Endometriosis: Symptoms, Causes, Diagnosis, and Everyday Relief Strategies
Many women live with severe menstrual pain, heavy bleeding, or constant tiredness and assume these issues are simply part of having a period. In reality, these symptoms can gradually affect work, relationships, daily routines, and quality of life for years before the underlying cause is recognized. The encouraging news is that better awareness can help women seek support earlier and find practical ways to manage symptoms. This guide explains the essentials of endometriosis, outlines realistic symptom-management strategies, and highlights one lifestyle factor that growing research connects with relief.
What Is Endometriosis?
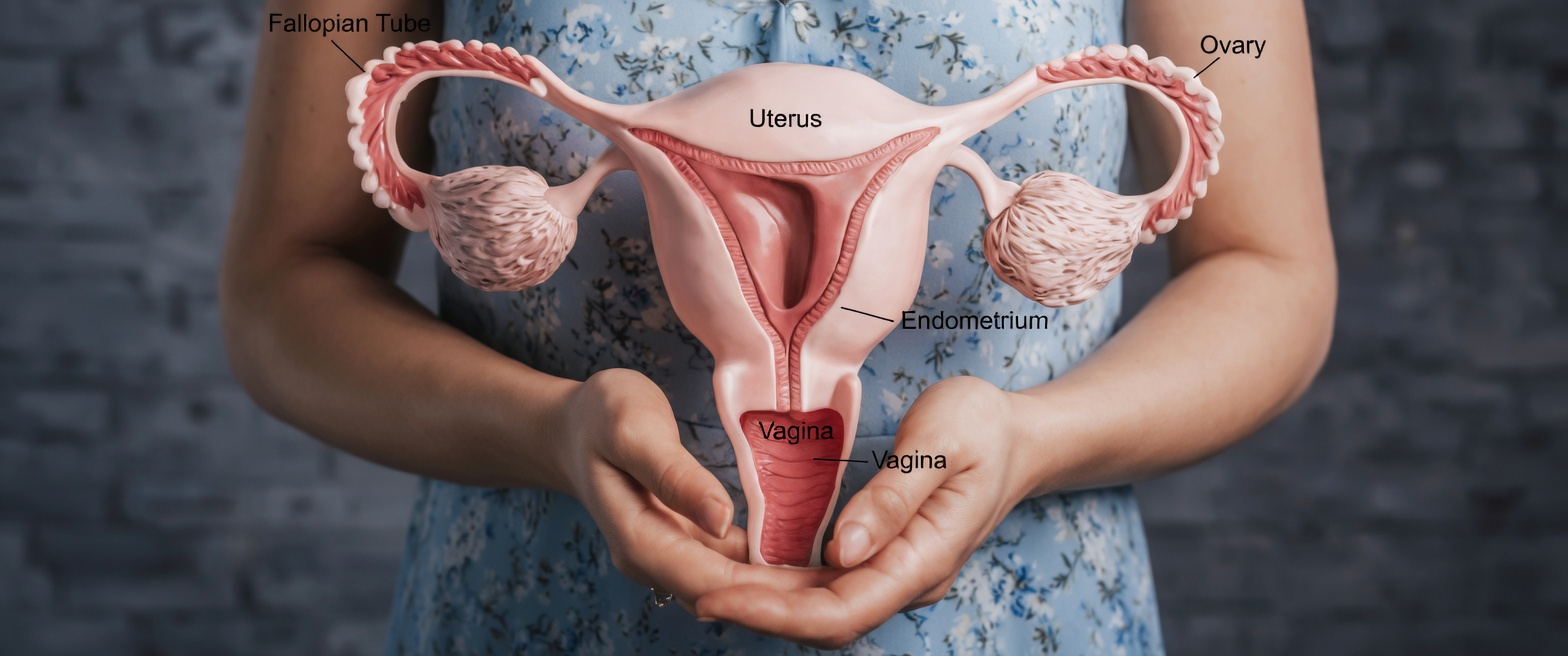
Endometriosis is a widespread health condition in which tissue resembling the uterine lining develops outside the uterus. It is often found on the ovaries, fallopian tubes, or the lining of the pelvis.
Like the tissue inside the uterus, these growths react to monthly hormonal shifts. They thicken, break down, and try to shed during the menstrual cycle. But because this tissue is outside the uterus, it cannot exit the body in the usual way.
Over time, this can trigger inflammation, irritation, and scar tissue formation. Although endometriosis is estimated to affect around 10% of women of reproductive age worldwide, many people remain undiagnosed for a long time.
Common Signs and Symptoms
Endometriosis does not look the same in every person, which is one reason it is often overlooked.
Some of the symptoms most often reported include:
- Intense menstrual cramps that become worse over time or do not respond well to standard pain medicine
- Persistent pelvic pain that continues outside of the menstrual period
- Pain during or after sex
- Heavy menstrual bleeding or spotting between periods
- Digestive symptoms such as bloating, nausea, constipation, or diarrhea during menstruation
- Constant fatigue or reduced energy
Because these symptoms can resemble other health problems, many women do not get answers quickly. According to multiple health organizations, the average delay in diagnosis can be 7 to 10 years.
There are also additional warning signs that some women notice, including pain in the lower back, discomfort in the legs, or pain during urination or bowel movements. Spotting these patterns early may help speed up the path to proper care.
What May Contribute to Endometriosis?
Researchers are still working to fully understand why endometriosis develops. While there is no single confirmed cause, several factors are believed to be involved:
- Retrograde menstruation: menstrual blood flows backward into the pelvic cavity instead of leaving the body normally
- Family history: women with close relatives who have endometriosis may have a higher risk
- Immune system differences: the body may not clear misplaced tissue effectively
- Hormonal influences: estrogen appears to encourage the growth of endometrial-like tissue
It is important to know that endometriosis is not caused by personal choices, and it cannot be passed from one person to another.
How Doctors Diagnose Endometriosis
For many women, getting a diagnosis begins with an honest conversation about symptoms.
Healthcare providers often use several steps to investigate the condition:
- A thorough discussion of symptoms, menstrual patterns, and medical history
- A pelvic exam to identify tenderness or other unusual findings
- Imaging tests such as ultrasound or MRI to examine the pelvic area
In some situations, the clearest way to confirm endometriosis is through minimally invasive surgery called laparoscopy. Speaking with a specialist early can help reduce delays and provide better clarity.
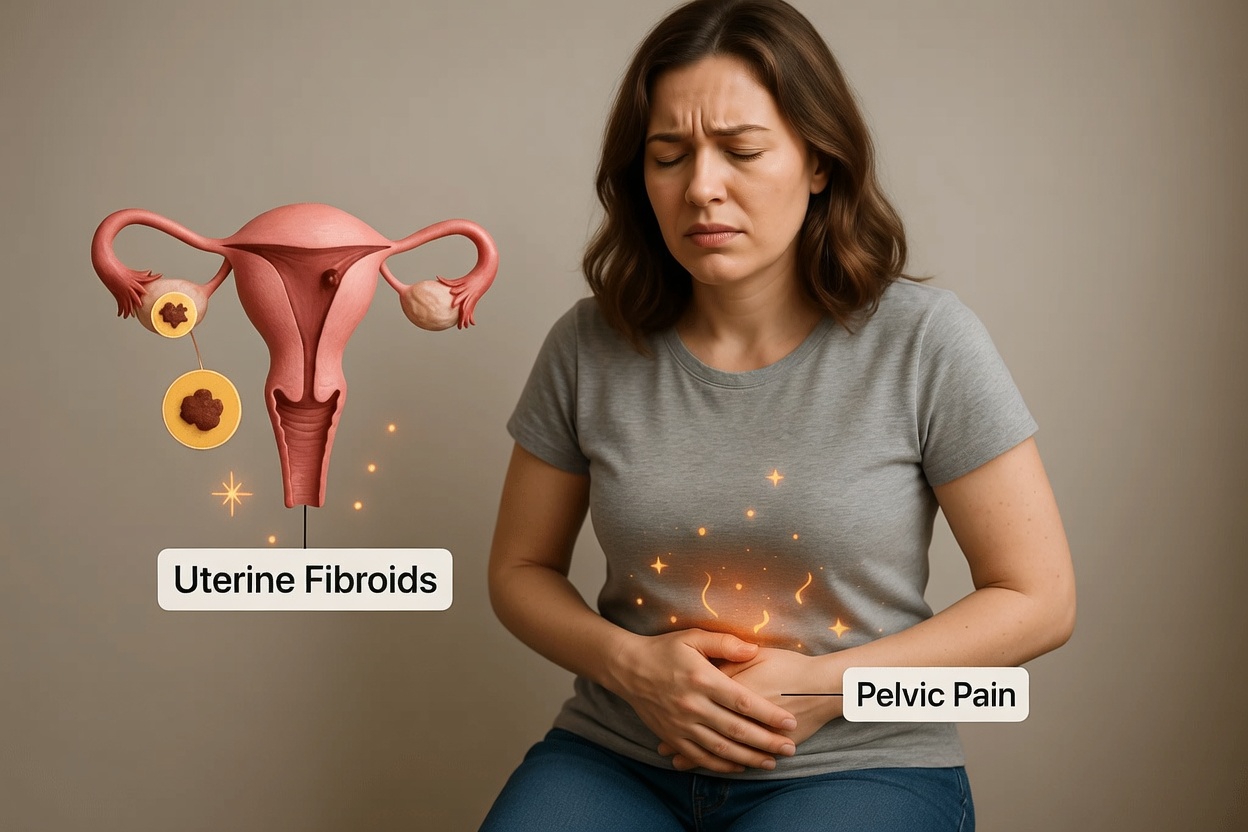
Endometriosis and Fertility
Endometriosis can make pregnancy more difficult for some women.
Research suggests that about 30% to 50% of women with endometriosis may face fertility challenges. Scar tissue may affect the fallopian tubes, while inflammation can interfere with ovulation, fertilization, or implantation.
Even so, there is reason for hope. Many women with endometriosis still become pregnant naturally or with medical treatment and go on to have healthy pregnancies and babies.
Practical Ways to Manage Symptoms
There is no universal solution for endometriosis, but several evidence-based approaches help many women improve comfort and daily functioning.
Pain Relief and Comfort Measures
Common symptom-relief options include:
- Over-the-counter anti-inflammatory medicines such as ibuprofen, especially when taken at the earliest sign of pain
- Warmth from a heating pad, hot water bottle, or warm bath
- Gentle physical activity such as walking, swimming, or yoga
Hormonal Treatment Options
Doctors may recommend hormonal therapies that reduce or pause menstrual cycles. For some women, this lowers the activity of endometrial-like tissue and eases symptoms.
Surgery for Moderate to Severe Cases
When symptoms are more serious, surgery to remove visible endometriosis tissue may offer meaningful relief. However, symptoms can come back over time, so long-term management is often still needed.
Everyday Habits That May Support Symptom Relief
Research increasingly suggests that daily lifestyle choices can play a supportive role in managing endometriosis symptoms.
Helpful habits may include:
- Regular moderate exercise to support circulation and help reduce inflammation
- Consistent, high-quality sleep
- Stress-management practices such as mindfulness, meditation, or deep breathing
- A balanced eating pattern that includes fruits, vegetables, whole grains, and omega-3-rich foods
Diet is one area receiving growing attention. Some studies indicate that cutting back on red meat and heavily processed foods while increasing fiber and anti-inflammatory foods may reduce symptoms for certain women. Foods often linked with this approach include berries, leafy greens, and oily fish.
Can Diet Help With Endometriosis?
Emerging evidence is exploring how nutrition may affect both inflammation and hormone balance in women with endometriosis.
Observational studies suggest that:
- Eating more fruits, vegetables, and omega-3 fatty acids may be linked to milder symptoms in some women
- Diets high in trans fats or red meat may be associated with greater risk
- Fiber-rich foods may support healthier estrogen metabolism
Diet alone does not eliminate endometriosis, but many women say they feel better when they adopt more mindful eating habits.
A simple way to begin may include:
- Add one more serving of colorful vegetables to each meal
- Swap refined grains for whole-grain options
- Include healthy fats such as olive oil, nuts, seeds, or avocado
- Drink enough water throughout the day
- Keep track of symptoms and food intake for a few cycles to notice patterns
In many cases, small and consistent changes are easier to maintain than a dramatic diet overhaul.
Living Better With Endometriosis
Managing a chronic condition often requires time, flexibility, and support.
Support groups and online communities can help women feel less alone. Open conversations with partners, close friends, or family members can also make day-to-day coping easier.
Most importantly, working with a healthcare professional who understands endometriosis can help create a treatment plan tailored to individual symptoms, goals, and lifestyle.
Frequently Asked Questions
How common is endometriosis?
Endometriosis affects about 1 in 10 women of reproductive age worldwide, although the true number may be higher because diagnosis is often delayed.
Can endometriosis disappear on its own?
Symptoms may lessen after menopause as estrogen levels drop naturally, but the tissue itself may still remain.
When should I talk to a doctor about period pain?
If menstrual pain regularly disrupts school, work, social life, or everyday activities, it is a good idea to speak with a healthcare provider as soon as possible.
Disclaimer
This article is for informational purposes only and does not replace medical advice. Always speak with a qualified healthcare professional for personal concerns, diagnosis, or treatment options.