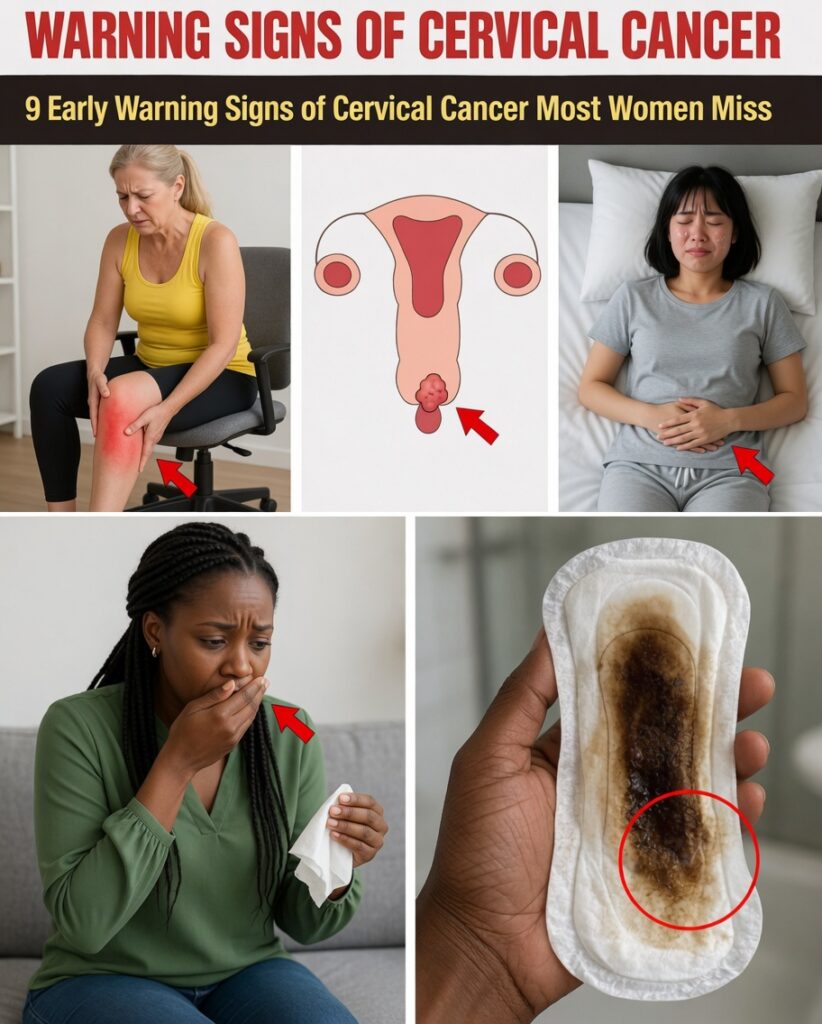
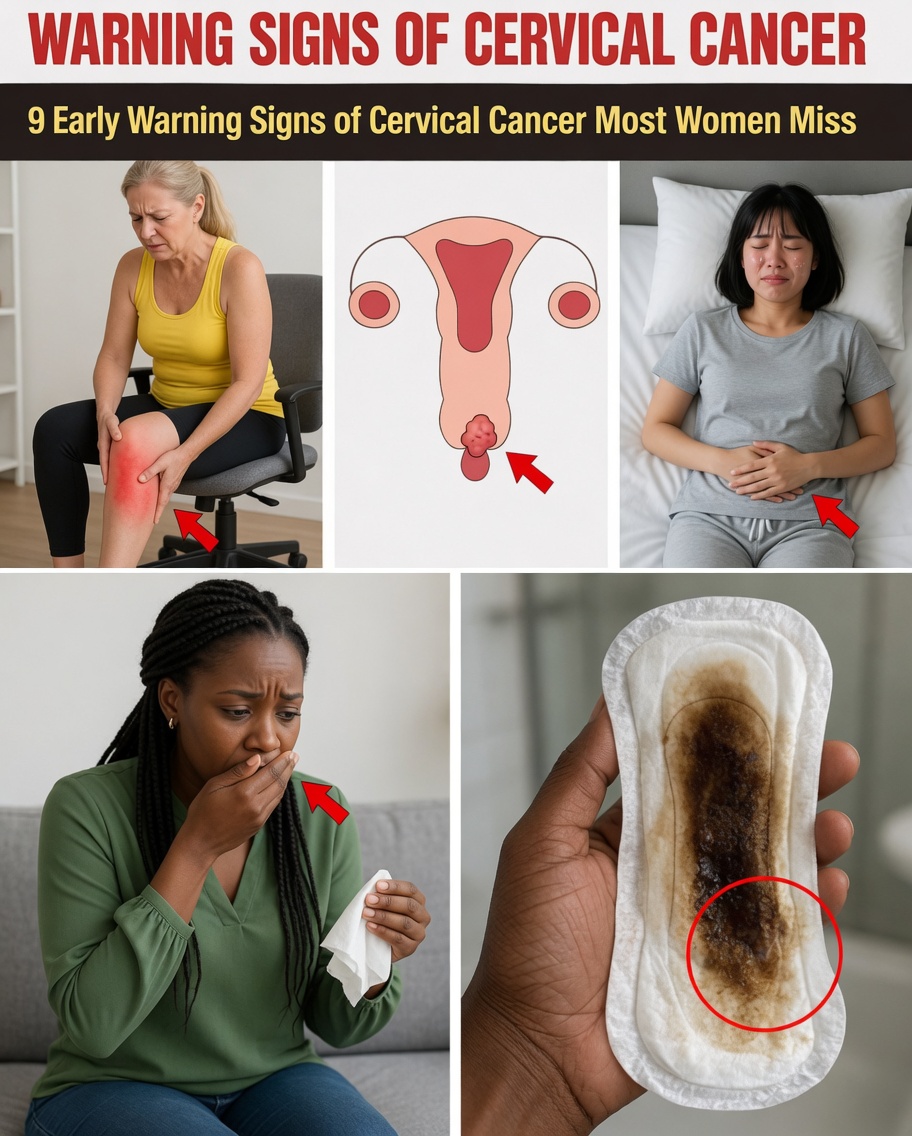
Many women notice small changes—light spotting, unusual tiredness, or discomfort—and quickly assume stress, hormones, or an overloaded schedule is to blame. Yet these subtle shifts can quietly chip away at your energy, affect your confidence at work or home, and create a persistent feeling that something isn’t quite right. Cervical cancer symptoms often develop slowly and can resemble everyday health issues, which is why paying attention early matters. The most overlooked reality is that regular screening plus body awareness is one of the strongest ways to protect your peace of mind.
Abnormal Bleeding: One of the Earliest Cervical Cancer Symptoms
Bleeding between periods, after sex, or outside your normal cycle can feel unsettling—and even embarrassing—leading you to constantly double-check dates and adjust your plans. Cervical cancer symptoms commonly include unexpected spotting because abnormal cervical tissue may bleed more easily. The American Cancer Society notes that many women experience this early sign but brush it off as “just hormones.”
Keeping a simple record of any unusual bleeding and treating it as a possible cervical cancer symptom can make it much easier to speak clearly with your healthcare provider—and reduce the anxiety of “waiting to see if it happens again.”
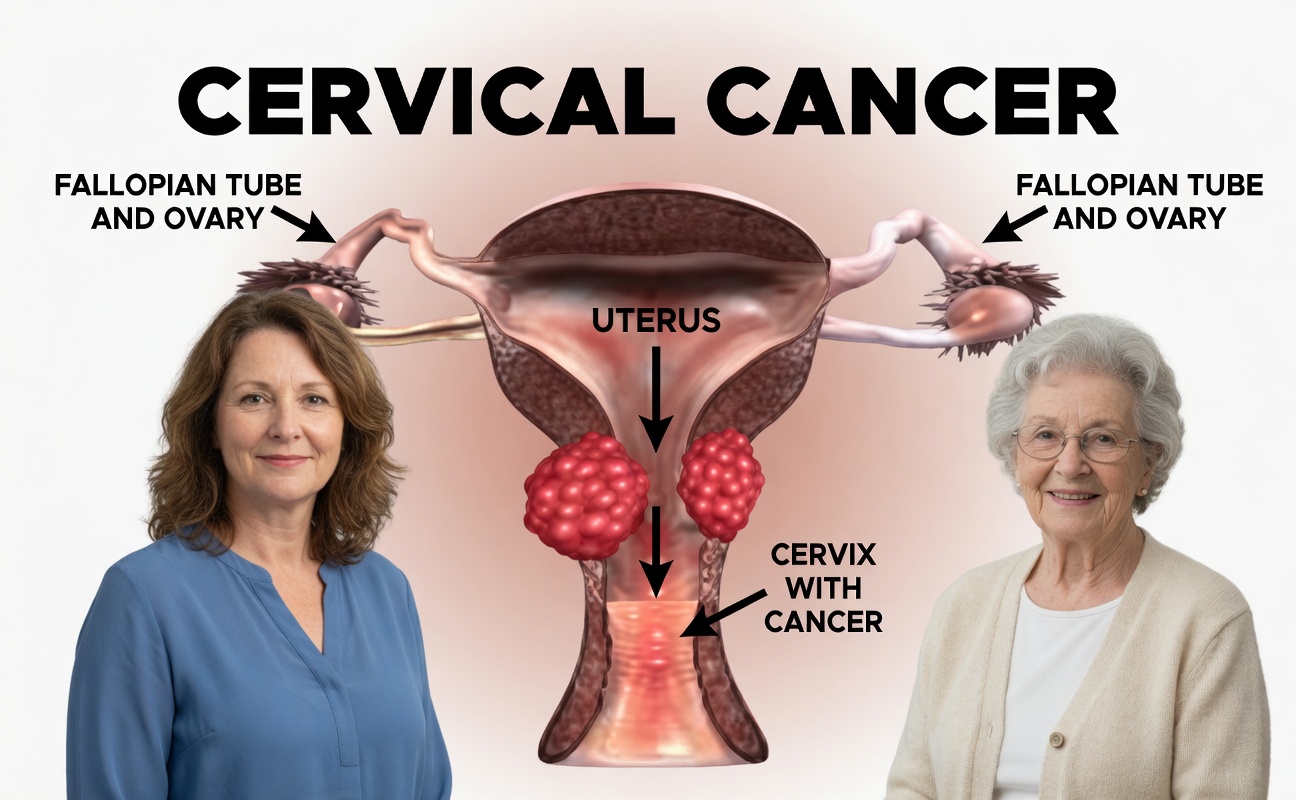
Unusual Vaginal Discharge: A Commonly Overlooked Cervical Cancer Symptom
A noticeable change in discharge—becoming watery, tinted, heavier, or stronger-smelling—can make you self-conscious throughout the day and uncomfortable during normal routines. Sometimes cervical cancer symptoms appear in this form as the cervix produces extra fluid or as tissue changes break down. The Mayo Clinic emphasizes that discharge changes that persist should be evaluated, even when they seem minor.
Once you recognize this as a potential cervical cancer symptom, tracking the pattern (color, odor, timing, and duration) can turn vague worry into a clear, actionable conversation with your doctor.
Persistent Pelvic or Lower Back Pain: An Easily Misread Cervical Cancer Symptom
A deep, lingering ache in the pelvis or lower back—especially when rest doesn’t help—can make sitting, working, or caring for children feel far more exhausting than it should. Cervical cancer symptoms may include this type of pain when growth or inflammation affects nearby structures. Health research and clinical guidance show it’s often blamed on stress, posture, or aging rather than being checked.
If pelvic or lower back pain continues, mentioning it as a possible cervical cancer symptom can reduce the constant mental burden of wondering what’s going on.

Pain During Intimacy: A Sensitive Cervical Cancer Symptom
Pain during or after sex can create emotional strain—leading to avoidance, tension in relationships, and a loss of confidence. In some cases, cervical cancer symptoms include deep or sharp discomfort because the cervix becomes more sensitive or irritated. The Mayo Clinic lists painful intercourse as a symptom worth discussing with your healthcare team.
Naming the issue and seeking professional input often brings faster relief—both physically and emotionally—than trying to manage it in silence.

Extreme Fatigue: The Cervical Cancer Symptom Many Women Dismiss
Feeling exhausted even after adequate sleep can steal your motivation, disrupt family life, and make work feel harder than usual. Cervical cancer symptoms can include significant fatigue, especially when ongoing bleeding contributes to low iron levels. The National Cancer Institute highlights that cancer-related fatigue often feels different from ordinary tiredness—more persistent and harder to “sleep off.”
If fatigue becomes constant and unexplained, treating it as a potential cervical cancer symptom and bringing it up with your provider can replace uncertainty with a plan.
Unexplained Weight Loss: Another Possible Cervical Cancer Symptom
Losing weight without changing diet or activity can create anxiety—especially when clothing fits differently or the scale continues to drop. In some cases, cervical cancer symptoms include unintended weight loss as the body responds to more advanced changes. Experts also stress that this sign has many possible causes and typically doesn’t appear on its own.
If weight loss is unexplained and persistent, discussing it as a possible cervical cancer symptom can help your doctor decide what to evaluate next.

Leg Swelling or Pain: A Less Common Cervical Cancer Symptom
Swelling, heaviness, or pain in one leg can make walking, standing, and daily errands uncomfortable—reducing your mobility and independence. While less common, cervical cancer symptoms may include leg swelling when lymphatic flow is affected, typically in later stages. Medical references note it often occurs alongside other symptoms rather than by itself.
Because leg symptoms can be linked to multiple conditions, it’s important to address persistent changes early instead of waiting for them to worsen.
Urinary or Bowel Changes: Cervical Cancer Symptoms Worth Tracking
Needing to urinate more frequently, seeing blood in urine, dealing with constipation, or noticing narrower stools can make you plan your day around bathroom access and feel constantly on edge. Cervical cancer symptoms can involve urinary or bowel changes when nearby tissues are affected. The American Cancer Society includes these shifts among symptoms that should be evaluated.
If these changes persist or appear with other signs, a single medical visit can turn daily stress into clarity and reassurance.
Simple Actions You Can Take Today to Notice Cervical Cancer Symptoms Earlier
- Track changes in bleeding, discharge, pain, or energy for two weeks in a notes app
- Book your next Pap test or HPV test if it has been more than three years
- Write a short symptom list (timing, severity, triggers) to bring to your appointment
Proven Ways to Support Cervical Health and Reduce Worry
Screening is the most reliable tool to detect cervical cell changes before most cervical cancer symptoms ever appear. The CDC recommends:
- Ages 21–29: Pap test every 3 years
- Ages 30–65: Pap + HPV test every 5 years (or Pap test every 3 years)
- HPV vaccination for eligible ages to prevent many HPV-related cervical changes
Additional supportive habits include avoiding smoking and practicing safer sex, both of which contribute to stronger overall health.
When to Talk to a Doctor About Cervical Cancer Symptoms
If any suspected cervical cancer symptoms last longer than two weeks, return repeatedly, or occur together, contact your healthcare provider promptly. Many of these signs have non-cancer causes, but professional evaluation is the fastest path to answers—and real peace of mind.
Conclusion
These nine commonly overlooked early warning signs show how the body can send quiet signals that deserve attention. Combining symptom awareness with consistent Pap and HPV screening provides the clearest, most practical path forward. With this knowledge, you can replace uncertainty with confident next steps.
FAQ
What are the earliest cervical cancer symptoms most women notice?
In many cases, early cervical cancer causes no symptoms at all. That’s why Pap and HPV tests are essential—they can detect changes long before cervical cancer symptoms begin.
Can cervical cancer symptoms be confused with perimenopause?
Yes. Irregular bleeding, fatigue, and pelvic discomfort can overlap with hormonal shifts. If symptoms persist, discuss possible cervical cancer symptoms with your doctor for proper evaluation.
How often should I screen to stay ahead of cervical cancer symptoms?
Follow age-based guidance—typically every 3 to 5 years depending on the test. Your provider may adjust the schedule based on your medical history and risk factors.