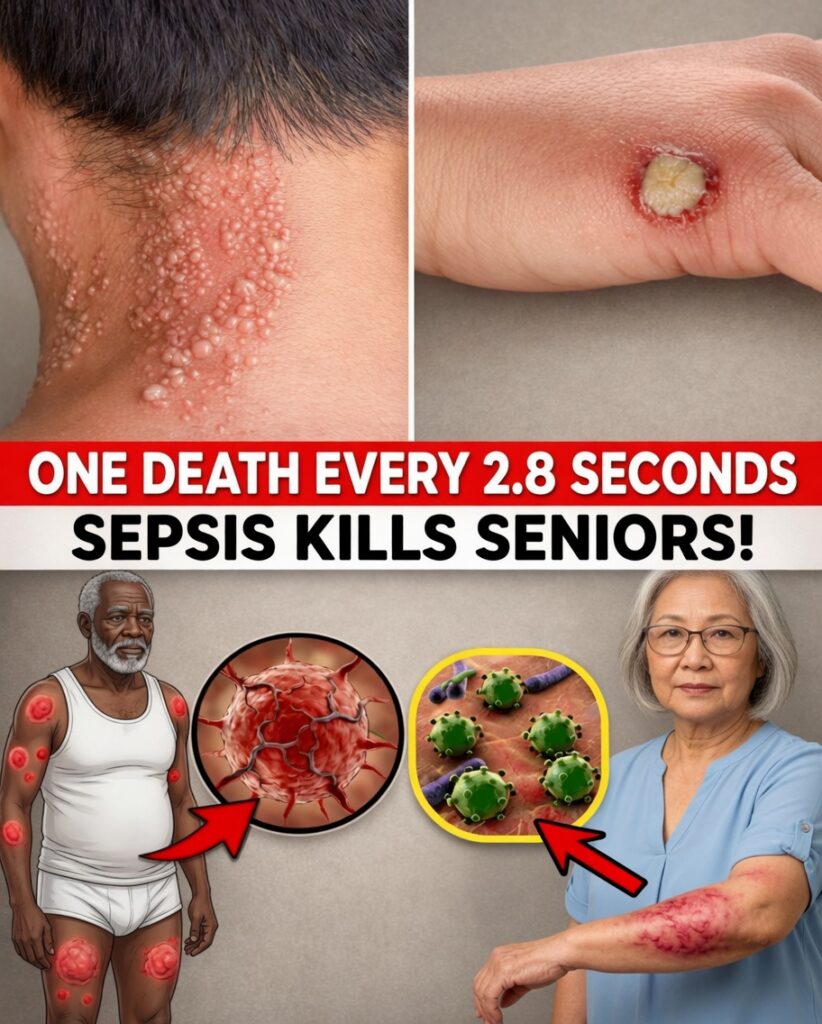
Sepsis in Older Adults Can Start Quietly—Know the Early Red Flags
Sepsis can develop in seniors with little warning, sometimes beginning as a routine infection that spirals quickly. For families supporting older loved ones, the earliest changes may look like “normal aging” or an off day—until the situation becomes urgent. Learning the most common early warning signs can help you speak with a healthcare professional sooner and with more clarity.
One important detail is frequently missed: the timing and clustering of symptoms. Stay with this guide to understand that pattern at the end.
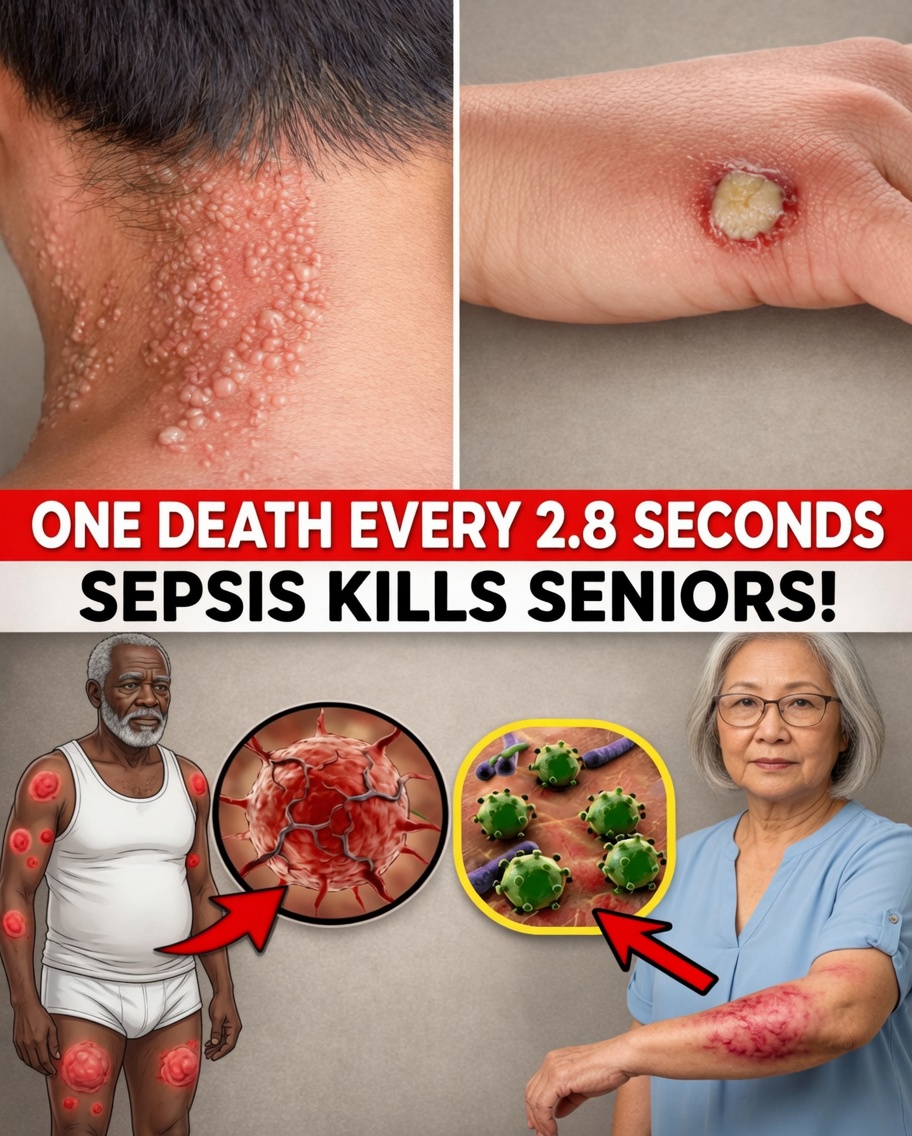
Why Sepsis in Seniors Is Often Missed
Aging bodies often react differently to infection. What seems minor—like a cough or urinary discomfort—can trigger a serious, whole-body response.
- Adults 65+ are generally at higher risk, often due to weaker immune defenses and existing medical conditions (commonly cited in public health data such as the CDC).
- Many sepsis cases begin with familiar infections, including urinary tract infections (UTIs) and pneumonia.
- Early symptoms can be mistaken for typical aging-related issues, which delays medical conversations when time matters.
Understanding what sepsis actually is makes these warning signs easier to interpret.
What Sepsis Really Means (It’s Not “Just an Infection”)
Sepsis happens when the body’s immune response to an infection becomes dysregulated, causing widespread inflammation that can disrupt blood flow and stress organs.
In older adults—especially those with conditions such as diabetes, lung disease, or heart problems—the inflammatory response may be more severe and harder to recover from (as discussed in major medical centers and research summaries, including sources like Johns Hopkins).
The challenge is that sepsis symptoms can resemble other common problems. The key is recognizing specific combinations and fast changes, which we’ll cover after the main warning signs.

The 5 Common Early Warning Signs of Sepsis in Seniors
1) Unusual Temperature Changes (High or Low)
A noticeable temperature shift can be a meaningful clue, including:
- Fever above 101°F (38.3°C) that persists or doesn’t respond as expected
- Low body temperature below 97°F (36.1°C), sometimes with chills or feeling cold despite a warm environment
Important note: many seniors do not mount a typical fever. In some cases, a lower-than-normal temperature may be an early signal, as noted in critical care literature.
If temperature changes are persistent—especially alongside other symptoms—contacting a clinician is a wise next step.
2) Fast Heart Rate and Rapid Breathing
When the body is under stress, heart rate and breathing can rise as it tries to maintain oxygen delivery.
Watch for:
- Resting heart rate above ~90 beats per minute
- Breathing rate above ~20 breaths per minute
These changes are easy to misread as anxiety, pain, or fatigue. If possible, recording at-home vitals can provide useful context for a healthcare provider.
3) Sudden Confusion or Mental Status Changes
A rapid shift in thinking or awareness is a major warning sign—especially when it appears quickly rather than gradually.
Examples include:
- New disorientation
- Trouble focusing or following conversations
- Unusual sleepiness or agitation
This differs from the slow progression typically seen in dementia. Studies commonly link these changes to how infection and inflammation can affect brain function, particularly in older adults.

4) A Powerful Sense of “Something Is Very Wrong”
Many families describe a striking symptom that’s hard to measure: a senior saying they feel profoundly unwell—sometimes phrased as:
- “This is the worst I’ve ever felt.”
- “I feel deeply off.”
- Extreme weakness, exhaustion, or a sense of dread
This can be easy to dismiss as a bad day, poor sleep, or medication effects. However, when this feeling appears suddenly—especially with other signs—it should raise concern.
5) Visible Skin Changes (Cold, Clammy, or Mottled)
Circulation can shift during severe inflammation. Signs to look for include:
- Skin that becomes cold and clammy
- Mottled or blotchy patches
- Areas that appear discolored or look “marbled,” sometimes not fading normally with pressure
These changes can be associated with more advanced progression, but spotting them early—especially when paired with confusion or breathing changes—can help prompt faster medical evaluation.

How Symptoms Escalate: The Pattern That Matters Most
A single symptom can have many explanations. What becomes concerning is when two or more signs appear suddenly, or when symptoms worsen over hours.
Examples of higher-risk combinations include:
- Confusion + rapid breathing
- Temperature changes + fast heart rate
- Profound malaise + clammy or mottled skin
Risk is often higher in seniors with:
- Chronic illnesses (diabetes, lung disease, kidney disease)
- Recent surgery or hospitalization
- Recent infections or wounds
What You Can Do Right Now (Practical Steps)
- Know the baseline: Learn the person’s typical temperature, pulse, and breathing rate when well.
- Track changes: Write down what you observe, including the time symptoms started and how fast they changed.
- Call a healthcare provider early: Share your measurements and the pattern (for example, “new confusion plus rapid breathing since this morning”).
- Seek emergency help immediately if symptoms are severe, rapidly worsening, or include collapse, extreme dizziness, or serious breathing difficulty.
- Use simple tools: A thermometer and a basic symptom log can help clinicians make faster decisions.
Quick Reference: The 5 Warning Signs to Remember
- Temperature extremes: Fever or unexpectedly low temperature with chills
- Rapid heart rate and breathing: Elevated rates at rest
- Sudden confusion: Fast-onset mental changes
- Profound malaise: An intense “not right” feeling
- Skin changes: Cold, clammy, or mottled appearance
Real-World Lessons: How Families Noticed the Shift
Families often describe the same turning point: they recognized that the change wasn’t gradual—it was sudden. Some noticed confusion and fast breathing after a procedure; others caught unusual skin changes in a loved one with diabetes. These experiences underline a practical truth: acting on early patterns can lead to earlier assessment and treatment.
The Key Insight Most People Miss: Trust the Cluster, Not Just One Symptom
The subtle pattern that often gets overlooked is rapid symptom clustering—especially:
- Confusion paired with breathing changes
- Confusion paired with skin changes
- Multiple signs appearing within the same day
When several warning signs show up together, hours matter. Seeking medical advice quickly aligns with what research and clinical guidance emphasize: earlier evaluation improves the chance of timely intervention.
Conclusion: Awareness Creates a Safety Net
Noticing the early signs of sepsis in older adults—temperature changes, rapid breathing or pulse, sudden confusion, profound malaise, and skin changes—can support faster, more informed conversations with healthcare providers. By tracking basic vitals and paying attention to sudden clusters of symptoms, families can reduce the chance that a serious issue is mistaken for “just aging.”
FAQ: Sepsis Signs in Seniors
What are the earliest signs of sepsis in older adults?
Common early indicators include temperature changes, rapid breathing, elevated heart rate, sudden confusion, extreme malaise, and skin changes, often following an infection.
How do I know if it’s sepsis or the flu?
Symptoms can overlap, but sudden combinations—especially confusion with fever, breathing changes, or skin mottling—should prompt professional evaluation. The flu typically improves with rest over time; sepsis can worsen quickly.
When should I seek medical help for possible sepsis?
Seek medical advice immediately if multiple symptoms appear abruptly, worsen over hours, or if the person seems severely unwell. If symptoms are serious or escalating, contact emergency services rather than waiting.