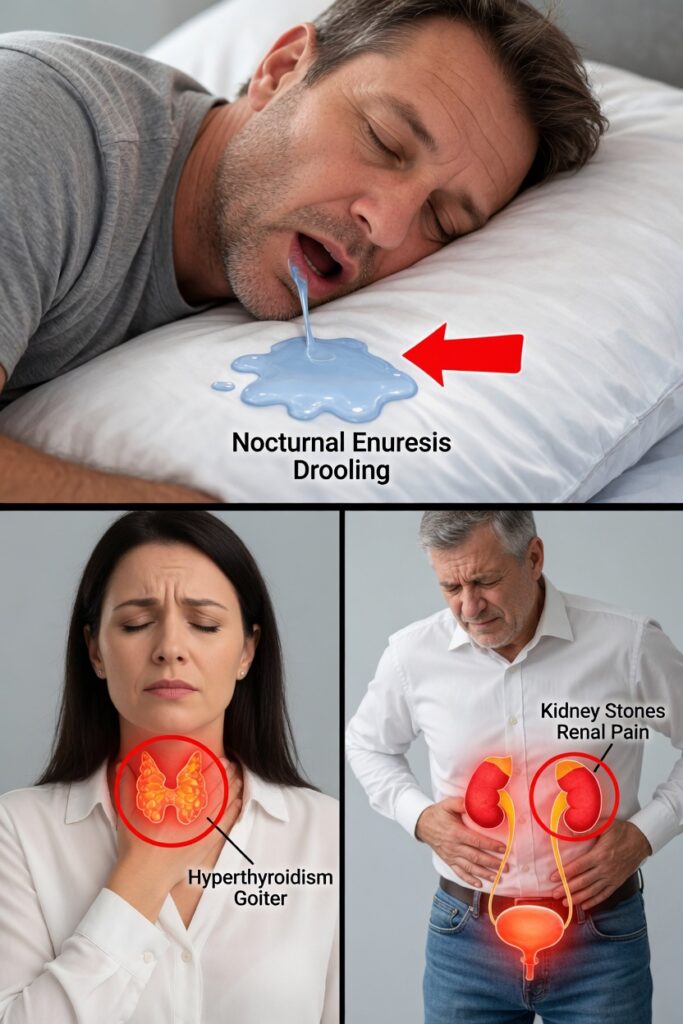
Imagine waking up to a damp pillow, noticing dried saliva at the corner of your mouth, and feeling both embarrassed and puzzled. You may wonder whether it was a fluke—or a sign that something else is going on.
Excessive drooling during sleep (often called nocturnal sialorrhea) is more common in adults than many people realize. In many cases it’s harmless, but persistent nighttime drooling can also be linked to issues that affect breathing, swallowing, or saliva control.
If it’s happening more often—especially alongside symptoms like snoring, daytime fatigue, or heartburn—it may be worth paying closer attention. Early evaluation can also help prevent complications such as skin irritation around the mouth or, in rare cases, aspiration (saliva entering the airway).
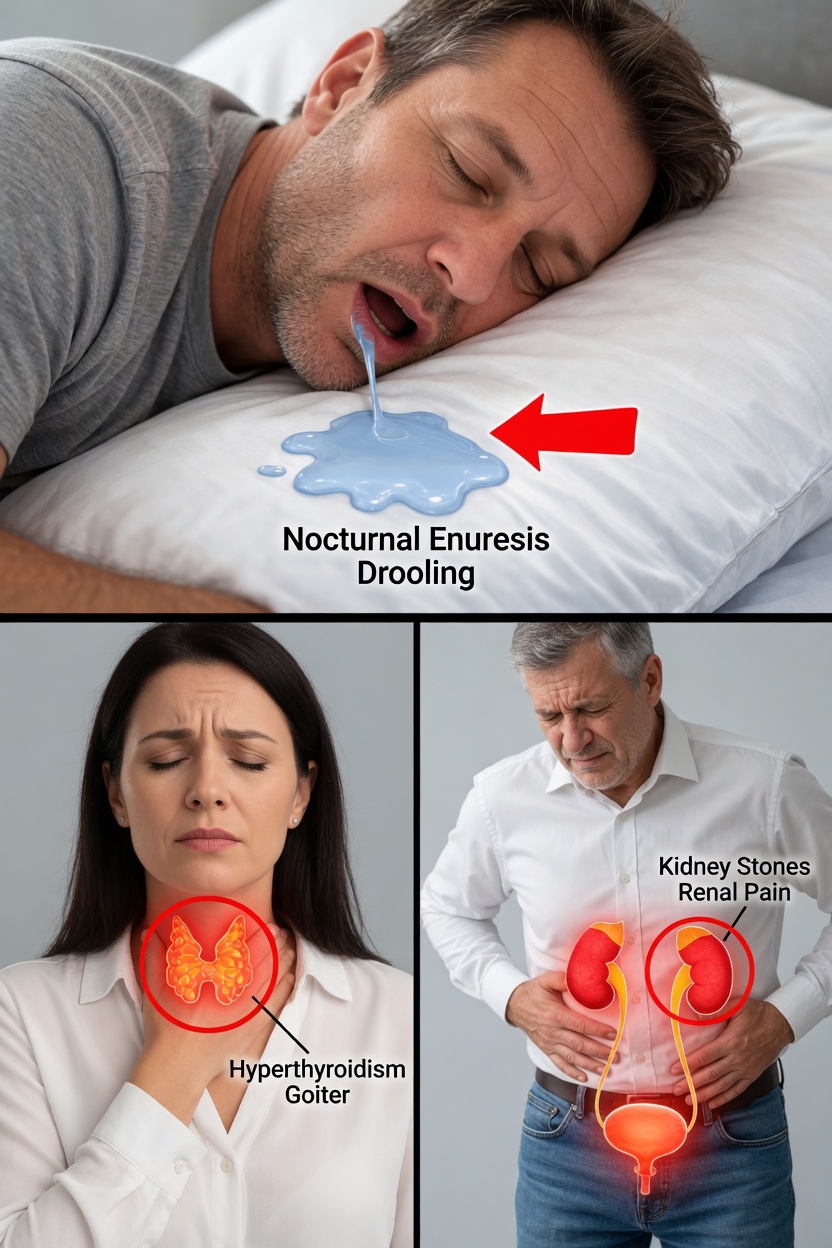
Why Drooling Often Increases During Sleep
Even while you sleep, your body continues to produce saliva. However:
- Swallowing frequency decreases
- Facial and jaw muscles relax
- Gravity matters, especially if you sleep on your side or stomach
- Mouth breathing makes it easier for saliva to escape
If a condition increases saliva production or interferes with normal muscle control, nighttime drooling can become more noticeable. Sometimes it truly is “just sleep position,” but if it’s frequent, the cause is often more than posture alone.

The 8 Conditions That May Cause Nighttime Drooling in Adults
Below are eight common links reported by major medical sources (including sleep and neurology experts). Use this list as a guide—not as a diagnosis.

8) Nasal Congestion or Sinus Problems
When your nose is blocked, you’re far more likely to sleep with your mouth open, allowing saliva to pool and leak out.
Common triggers include:
- Seasonal allergies
- Colds or flu
- Chronic sinusitis
- Deviated septum (in some cases)
If congestion is occasional, drooling often resolves on its own. If it keeps returning, it may be part of a bigger sleep-breathing pattern.
7) Gastroesophageal Reflux Disease (GERD)
GERD can cause stomach acid to move upward, especially when lying down. Your body may respond by producing extra saliva to help neutralize irritation—sometimes leading to drooling at night.
Nighttime reflux can also come with:
- Heartburn
- Sour taste in the mouth
- Chronic cough
- A sensation of choking or throat tightness
If drooling appears alongside regular reflux symptoms, GERD management can make a meaningful difference.
6) Medication Side Effects
Some medications can increase saliva or reduce your ability to manage it normally. This side effect is often treatable once identified.
Medication categories that may contribute include:
- Certain antipsychotic medications
- Some Alzheimer’s and dementia-related drugs
- Cholinergic agents (which can stimulate salivation)
If the timing of drooling matches a new prescription or dosage change, bring it up with your clinician—do not stop medications on your own.
5) Obstructive Sleep Apnea (OSA)
Obstructive sleep apnea can cause repeated breathing interruptions during sleep. Many people with OSA compensate by mouth breathing, which increases drooling risk.
OSA is commonly associated with:
- Loud snoring
- Gasping or choking at night
- Morning headaches
- Daytime sleepiness and poor concentration
Because sleep apnea affects cardiovascular and metabolic health, persistent drooling plus snoring or fatigue should raise the priority for evaluation.

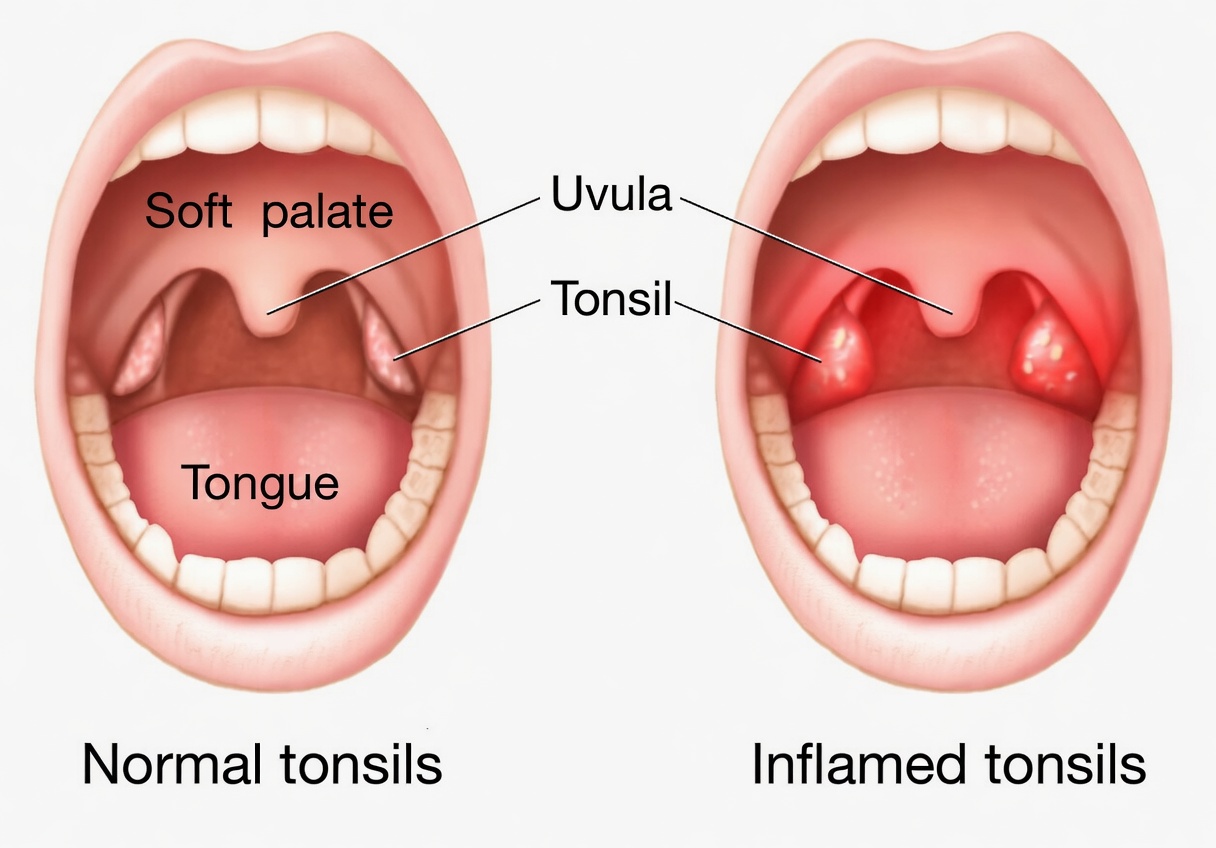
4) Infections or Throat Irritation
Temporary infections and irritation can overwhelm your usual swallowing rhythm, especially when you’re asleep.
Possible contributors include:
- Tonsillitis
- Sore throat or pharyngitis
- Post-nasal drip
- Respiratory infections that increase mucus and saliva
If drooling improves when the infection resolves, it’s usually not concerning. If irritation persists or recurs often, it deserves follow-up.
3) Stroke or a Recent Neurological Event
Drooling that appears suddenly, especially with facial weakness or speech difficulty, can be a warning sign.
After a stroke, drooling may occur due to:
- Reduced muscle strength on one side of the face
- Impaired swallowing coordination
- Difficulty sealing the lips
If drooling is new and paired with symptoms like slurred speech, arm weakness, or facial droop, seek urgent medical care.

2) Parkinson’s Disease
In Parkinson’s disease, drooling often happens not because the body makes too much saliva, but because swallowing becomes less frequent or less coordinated.
It may also appear alongside:
- Tremor
- Muscle stiffness
- Slowed movement
- Changes in speech or facial expression
Many people find drooling one of the most frustrating day-to-day symptoms, and treatment options can help.
1) Other Neurological Conditions
Several neurological disorders can disrupt the nerve and muscle control required to keep saliva managed—especially during sleep. These may include:
- ALS (amyotrophic lateral sclerosis)
- Multiple sclerosis (MS)
- Cerebral palsy
- Other progressive neuromuscular disorders
These conditions can affect facial tone, swallowing reflexes, and airway protection—making drooling a common and sometimes persistent issue.

Quick Reference: Patterns That Can Point to a Cause
- Mouth breathing-related drooling: often linked to nasal blockage or sleep apnea (commonly with snoring and fatigue)
- Excess saliva production: can occur with GERD or throat irritation (often with heartburn or sore throat)
- Reduced muscle control: can be medication-related or neurological (often with speech changes or weakness)
- Swallowing coordination issues: common in Parkinson’s and other neurological conditions (often with tremors or stiffness)
Real-Life Examples: When Recognition Led to Relief
- Laura, 58 noticed increasing drooling along with snoring and daytime exhaustion. A sleep study revealed obstructive sleep apnea, and CPAP therapy significantly reduced the drooling while improving her energy.
- David, 65 saw that drooling often followed nighttime reflux episodes. After addressing GERD triggers and treatment, his symptoms improved noticeably.
These stories highlight a key point: drooling may feel embarrassing, but identifying the underlying driver can be genuinely life-improving.
Safe Steps to Take If Nighttime Drooling Keeps Happening
Occasional drooling can be normal. If it becomes frequent, try these practical steps:
-
Track patterns for 1–2 weeks
- How often it happens
- Sleep position
- Alcohol use, allergies, or reflux symptoms
- New medications
-
Adjust sleep habits
- Try sleeping on your back (if safe and comfortable)
- Consider nasal strips or saline rinses for congestion
-
Address likely triggers
- Manage reflux with clinician guidance
- Treat allergies or chronic sinus issues
-
Talk to a healthcare professional
- Especially if drooling is persistent or paired with other symptoms
When to Seek Medical Help
Seek evaluation sooner if you notice:
- Drooling with snoring, choking, or severe fatigue
- Sudden onset drooling (especially with facial or speech changes)
- Multiple symptoms at once (reflux + sleep issues, or weakness + drooling)
- Concern that a medication may be contributing
Bringing a short sleep diary and a medication list can make the visit far more productive.
Final Takeaway
A wet pillow once in a while is usually nothing to worry about. But nightly or worsening drooling can be a useful clue—often connected to breathing issues, reflux, medications, or neurological conditions. Recognizing the pattern early may prevent discomfort and support better sleep and overall health.
FAQ
Is drooling while sleeping normal?
Yes. Occasional drooling during sleep can be normal. However, consistent drooling, especially with symptoms like snoring, reflux, or fatigue, should be discussed with a healthcare professional.
Can medications cause drooling at night?
They can. Some medications—particularly certain psychiatric and neurological drugs—may increase saliva or reduce saliva control. If this starts after a medication change, consult your prescribing clinician.
How can I reduce drooling while sleeping?
Helpful strategies may include changing sleep position, improving nasal breathing, and managing conditions like GERD or sleep apnea. A clinician can recommend the safest approach based on your situation.
Medical disclaimer: This article is for informational purposes only and does not replace professional medical advice. If you have persistent symptoms or concerns, consult a qualified healthcare provider for personalized evaluation and care.