Endometriosis: When Period Pain Is More Than “Just Cramps”
Every month, millions of women deal with pelvic pain so intense that it goes far beyond ordinary period discomfort. For many, the pain lasts longer than a few days and affects work, sleep, relationships, and basic everyday activities. Just as difficult, many women feel dismissed or misunderstood when their symptoms are reduced to “normal female pain.”
Thankfully, awareness around endometriosis is growing. More women are learning to pay attention to recurring symptoms, ask better questions, and seek support sooner. And by the end of this article, you’ll learn one simple daily habit many women say helps them feel more in control.
What Is Endometriosis?
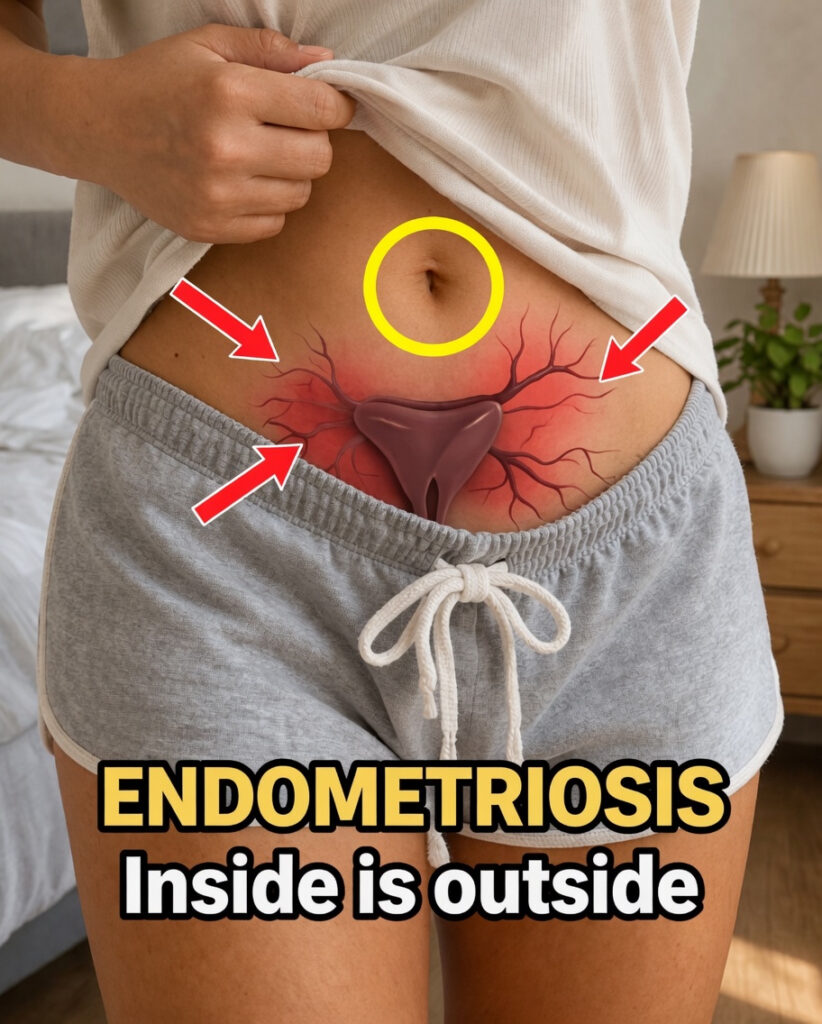
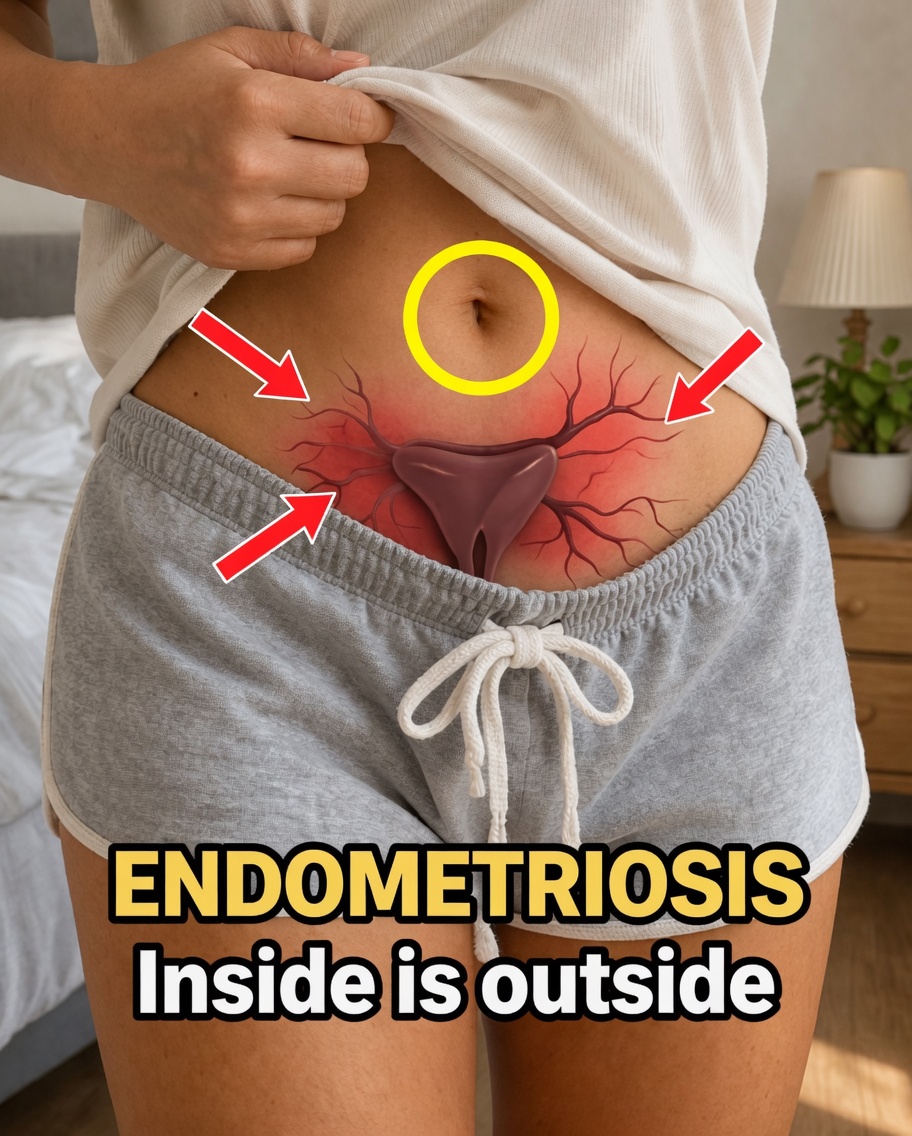
Endometriosis is a condition in which tissue resembling the lining of the uterus grows outside the uterus. This tissue may be found on the ovaries, fallopian tubes, the outer wall of the uterus, or other organs in the pelvic region. Over time, it can lead to inflammation, scar tissue, and adhesions that cause ongoing physical discomfort.
What makes this condition especially problematic is that this tissue behaves similarly to the uterine lining. During each menstrual cycle, it thickens, breaks down, and bleeds. But unlike menstrual blood from inside the uterus, this blood has no way to leave the body. As a result, it becomes trapped, which can trigger pain and other complications. That is why many people describe endometriosis as a case of tissue being “in the wrong place.”
According to international health research, endometriosis affects around 10% of women of reproductive age—about 190 million people globally. Even so, many women live with it for years before realizing what is happening. Knowing the basics can help you recognize when your symptoms may be signaling something more serious.
Common Symptoms to Watch For
Endometriosis does not look the same for everyone, which is one reason it can be difficult to identify early. Some women have mild symptoms, while others experience severe pain that disrupts daily life for days or even weeks. One of the most important clues is repetition—symptoms that return cycle after cycle.
Health professionals commonly point to the following signs:
- Intense menstrual cramps that begin before the period and continue for several days
- Ongoing pelvic pain between periods
- Pain during or after sex
- Pain with bowel movements or urination, especially during menstruation
- Heavy periods or unexpected bleeding between cycles
- Fatigue and bloating linked to the menstrual cycle
- Trouble becoming pregnant after trying for six months or longer
Some women also experience:
- Lower back pain
- Nausea
- Digestive discomfort that worsens before or during a period
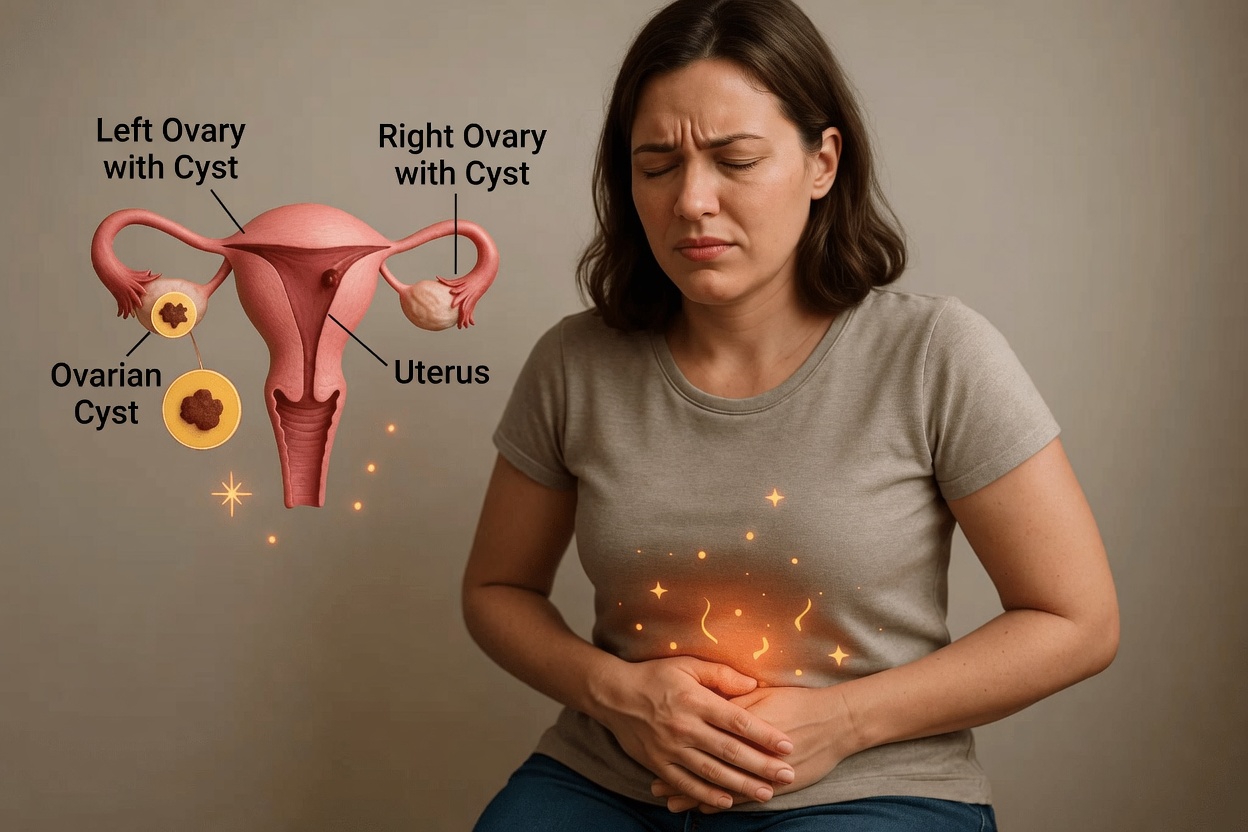
If this sounds familiar, you are not alone. Research suggests that many women wait seven to ten years between their first symptoms and a proper medical conversation about endometriosis.
What Causes Endometriosis?
Researchers have not identified one single cause of endometriosis, but several well-supported theories exist. One of the most discussed is retrograde menstruation. This happens when menstrual blood flows backward through the fallopian tubes instead of leaving the body normally, allowing tissue to implant outside the uterus.
Genetics may also increase risk. If your mother or sister has endometriosis, your chances may be higher. In addition, some studies suggest that immune system differences may prevent the body from clearing misplaced tissue effectively. Hormones and environmental factors are also being studied for their potential role.
The World Health Organization describes endometriosis as a chronic inflammatory condition, even though its exact cause remains uncertain.
One important point deserves emphasis: this is not your fault. Endometriosis is not caused by something you did, failed to do, or chose in your lifestyle. Understanding that can reduce self-blame and make it easier to have informed discussions with a healthcare professional.
How Endometriosis Can Affect Daily Life
Endometriosis can influence much more than physical health. During flare-ups, it may become difficult to concentrate at work or keep up with normal responsibilities. Relationships can also suffer, especially when pain makes intimacy difficult. Many women describe the emotional burden as heavy, especially when others cannot see their pain.
Fertility is another major concern. Not every woman with endometriosis will have trouble conceiving, but the condition can contribute to fertility challenges in some cases. Inflammation and scar tissue may interfere with the ovaries or fallopian tubes over time.
Still, endometriosis does not mean life must stop. Many women continue to lead active, fulfilling lives once they better understand their symptoms and find ways to manage them. Early recognition can make a meaningful difference.
How to Talk to Your Doctor About Symptoms
Discussing pelvic pain can feel uncomfortable, but being prepared can make the appointment much more effective. A good first step is to track your symptoms for at least two menstrual cycles. You can use a notes app, a symptom tracker, or a simple journal.
Record details such as:
- When the pain starts and ends
- How intense it feels on a scale from 1 to 10
- Whether anything makes it better or worse
- Any related issues like fatigue, bloating, nausea, or unusual bleeding
Bring this information with you to your appointment. Specific details help your doctor understand the pattern more clearly. For example, saying, “My cramps last eight days and are usually an 8 out of 10,” is much more useful than simply saying, “My periods are painful.”
You can also ask direct questions, such as:
- Could this be endometriosis?
- What tests or evaluations would help identify the cause?
- Should I see a pelvic pain specialist?
If you leave the visit feeling unheard or rushed, remember that a second opinion is always an option. Many specialists now focus specifically on pelvic pain and can evaluate symptoms with more targeted approaches before recommending invasive procedures.
Everyday Habits That May Help Ease Discomfort
There is no one-size-fits-all solution for endometriosis, but many women find that small daily habits improve comfort and help them feel more in control. These are not cures, but they may offer support when used consistently.
You may want to try:
- Using a heating pad or taking warm baths during painful days to relax muscles and improve circulation
- Doing gentle exercise such as walking, yoga, or swimming on most days, since low-impact movement has been linked to lower inflammation
- Following an anti-inflammatory eating style with more fruits, vegetables, whole grains, and omega-3-rich foods while cutting back on heavily processed meals
- Reducing stress with mindfulness, deep breathing, or journaling, as ongoing stress can intensify pain
- Staying well hydrated and maintaining regular sleep habits, since exhaustion and dehydration often make symptoms feel worse

One especially helpful daily habit many women mention is tracking what actually helps. Writing down which foods, activities, sleep patterns, or self-care practices make symptoms better—or worse—can turn a confusing experience into something more manageable. Over time, this simple habit can help you feel more informed and more in control of your body.
Final Thoughts: Understanding Endometriosis Matters
Endometriosis is common, but it should never be ignored or dismissed. Learning how the condition works, noticing recurring symptoms, and trying supportive daily habits can help you advocate for yourself and improve your quality of life.
Awareness is expanding, and more women are speaking openly about experiences that were once kept silent. That shift matters.
Listening to your body is not overreacting. It is a powerful first step. You deserve answers, support, and care.
Frequently Asked Questions
Is endometriosis the same thing as painful periods?
No. Painful periods can happen for many reasons, but endometriosis involves tissue similar to the uterine lining growing outside the uterus. It can cause pain not only during menstruation, but at other times of the month as well. Typical cramps usually improve with standard pain relief and are less likely to interfere severely with daily life.
Can endometriosis disappear on its own?
For many women, symptoms continue until menopause, although they may change during pregnancy or with hormonal shifts. Endometriosis does not usually go away without some form of management, which is why regular monitoring and ongoing conversations with your doctor are important.