Living With Rheumatoid Arthritis: From Daily Pain to New Possibilities
Living with rheumatoid arthritis often means waking up to aching, stiff joints that make even simple tasks feel exhausting. This chronic autoimmune disease triggers your immune system to attack your own joints, leading to pain, swelling, and stiffness that can slowly chip away at your independence and enjoyment of everyday life.
Rheumatoid arthritis frequently appears during prime working and family years, and without proper control, each day can bring a little less mobility and a little more frustration.
There is still no cure. However, breakthroughs in rheumatoid arthritis treatment are giving people more choices than ever to control inflammation, protect joints, and reclaim daily routines. Read through to the end—one rapidly evolving approach may be the turning point you have been hoping for on your rheumatoid arthritis journey.
Why Rheumatoid Arthritis Feels Like a Relentless Battle—and Why Hope Is Rising
Rheumatoid arthritis often arrives suddenly, transforming ordinary activities—opening jars, getting dressed, walking down stairs—into painful challenges that drain both energy and confidence.
Persistent inflammation inside the joints can cause swelling and tenderness that make simple movements, like buttoning a shirt or holding a coffee mug, feel nearly impossible. Over time, this can create a constant sense of limitation and discouragement.
But the outlook is changing. Advances in rheumatoid arthritis management are helping more people reduce daily pain, move more freely, and avoid long-term joint damage.
- Recent data suggests that more than 70% of people with rheumatoid arthritis experience morning stiffness lasting over an hour, making it feel like you have already done a full day’s work before breakfast.
- If left unmanaged, rheumatoid arthritis can accelerate joint destruction and severe fatigue, further eroding quality of life.
You are not alone in this struggle—and you are not without options.

Core Medical Treatments: Taking Control of Inflammation
If rheumatoid arthritis pain is dominating your days right now, the first goal is to calm inflammation and protect your joints. Foundational therapies are designed to do exactly that.
Fast-Acting Symptom Relief
-
Non-steroidal anti-inflammatory drugs (NSAIDs)
Medications like ibuprofen or naproxen can lower pain and swelling from rheumatoid arthritis, making it easier to move through your day with less discomfort. -
Corticosteroids
Steroid medications, such as prednisone, can provide rapid relief during flares by powerfully suppressing inflammation. Because of potential side effects, most rheumatologists recommend using them at the lowest effective dose and for the shortest possible time.
Long-Term Disease Control
-
Conventional DMARDs (Disease-Modifying Antirheumatic Drugs)
Drugs such as methotrexate, leflunomide, or sulfasalazine help slow or even halt the underlying disease process of rheumatoid arthritis. They aim to prevent progressive joint damage and preserve function over the long term. -
Biologic DMARDs
Biologic therapies, including TNF inhibitors and other targeted biologics, are designed to block specific steps in the immune response that drive rheumatoid arthritis. They are often used when traditional DMARDs are not enough to control symptoms or disease progression.
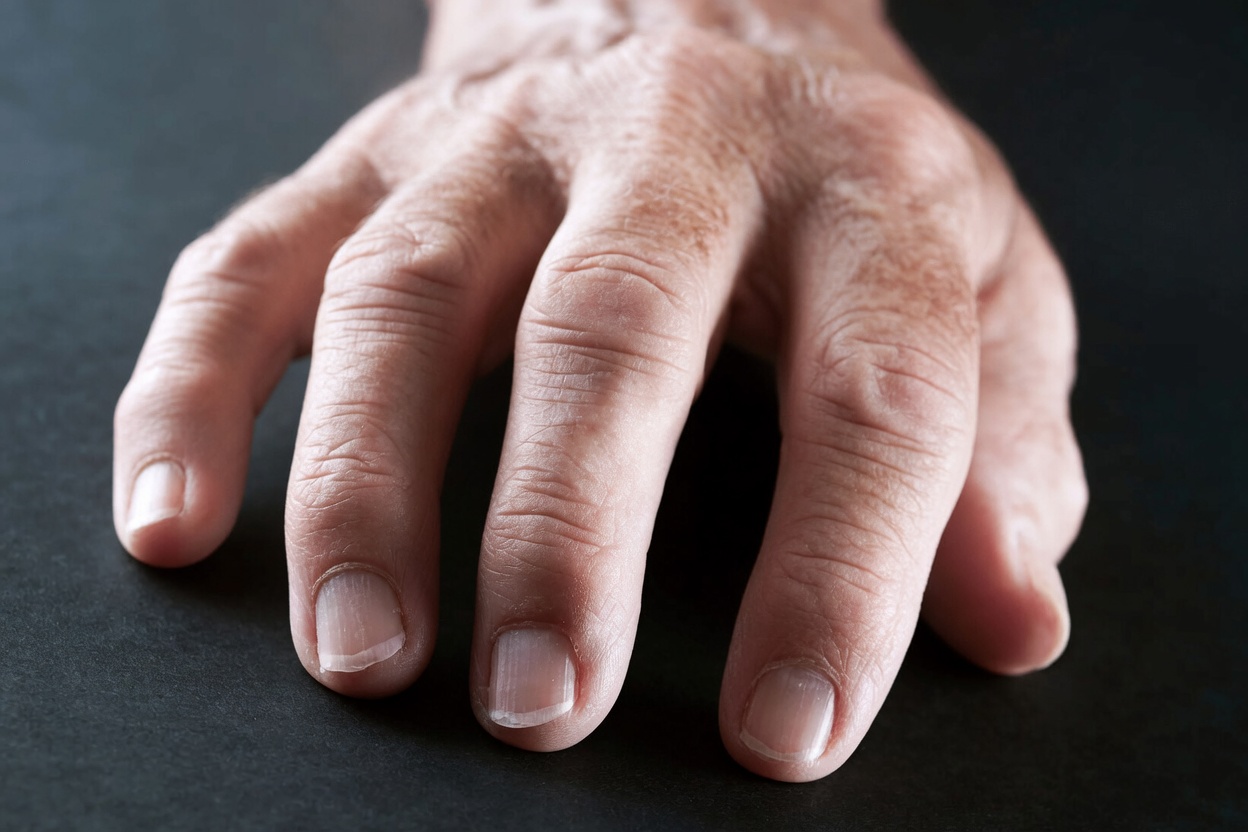
Together, these medications form the backbone of modern rheumatoid arthritis treatment, giving many people a chance to maintain work, family life, and hobbies.
Next-Level Options: Advanced Therapies for Rheumatoid Arthritis
Beyond the core therapies, newer treatment options are helping to personalize and simplify rheumatoid arthritis care.
Targeted Oral Medications
-
JAK inhibitors (e.g., tofacitinib)
These medications act on Janus kinase (JAK) pathways—key signaling routes in the immune system that promote inflammation in rheumatoid arthritis. Taken as pills, they offer a convenient alternative to injectable therapies for some patients. -
IL-6 inhibitors (e.g., tocilizumab)
These drugs block interleukin-6 (IL-6), a powerful inflammatory messenger involved in rheumatoid arthritis. By interrupting IL-6 signaling, they can reduce pain, swelling, and laboratory markers of inflammation.
Smarter Combinations and Cost-Saving Options
-
Combination therapy
Combining methotrexate with a biologic or JAK inhibitor often provides stronger and more consistent control of rheumatoid arthritis than using either one alone. This approach is common when single therapies do not fully control the disease. -
Biosimilars
Biosimilars are highly similar versions of existing biologic drugs, designed to offer comparable safety and effectiveness at a lower cost. They are expanding access to advanced rheumatoid arthritis treatments for more people worldwide.
By learning about these next-level options, you are already among the minority of patients who actively seek out information to better manage rheumatoid arthritis and improve long-term outcomes.
Real People, Real Progress: Stories From the Front Line
Hearing how others have navigated rheumatoid arthritis can make the possibilities feel more real.
Meet Karen, 52. She is a teacher whose severe morning stiffness made getting to class, standing for lessons, and interacting with students almost unbearable. After she and her rheumatologist decided to try a JAK inhibitor, her symptoms gradually eased.
“Before, rheumatoid arthritis pain completely wiped out my energy,” she recalls. “Now I feel like I have my life back.”
Then there is David, 58. Years of uncontrolled rheumatoid arthritis had damaged his knees so badly that walking short distances was a challenge. Working with his care team, he started combination therapy and committed to regular physical therapy.
Over time, his mobility improved, and he was able to return to playing golf—something he thought he had lost forever. His story shows how consistent, comprehensive rheumatoid arthritis treatment can change what daily life looks like.
Beyond Medication: Emerging and Supportive Strategies
Medication is crucial, but it is only one part of a complete rheumatoid arthritis management plan. Supportive and emerging strategies can work alongside your prescribed treatments to further reduce symptoms and protect function.

Innovative and Complementary Approaches
-
Vagus nerve stimulation
Noninvasive devices that gently stimulate the vagus nerve may help modulate inflammation signals in some autoimmune conditions, including rheumatoid arthritis. Research is ongoing, but early findings are promising. -
Omega-3 fatty acids
Omega-3s from fish oil or algae-based supplements may help reduce joint tenderness and morning stiffness in some people with rheumatoid arthritis, especially when combined with standard medical treatment.
Lifestyle and Rehabilitation Support
-
Physical therapy and gentle exercise
Tailored exercise programs, stretching, and strength training can maintain joint mobility and muscle support even when rheumatoid arthritis is trying to restrict your movement. Activities like walking, swimming, or yoga—under professional guidance—can be particularly helpful. -
Anti-inflammatory eating pattern
A Mediterranean-style diet rich in vegetables, fruits, whole grains, olive oil, nuts, seeds, and fatty fish may help lower systemic inflammation and support overall health in people with rheumatoid arthritis. -
Stress management
Practices such as mindfulness meditation, deep breathing, or yoga can reduce stress, which may in turn help lessen the frequency or intensity of rheumatoid arthritis flares for some individuals. -
Joint protection strategies
Using ergonomic tools, splints, or adaptive devices can minimize strain on vulnerable joints. Small changes—like using utensils with larger grips or adjusting your workstation—can significantly reduce daily pain.
Regular follow-up with your rheumatology team ensures that any changes in your rheumatoid arthritis are detected early, allowing for timely adjustments in treatment to maintain long-term stability.
A Simple 12-Week Roadmap to Stronger Rheumatoid Arthritis Control
To help visualize how different strategies fit together, here is a sample timeline many treatment plans roughly follow. Your own plan will be personalized by your doctor, but this gives a helpful overview:
| Timeframe | Focus Area | Key Actions | Main Expected Benefit |
|---|---|---|---|
| Weeks 1–4 | Build the basics | Start or optimize DMARDs; begin physical therapy | Reduced inflammation and initial symptom relief |
| Weeks 5–8 | Step up treatment | Add a biologic or JAK inhibitor if needed | Better control of pain, stiffness, and daily function |
| Weeks 9–12 | Reinforce support | Implement diet changes, regular exercise, stress tools | Improved energy, resilience, and overall well-being |
| Ongoing | Monitor & adjust | Regular check-ups, blood tests, treatment fine-tuning | Long-term stability and protection against joint damage |
This kind of structured approach helps turn rheumatoid arthritis care into a clear, manageable plan rather than a series of unpredictable crises.
Quick Check-In: Mid-Article Reflection
Take a moment to assess where you are right now on your rheumatoid arthritis journey. Reflecting can help you and your care team make better decisions.
- About how many different strategies have we covered so far? (Hint: roughly 15.)
- What is your single biggest challenge with rheumatoid arthritis at this moment—pain, stiffness, fatigue, mobility, or something else?
- Which option do you think could be the biggest breakthrough for you personally: a new medication, lifestyle changes, or emerging technologies?
- If you were to rate your joint comfort on a scale of 1–10 right now, how does that compare with how you felt before reading this?
- Are you ready to explore the most exciting direction in rheumatoid arthritis care—highly personalized treatment plans?
Use your answers as a starting point for your next discussion with your healthcare provider.
The Game Changer: Personalized Medicine for Rheumatoid Arthritis
Everything described so far can help manage rheumatoid arthritis—but the most transformative advances center on tailoring therapy to the individual.

What Personalized Medicine Means for Rheumatoid Arthritis
Personalized medicine uses advanced testing—such as biomarkers, imaging, and detailed health data—to identify:
- Which inflammatory pathways are most active in your particular case of rheumatoid arthritis
- Which drug classes you are more likely to respond to
- How to adjust doses and combinations for maximum benefit and minimal side effects
Instead of trial-and-error that can take months or years, personalized approaches aim to match the right treatment to the right person more quickly and accurately.
Imagine 30 days from now:
- Less morning stiffness and fewer flares
- More confidence in your ability to plan your days
- Greater freedom to enjoy activities you thought you might have to give up
That is the potential payoff of combining consistent action with more individualized rheumatoid arthritis care.
Extra Pointers Most Guides Leave Out
Small, practical habits can make a surprising difference over time:
-
Track your flares
Keep a simple journal or use an app to record when flares occur, what you were doing, what you ate, how you slept, and your stress level. Patterns often emerge, helping you identify personal triggers and make targeted changes. -
Warm up before moving
A warm bath or shower before exercise or physical therapy can relax stiff joints and muscles affected by rheumatoid arthritis, allowing you to move more comfortably and safely.
These seemingly minor steps can amplify the impact of your medical treatment.
The Common Thread: What Really Makes the Difference
Across all the strategies—medications, lifestyle changes, and emerging technologies—one principle stands out:
Early, assertive, and personalized treatment offers the best chance of reaching low disease activity or even remission in rheumatoid arthritis.
Partnering closely with a rheumatologist, starting appropriate therapy as soon as possible, and adjusting your plan based on your unique response can dramatically change the course of the disease.
FAQ: Common Questions About Rheumatoid Arthritis
Is there a cure for rheumatoid arthritis?
Currently, there is no cure for rheumatoid arthritis. However, modern treatments can effectively control symptoms, reduce inflammation, and slow or prevent joint damage for many people.
What lifestyle changes can help with rheumatoid arthritis?
Key lifestyle strategies include:
- Regular, gentle exercise tailored to your abilities
- Following an anti-inflammatory diet, such as a Mediterranean-style eating pattern
- Prioritizing quality sleep
- Managing stress through mindfulness, relaxation techniques, or counseling
- Avoiding smoking and limiting excess alcohol
These steps support medical treatments and can improve overall well-being.
How do I know if my rheumatoid arthritis treatment is working?
Signs that your treatment plan is helping may include:
- Fewer or less intense flares
- Reduced morning stiffness and joint swelling
- Improved energy levels and ability to perform daily tasks
- Better results on blood tests and imaging, as assessed by your doctor
If you are not seeing progress, or if side effects are troubling, talk with your rheumatologist about adjusting your treatment.
Final Thought: Staying Proactive on Your Rheumatoid Arthritis Journey
This article is for educational purposes only and does not replace professional medical advice. Always consult your healthcare provider for diagnosis and treatment decisions related to rheumatoid arthritis.
One last suggestion: ask your rheumatologist about clinical trials. New therapies for rheumatoid arthritis are often tested in clinical studies long before they are widely available, and participating may give you access to cutting-edge options.
Your better, more active days with rheumatoid arthritis may be closer than you think.