Cervical Cancer: Why Recognizing Early Warning Signs Matters
Cervical cancer is still one of the most common cancers affecting women worldwide. Yet many early warning signs of cervical cancer are easy to shrug off as “small issues”—until the worry starts building in the background. When your body feels different and you can’t explain why, it can drain your energy, trigger anxiety about the future, and make you feel less present with the people you care about.
The good news is that learning to spot early symptoms of cervical cancer helps you respond sooner and with more confidence. A simple mindset shift can change everything: treat subtle body changes as useful information—not something to fear or ignore.
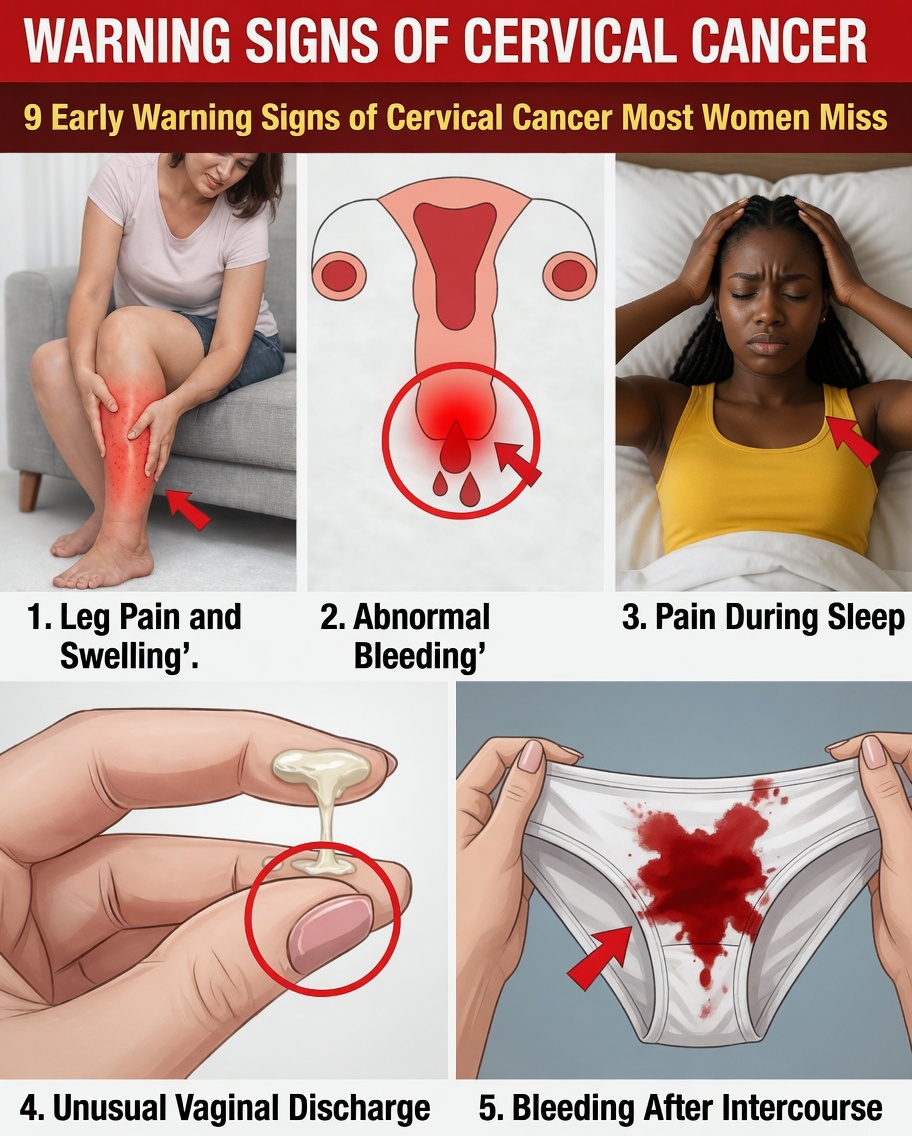
Why Early Warning Signs of Cervical Cancer Are Often Missed
Cervical cancer typically grows slowly over years. Because of that, early warning signs often don’t feel dramatic at first, which can lead many women to doubt their instincts and delay getting checked.
Major organizations such as the American Cancer Society and the National Cancer Institute emphasize that earlier attention can make a real difference, especially since most cervical cancer cases are linked to HPV (human papillomavirus)—a virus that is extremely common.
Another challenge is that many symptoms resemble everyday concerns like hormonal shifts, stress, or routine infections. The Mayo Clinic notes that these overlaps make it easy to postpone a medical visit, even when symptoms persist.
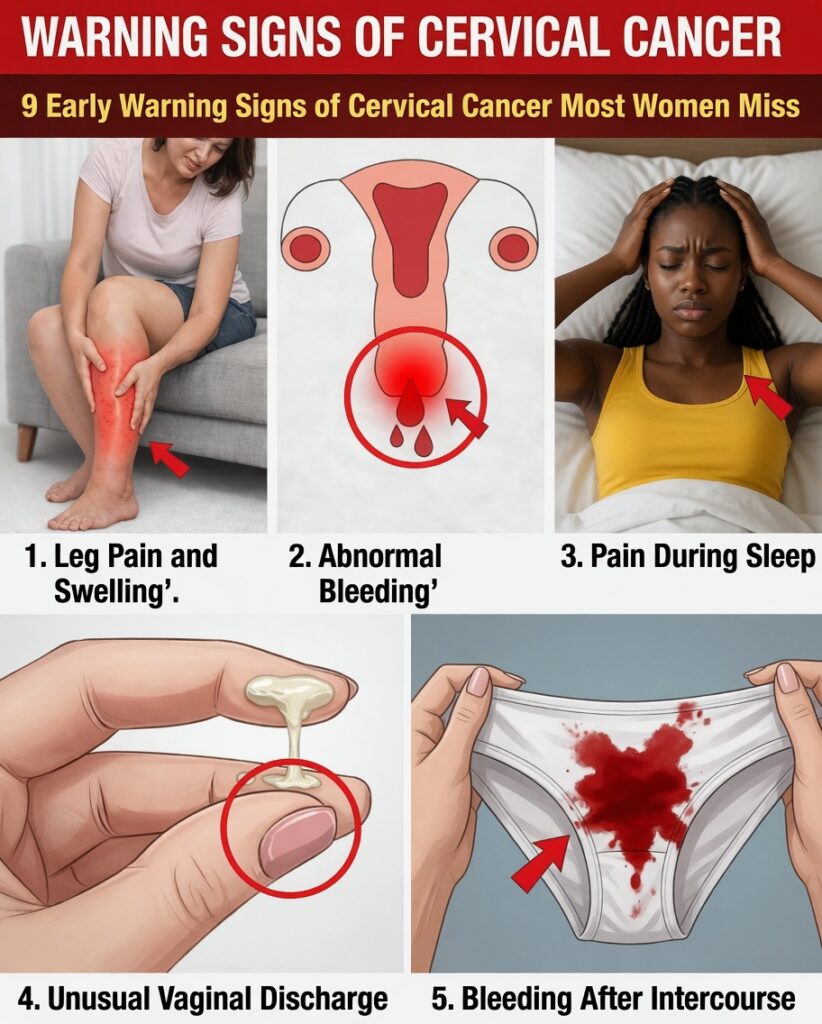
Sign #1: Abnormal Vaginal Bleeding
One of the most frequently reported early warning signs of cervical cancer is unusual vaginal bleeding, including:
- Spotting between periods
- Bleeding after sex
- Bleeding after menopause
- Periods that suddenly become heavier or last longer than usual
In cervical cancer, tissue changes can make small blood vessels more fragile, so bleeding may occur more easily. Even if it seems minor, repeated or unexplained bleeding is worth tracking and discussing with a clinician.
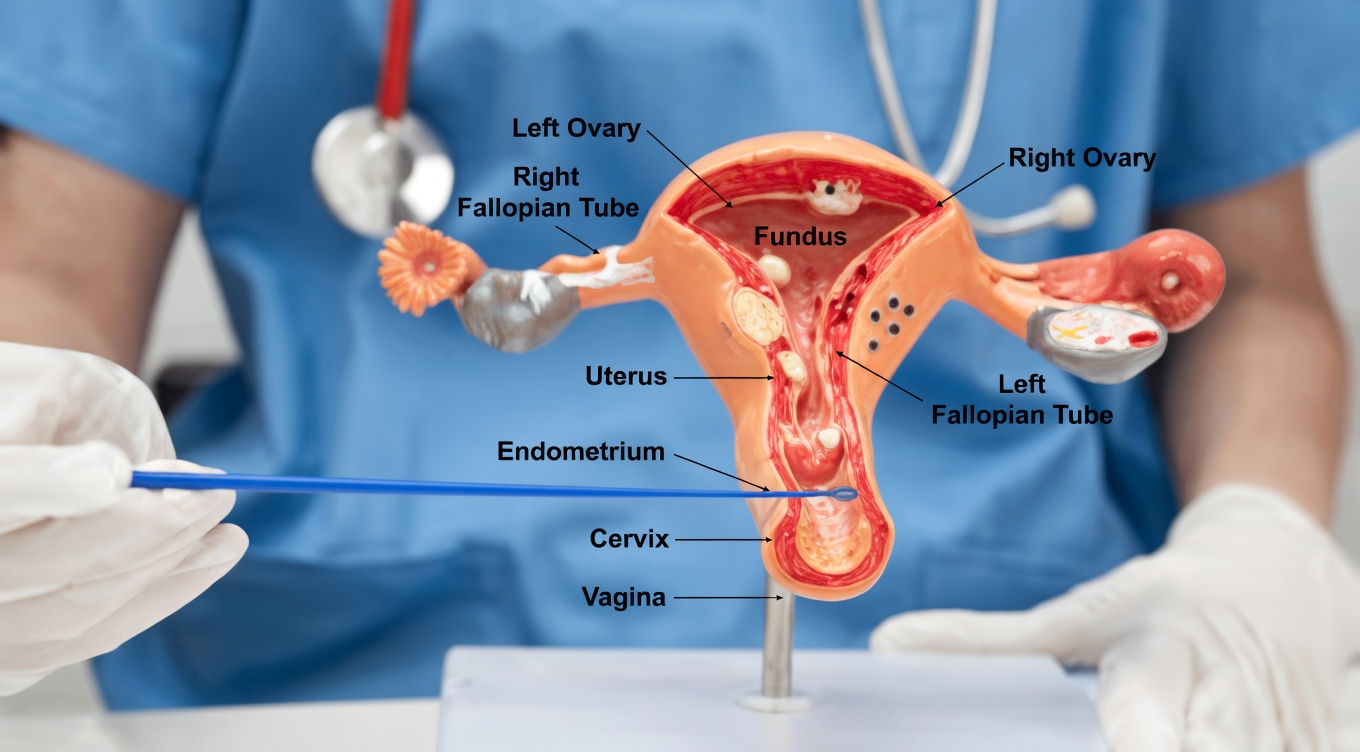
Sign #2: Unusual Vaginal Discharge That Doesn’t Go Away
Persistent changes in discharge are another important early sign of cervical cancer. Typical discharge is often clear or milky with minimal odor. With cervical cancer, discharge may become:
- Watery
- Pink, brown, or blood-tinged
- Strong-smelling or foul-smelling
- More frequent or longer-lasting than normal
These changes can cause embarrassment and make people withdraw from activities they normally enjoy. If discharge shifts noticeably and lingers, it deserves attention—especially if other symptoms appear alongside it.
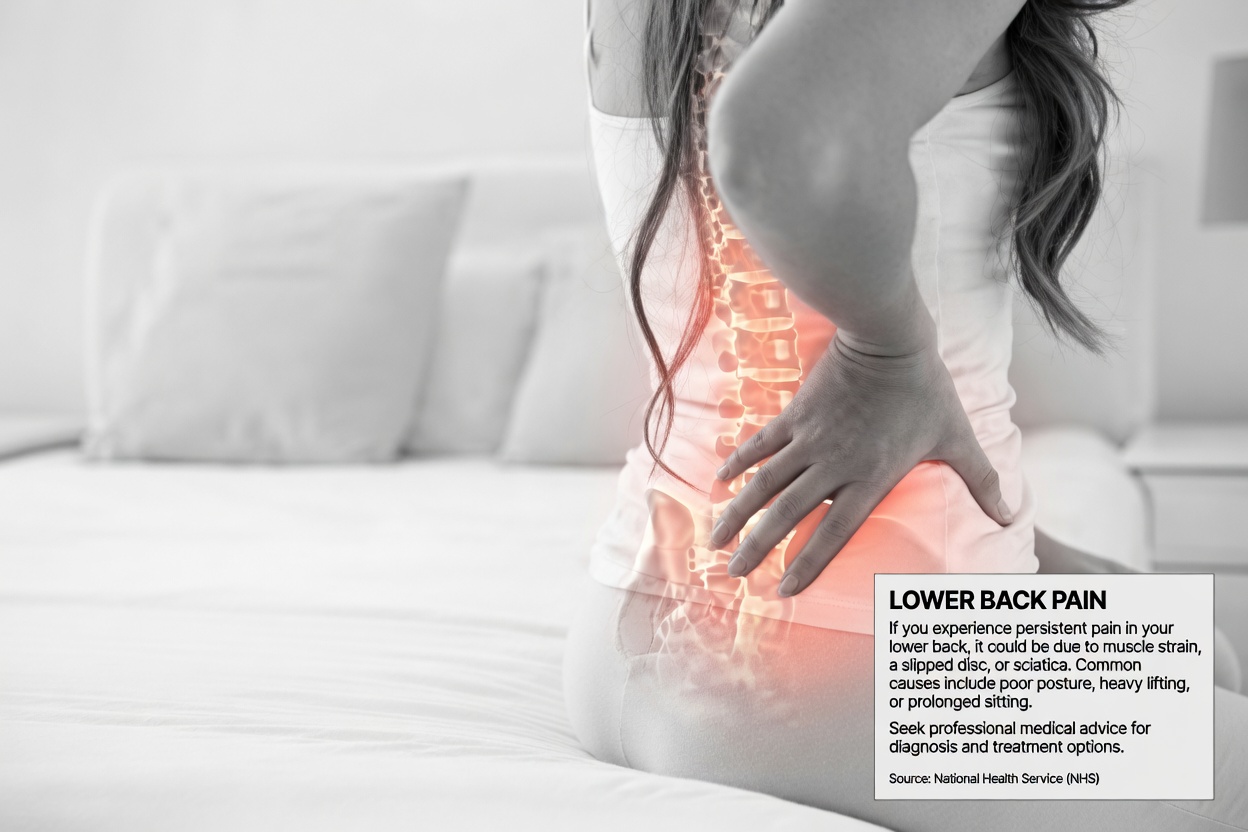
Sign #3: Ongoing Pelvic Pain or Lower Back Pain
A deep, dull ache in the pelvis or lower back that doesn’t improve with rest is commonly overlooked. Research in oncology literature links this type of discomfort to pressure or irritation affecting nearby nerves and tissues.
What makes this symptom stand out is persistence. Unlike typical menstrual cramps, the pain may linger, recur frequently, and interfere with sleep, work, and mood. Tracking the pattern can help you decide when it’s time to seek medical advice.
Sign #4: Pain During or After Intercourse
Pain during intimacy—or discomfort that continues afterward—can be an early warning sign of cervical cancer. Mayo Clinic data suggests this occurs in a meaningful portion of early cases and may also be accompanied by light bleeding.
Inflammation and tissue changes around the cervix can make contact uncomfortable. Beyond the physical impact, it can strain relationships and reduce overall well-being. If sex has started to feel noticeably different, it’s valid to treat it as a medical signal, not something to “push through.”

Quick Self Check
Consider these questions briefly:
- Which symptoms have stood out to you the most so far?
- Are any of them persistent or repeating?
- From 1–10, how aware do you feel of your body signals today?
Many women overlook the next signs entirely—especially when they seem unrelated.
Sign #5: Unexplained, Overwhelming Fatigue
Severe exhaustion that rest doesn’t resolve is one of the most commonly dismissed early symptoms of cervical cancer. The National Cancer Institute reports that significant fatigue can show up early in many cancers, sometimes connected to subtle blood loss and anemia.
This fatigue often feels “bone-deep”—reducing your capacity for work, family responsibilities, and hobbies. If tiredness is constant, unusual for you, and paired with other symptoms, it’s worth bringing up with your healthcare provider.
Signs #6–9: Weight Loss, Leg Swelling, Urinary Changes, and Bowel Issues
Some symptoms tend to appear later, but they can still matter—especially when they occur alongside earlier warning signs. These may include:
- Unexplained weight loss (for example, 10 pounds or more without trying)
- Swelling or pain in one leg
- Urinary changes (frequent urination, burning, or blood in urine)
- Bowel changes (ongoing constipation or noticeably narrower stools)
These can happen when cervical cancer affects nearby structures. The key takeaway: clusters of symptoms are often more meaningful than any single symptom on its own.
How to Stay Ahead of Cervical Cancer Symptoms
Reducing risk and catching changes early often comes down to consistent, preventive steps:
- Keep up with screening
- Pap tests are commonly recommended every 3 years for many people ages 21–65
- HPV testing may be combined or used at longer intervals (often every 5 years after age 30) depending on guidelines and history
- Consider HPV vaccination
- The HPV vaccine prevents the majority of HPV-related cases and is typically recommended through age 26, and sometimes later depending on circumstances
- Avoid smoking
- Smoking increases risk and can worsen cervical tissue health
- Act when symptoms persist
- If multiple early warning signs of cervical cancer appear—or one symptom doesn’t resolve—schedule an appointment rather than waiting
These habits don’t just support physical health; they also reduce the constant background anxiety that uncertainty creates.
3 Common Questions About Early Warning Signs of Cervical Cancer
-
What are the most common early warning signs of cervical cancer?
Abnormal bleeding, unusual discharge, pelvic pain, and pain during or after intercourse are among the most common. Any persistent or unexplained change deserves attention. -
How often should I get screened?
Many people benefit from Pap and/or HPV testing every 3–5 years depending on age and medical history. A clinician can help tailor the right schedule. -
Can lifestyle choices reduce the chance of cervical cancer?
Yes. Avoiding smoking, getting the HPV vaccine if eligible, and paying attention to persistent symptoms can lower risk and improve early detection.
A Final Mindset Shift: Turn Body Signals Into an Ally
Imagine how different you could feel 30 days from now—calmer, more informed, and more in control—because you recognize the early warning signs of cervical cancer and know when to take action. The most powerful shift is simple: when your body sends a quiet signal, treat it as useful guidance you deserve to understand, not a worry you must carry alone.