Beta Blockers and High Blood Pressure: What New Research Suggests for Women
Living with high blood pressure (hypertension) can feel like carrying a constant “what if?”—especially when complications such as heart failure are part of the long-term risk picture. Medications can bring peace of mind, but they can also raise questions about side effects and whether the same treatment works equally well for everyone.
New findings on beta blockers add an important point to discuss—particularly for women who take them for uncomplicated hypertension (high blood pressure without prior heart disease).

What the Research on Beta Blockers Found
A study published in the journal Hypertension examined outcomes in people treated for high blood pressure and found a notable difference between women and men in a specific scenario.
Researchers reported that women taking beta blockers for hypertension alone (without a history of heart disease) experienced higher rates of heart failure at hospital admission when they presented with acute coronary events, compared with men in similar circumstances.
- Among beta blocker users, women had a 4.6% higher incidence of heart failure than men.
- Importantly, this difference did not appear among patients who were not using beta blockers.
These results don’t automatically mean beta blockers are “bad”—but they do suggest that sex-based differences may matter in certain high-stress cardiac events.
Why Sex Differences With Beta Blockers Matter
Many large medical studies have historically leaned male in their participant populations, which can leave women wondering whether recommendations fully reflect their needs. In this University of Bologna-led analysis, researchers reviewed data from more than 13,000 adults with hypertension across Europe.
Their key observation: among people using beta blockers, women who arrived at the hospital with major coronary problems were more likely to develop heart failure complications.
The authors noted that these findings could support a closer look at whether beta blockers should always be considered a first-line treatment for women with uncomplicated high blood pressure.
The goal isn’t to provoke fear—it’s to encourage personalized hypertension care.
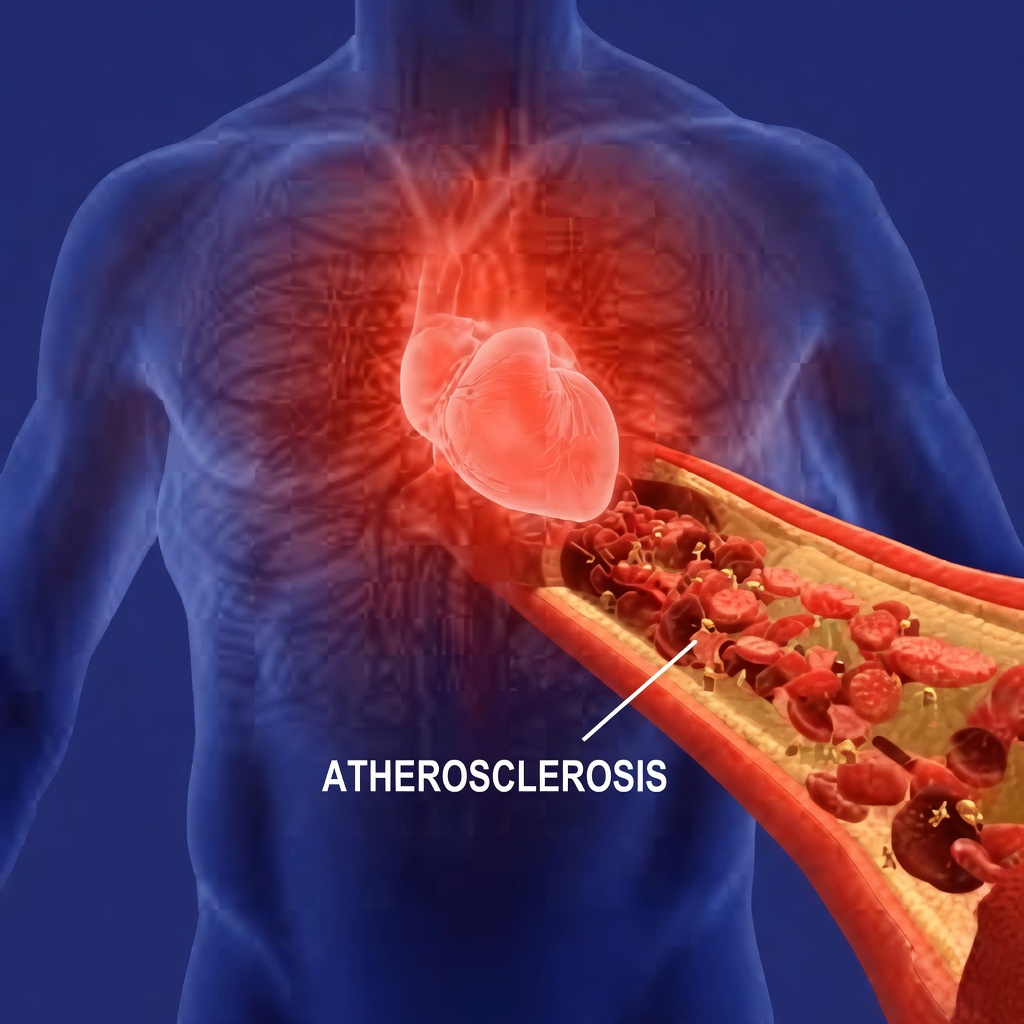
The Possible Connection During Acute Coronary Events
The study focused on patients experiencing new-onset coronary issues, including severe events such as STEMI (a major type of heart attack). In that setting:
- Women taking beta blockers showed higher heart failure rates, especially in the most serious cases.
- When heart failure occurred, mortality was significantly higher, highlighting how critical prevention and risk reduction can be.
Notably, the same male–female gap was not observed in those not taking beta blockers, which is part of what makes the finding so clinically interesting.
Key Limitations to Understand
It’s smart to read medical headlines with a critical eye. This research was observational, meaning it can identify relationships but cannot prove cause and effect.
The authors also noted that some potentially relevant factors—such as hormone therapy interactions—were not fully examined. They emphasized the need for broader clinical trials with stronger female representation to clarify how beta blockers may affect women in different scenarios.
Beta blockers remain highly valuable for many conditions (including certain heart diseases), but this research points to possible nuances for women using them for high blood pressure alone.
Lifestyle Strategies to Support Blood Pressure Naturally
If you’d like more control over your blood pressure—beyond medication—lifestyle changes can be powerful. The study’s author highlighted diet and exercise as especially important for women with hypertension and no previous heart problems.
Practical steps that can make a real difference include:
- Get 150 minutes per week of moderate activity (such as brisk walking).
- Prioritize whole foods: vegetables, fruits, lean proteins, and whole grains.
- Keep sodium under 2,300 mg per day.
- Reduce stress with mindfulness, relaxation practices, or enjoyable hobbies.
Small, consistent changes often deliver the most sustainable results.
Heart-Healthy Eating Ideas for Better Blood Pressure
If you’re managing both blood pressure and questions about beta blockers, nutrient-dense foods can support your overall routine. Consider:
- Leafy greens (like spinach) for potassium
- Berries for antioxidants
- Fatty fish for omega-3s
- Nuts and seeds (in moderation)
- Oatmeal for soluble fiber
Pair these choices with mindful portions and steady hydration to support balanced cardiovascular health.
Movement Tips That Pair Well With Blood Pressure Management
If staying active feels challenging, gentle and consistent movement can be effective without feeling overwhelming. Options include:
- Walking outdoors for both fitness and stress relief
- Yoga or tai chi for flexibility and calm
- Swimming for low-impact cardio
- Strength training twice weekly to support long-term heart and metabolic health
If you’re taking beta blockers, check with your healthcare provider before changing your exercise routine—your response to exertion can differ on these medications.
Why Awareness About Beta Blockers Matters
This beta blocker research won’t rewrite medical guidelines overnight, but it does support a more individualized approach—especially for women treating uncomplicated hypertension. Understanding potential sex-specific differences can help you ask better questions, weigh options with your clinician, and choose a plan that fits your risks and goals.
FAQ: Beta Blockers, Women, and Heart Risk
-
Are beta blockers unsafe for all women with high blood pressure?
No. The findings relate to specific circumstances during acute coronary events. Beta blockers remain beneficial for many people, and the best choice depends on individual health factors. -
Should I stop taking beta blockers after reading this?
No. Do not stop or change any medication without medical supervision. Stopping suddenly can be dangerous. -
What if I have high blood pressure but no other heart issues?
Talk with your healthcare provider about the full range of options. For many people, lifestyle measures play a major role, either alongside medication or as part of a stepwise plan.
Final Thoughts
The discussion around beta blockers and heart failure risk in women reflects how cardiovascular research continues to evolve. This study encourages thoughtful, personalized hypertension management—grounded in evidence, supported by healthy routines, and guided by open conversations with qualified professionals.
Medical disclaimer: This article is for informational purposes only and does not provide medical advice. Study findings are observational and may have limitations. Always consult a qualified healthcare professional for guidance on beta blockers, blood pressure treatment, or any health concern.



