Subtle Colon Cancer Signals You Might Be Overlooking
Many people notice small changes in their bodies and chalk them up to stress, diet, or simply aging. When these subtle shifts continue without a clear reason, they can quietly fuel ongoing worry and disturb your sense of well-being. Ignoring early, silent colon cancer symptoms often increases anxiety as your body keeps sending gentle warnings.
The encouraging part: tuning in to these changes allows you to speak more confidently with your doctor and take straightforward steps toward peace of mind. Keep reading to the end for a clear screening timeline recommended by experts and specific questions you can bring to your next appointment to stay proactive about your health.
Silent Sign #1: Abdominal Discomfort You’ve Learned to Tolerate
One of the most frequent silent colon cancer symptoms is long-lasting abdominal discomfort that’s easy to blame on gas, indigestion, or a hectic lifestyle. Ongoing cramping or a dull ache can leave you worn out and irritable, turning ordinary meals into something you quietly dread.
Research shows many adults minimize these early warnings for months before seeking medical advice. When your stomach feels “off” more days than not, it subtly adds strain to your daily life.
The challenge with these early signals is that they often start so mildly that you simply adjust and keep going, instead of asking why they are there in the first place.
Silent Sign #2: New Bowel Habits That Start to Feel “Normal”
Another common cluster of silent colon cancer symptoms involves noticeable changes in bowel habits, such as:
- New or worsening constipation
- Looser or more frequent stools
- Alternating between constipation and diarrhea
Over time, many people begin to treat these changes as their “new normal,” even though they bring embarrassment, inconvenience, and low-level stress. Medical studies suggest that unexplained shifts in bowel patterns—especially in adults—should be taken seriously and discussed with a healthcare professional.
You deserve a daily routine that doesn’t involve worrying about every trip to the bathroom.
Silent Sign #3: Consistently Pencil-Thin Stools
Stools that repeatedly look narrower or more “pencil-thin” than they used to be are another often-overlooked warning sign. People may joke about it or brush it off, but the concern tends to linger in the back of the mind.
Experts note that ongoing changes in stool shape can sometimes indicate a narrowing in the colon and may be linked to silent colon cancer symptoms. While a single episode is usually not a cause for alarm, a pattern that persists is worth mentioning to your doctor.
Silent Sign #4: Blood You Blame on Something Minor
Noticing blood on the toilet paper, in the toilet bowl, or mixed with stool is commonly attributed to hemorrhoids, straining, or a small tear. Because these explanations seem harmless, many people stay silent, even as the worry grows.
Healthcare guidelines emphasize that repeat or persistent bleeding should be evaluated, as it can be one of the silent colon cancer symptoms. You do not have to shoulder that uncertainty by yourself—bringing it up can lead to clarity and timely care.
Level 1 Milestone: The First Four Symptoms Many Doctors Hear About
By this point, you’ve seen four early warning signs that frequently appear in patient stories and medical appointments. Recognizing them is a powerful first step toward protecting your colon health.

Mid-Article Self Check
Take a brief moment to reflect before continuing:
- How many of these subtle colon signals have you noticed in yourself or a loved one?
- Is there a symptom you’ve been shrugging off or telling yourself is “no big deal”?
- Are you ready to look at the next group of possible warning signs with an open mind?
- If you’ve been feeling tired, how would you rate your fatigue right now on a scale of 1–10, and has reading this changed that awareness?
- Still reading? That persistence will pay off as the next sections become even more practical and action-focused.
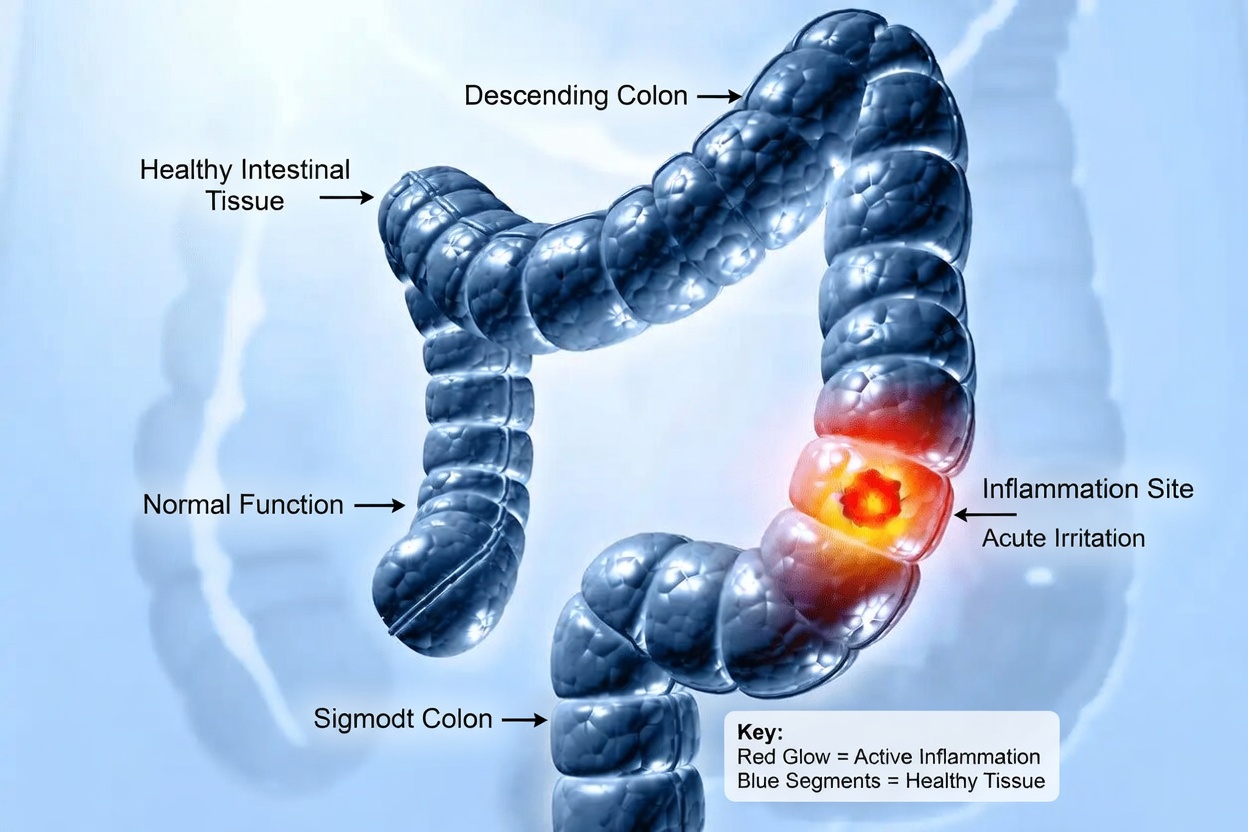
Silent Sign #5: Feeling Like You Never Completely Empty
That nagging sensation of not fully emptying your bowels—even after you’ve just gone—can be one of the more frustrating silent colon cancer symptoms. This lingering feeling can:
- Make you feel uneasy or distracted throughout the day
- Lower your confidence in social or work settings
- Gradually drain your emotional energy over weeks or months
Living with that constant “unfinished” sensation should not be your norm. If it continues, it’s worth discussing with a medical professional.
Silent Sign #6: Unexplained Iron-Deficiency Anemia
Iron-deficiency anemia without a clear cause—such as heavy menstrual bleeding, a known medical condition, or dietary issues—is another red flag, especially in adults over 40. When related to the colon, it often appears as:
- Persistent low energy
- Shortness of breath with mild exertion
- Pale skin or frequent lightheadedness
Respected medical organizations acknowledge that unexplained anemia can sometimes be tied to blood loss in the digestive tract, including from colon cancer. Identifying the cause can lift the heavy fog of exhaustion and restore your sense of vitality.
Silent Sign #7: Fatigue That Rest Doesn’t Solve
Almost everyone feels tired at times, but fatigue associated with silent colon cancer symptoms often feels different. You might notice:
- Sleep doesn’t refresh you the way it used to
- Simple tasks feel unusually demanding
- Your motivation and mood are consistently lower
When tiredness becomes a constant background presence rather than an occasional response to a busy week, it deserves attention. You are entitled to days where you feel genuinely energized, not just pushing through.
Silent Sign #8: Ongoing Bloating or Midsection Pressure
Bloating that appears suddenly and doesn’t ease up can be more than just a reaction to food. People often report:
- A tight, swollen feeling in the abdomen
- Discomfort during meals, meetings, or sitting for long periods
- Increased self-consciousness about their midsection
When bloating persists without a clear dietary trigger, it may be one of the silent colon cancer symptoms that disrupt daily comfort. Addressing the cause can help you feel at ease in your body again.
Silent Sign #9: Nausea or Vomiting You Blame on Something You Ate
Recurring nausea, queasiness, or vomiting is easy to attribute to a “sensitive stomach” or a particular meal. However, when these episodes become frequent, they can create:
- Anxiety around eating or social gatherings that involve food
- Worry about your overall health and digestion
- A cycle of guessing, restricting, and still not feeling better
When nausea is related to colon issues, clarifying the cause and treating it appropriately can bring significant relief. Instead of guessing, you can understand what your body is trying to communicate.
Silent Sign #10: Shortness of Breath During Everyday Activities
Feeling unusually winded while climbing stairs, walking a short distance, or doing routine tasks can sometimes be linked to anemia or fatigue associated with colon disease. This can:
- Limit your independence and activity level
- Spark concern about your heart, lungs, or overall health
- Make once-simple tasks feel overwhelming
Recognizing that this could be one part of a broader pattern of silent colon cancer symptoms allows you to seek targeted evaluation and support. The goal is to move through daily life with more ease and confidence.
When to Talk About Screening: A Practical Timeline
Understanding when to start screening helps you turn awareness into action. Use this overview as a starting point for conversations with your doctor about your risk level and any symptoms you’ve noticed.

General Screening Guidance (May Vary by Country and Guidelines)
| Risk Level | When to Start the Conversation | Typical Screening Frequency | Common First-Line Test |
|---|---|---|---|
| Average risk | Around age 45 | About every 10 years | Colonoscopy |
| Family history | Around age 40, or 10 years before the youngest relative’s diagnosis | About every 5 years | Colonoscopy |
| Current symptoms | As soon as possible, regardless of age | As your doctor recommends | Colonoscopy or other tests |
These timelines are general, not one-size-fits-all. They give you a clear, confident starting point to discuss your own situation rather than waiting in uncertainty.
Symptoms vs. Common Explanations: A Quick Comparison
It’s easy to assume everyday causes. Use this comparison to know when to look deeper:
-
Blood in stool
- Common explanation: Hemorrhoids, minor tears, or straining
- When to look closer: If it recurs or persists for more than about two weeks, it should be assessed as a potential warning sign.
-
Abdominal pain or cramping
- Common explanation: Gas, food intolerance, or stress
- When to look closer: If it continues for weeks, worsens, or doesn’t match your usual patterns, it may warrant evaluation.
-
Changes in bowel habits
- Common explanation: Diet changes, infections, travel, or temporary illness
- When to look closer: If altered patterns last longer than a few weeks or keep returning, they should not be ignored.
-
Unexplained fatigue
- Common explanation: Busy schedule, poor sleep, or stress
- When to look closer: If rest doesn’t help, or fatigue is paired with other symptoms such as anemia, weight changes, or bleeding, talk with your doctor.
Practical Steps You Can Take Today
You don’t need to have all the answers before reaching out for help. Simple actions can make a big difference in how prepared and calm you feel.

-
Track your symptoms for one week
- Jot down any abdominal pain, bowel changes, bleeding, fatigue, or other concerns. Note timing, frequency, and what you were eating or doing.
-
Schedule a medical appointment if two or more symptoms persist
- Especially if they have been present for several weeks or are getting worse.
-
Bring focused questions to your visit
- For example:
- “Could these symptoms indicate something more serious?”
- “Are they consistent with colon issues, or do they suggest something else?”
- “What tests would help rule out colon cancer?”
- For example:
-
Ask about screening based on your age and family history
- Discuss whether a colonoscopy or another screening test is appropriate for you right now, even if your symptoms are mild.
-
Share your notes honestly
- Being open about what you’re experiencing often reduces anxiety and helps your provider see the full picture.
Key Takeaways for Moving Forward
Paying attention to subtle colon changes is not about alarm—it’s about informed self-care. Recognizing potential silent colon cancer symptoms empowers you to:
- Act earlier rather than waiting in worry
- Have better-quality, more focused conversations with healthcare professionals
- Access tests and treatment options at a stage when they are often most effective
Many people feel a significant sense of relief once they stop ignoring their symptoms and start seeking answers. Listening to your body with curiosity, not fear, can make your health journey feel lighter and more manageable.
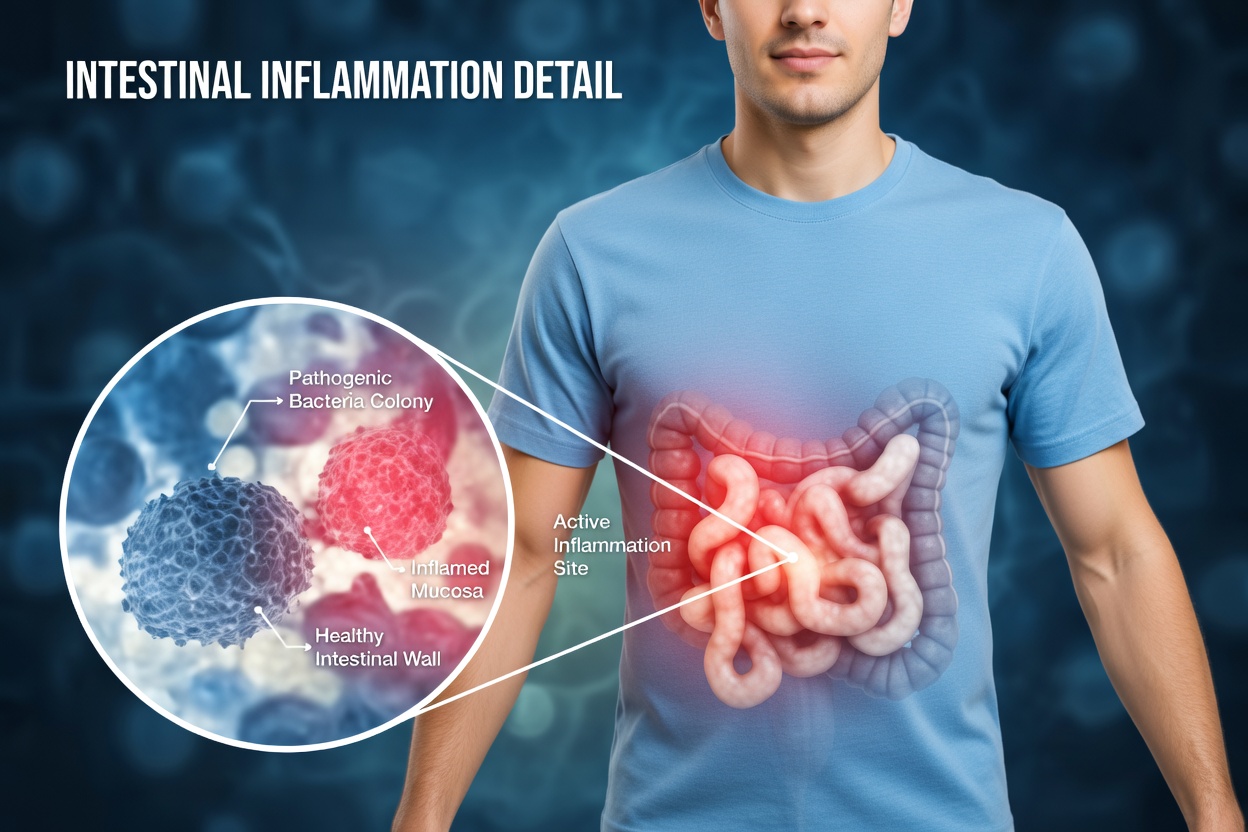
Frequently Asked Questions
Are silent colon cancer symptoms the same as IBS or stress?
Not necessarily. Silent colon cancer symptoms can overlap with conditions like irritable bowel syndrome (IBS) or stress-related digestive issues. The key differences are:
- Duration: Symptoms that last beyond a few weeks or keep coming back deserve medical review.
- Pattern: New or changing patterns—especially after age 40—are more concerning.
- Additional signs: Unexplained weight loss, blood in stool, or anemia make evaluation even more important.
Only a healthcare professional can distinguish between IBS, stress-related symptoms, and more serious causes.
At what age should someone start talking about colon cancer screening?
Guidelines often recommend:
- Average-risk adults: Begin discussing screening around age 45.
- Higher-risk adults: Start earlier if you have a family history of colon cancer or certain genetic conditions—sometimes around age 40 or even younger, based on your situation.
Your doctor can help personalize the timing based on your age, medical history, and any symptoms you are experiencing.
How do doctors evaluate possible silent colon cancer symptoms?
Evaluation usually begins with a conversation and basic exam, then may include:
- Detailed medical history: Your symptoms, family history, medications, and lifestyle factors.
- Physical and rectal exam: To check for tenderness, masses, or obvious abnormalities.
- Blood tests: To look for anemia, inflammation, or other clues.
- Stool tests: To detect hidden (occult) blood or other markers.
- Imaging or endoscopic tests: Most commonly a colonoscopy, which allows direct viewing of the colon and removal or biopsy of any suspicious areas.
Your doctor will recommend specific tests based on your risk level and symptom pattern, with the goal of finding clear answers and guiding appropriate next steps.