegar or raw garlic to the skin
- Using undiluted essential oils
- Scrubbing with harsh brushes or using alcohol-based treatments
- Relying on over-the-counter creams not designed for scalp fungal infections
These approaches may burn or inflame sensitive skin and delay proper treatment.
Why Over-the-Counter Creams Often Don’t Solve the Problem
Many parents try topical antifungal creams first, but scalp ringworm often persists because the fungus lives deep in hair follicles, where creams can’t reliably reach. Doctors typically prescribe:
- Oral antifungal medication, which targets the infection through the bloodstream
- Medicated shampoo, which helps reduce shedding and lowers transmission risk to others
Treatment often continues for several weeks to fully clear the infection and prevent recurrence.
Helping Your Child Feel Confident During Treatment
Visible patches and temporary hair loss can be upsetting for children. Emotional support can make a big difference:
- Remind them this condition is common and usually temporary
- Allow soft hats or light scarves if they feel self-conscious (wash them regularly)
- Keep daily routines stable to reduce stress
When children feel supported, they’re more likely to cooperate with treatment—and feel better faster.
Preventing Future Scalp Infections
You can reduce the chance of reinfection with practical habits:
- Encourage regular hair washing and good scalp hygiene
- Dry the scalp well after swimming or sports
- Don’t share personal items like combs, hats, or hair accessories
- Clean shared environments when possible (for example, sports gear areas or locker rooms)
These steps protect not just your child, but the whole household.
FAQ: Common Parent Questions
-
Will hair grow back after scalp ringworm?
Yes. In most cases, hair grows back normally once the infection is treated properly. -
Can adults catch scalp ringworm from a child?
It can spread through close contact, though healthy adults are generally less likely to develop symptoms. -
How long does treatment usually take?
Oral antifungal medicine commonly lasts 4–6 weeks, often paired with a medicated shampoo.
Disclaimer
This article is for informational purposes only and is not a substitute for professional medical advice. For diagnosis and personalized treatment, consult a pediatrician or qualified healthcare provider.