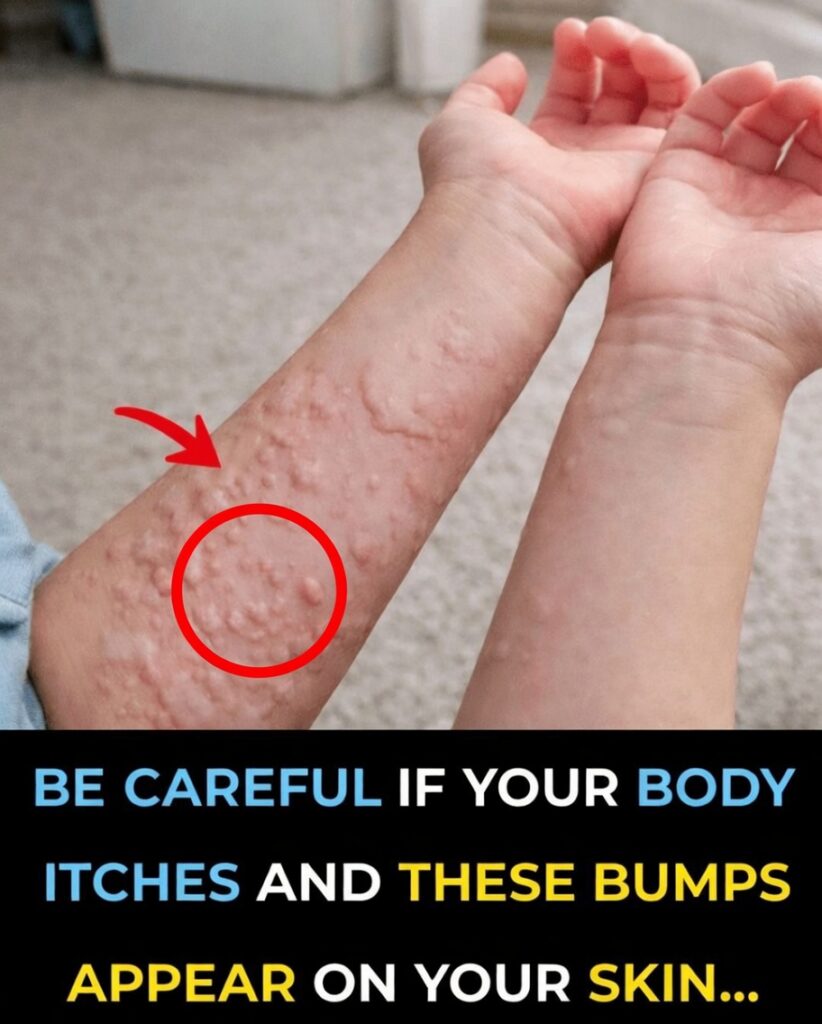
When Itchy Red Bumps Suddenly Take Over Your Skin
Imagine opening your eyes one morning and realizing your arms and legs are dotted with red, raised, intensely itchy bumps. The urge to scratch is constant. Throughout the day, even simple tasks feel distracting and uncomfortable, and at night the itching can rob you of sleep. What seemed like a small irritation quickly starts to affect your mood, confidence, and daily rhythm. You might find yourself asking: Why is my skin reacting like this out of nowhere?
What many people never realize is that some of the most powerful triggers are woven into everyday life—and one of the most overlooked factors only becomes obvious once you understand how all the pieces fit together.
Your skin is sending you signals through these itchy welts. Learning to interpret those signals can bring real relief and clarity. This reaction is extremely common, and the better you understand daily triggers, the easier it becomes to connect the dots and take back control.
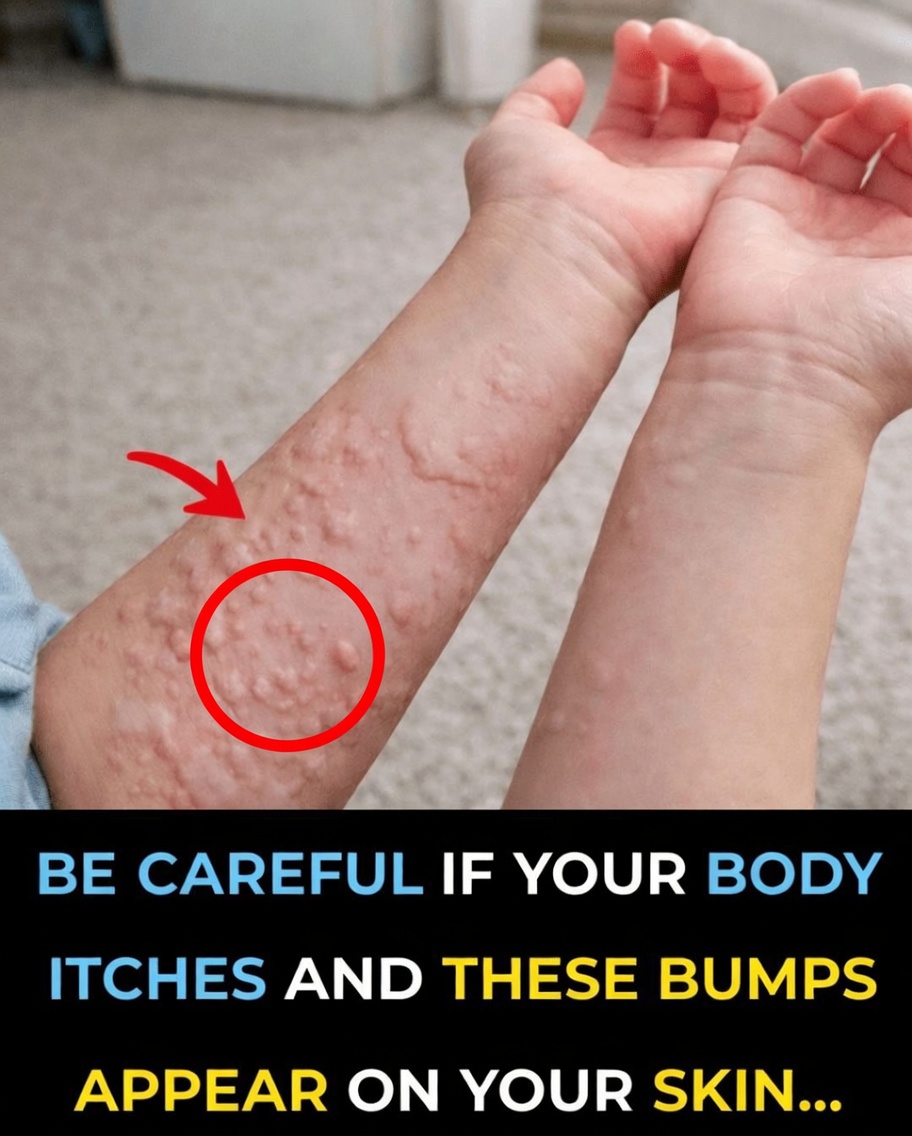
What’s Actually Happening in Your Skin?
Those red, raised, itchy patches are often referred to as hives (or “urticaria”). They appear when your body releases a natural chemical called histamine. Histamine makes tiny blood vessels in the skin leak fluid, which builds up and forms the swollen bumps you see and feel.
These welts can:
- Pop up anywhere on your body
- Change size, shape, or location quickly
- Vanish within a few hours—and then unexpectedly return later
According to information from organizations like the Cleveland Clinic, these flare-ups are usually grouped into:
- Acute reactions: lasting less than six weeks
- Chronic reactions: continuing, off and on, for more than six weeks
The challenge is that hives don’t always have a single, obvious cause. Often, the key isn’t one event but patterns over time. And those patterns can involve everyday factors you might never suspect.
Common Everyday Triggers You Probably Expect
Allergic reactions are among the most familiar reasons people develop itchy red bumps. Certain foods and medications are especially well-known for kick-starting this response in sensitive individuals.
Food triggers
Some of the most frequently reported foods include:
- Peanuts and other tree nuts
- Shellfish (such as shrimp, crab, or lobster)
- Eggs
- Cow’s milk
- Certain fruits and berries
For many people, these foods can cause symptoms within minutes to a few hours after eating.
Medication triggers
Medications are another major source of trouble. Allergy specialists often mention:
- Antibiotics: especially penicillin and related drugs
- Pain relievers: such as aspirin and ibuprofen (NSAIDs)
- Other prescriptions: including some blood pressure or heart medications
Other common exposures
Everyday environmental or contact triggers can also be involved, such as:
- Pollen
- Pet dander (from cats, dogs, and other animals)
- Latex (gloves, balloons, elastic in clothing)
- Insect bites or stings
The American College of Allergy, Asthma & Immunology notes that these types of triggers often cause rapid-onset reactions. Writing down what you ate, touched, or took shortly before the bumps appeared can reveal patterns that might otherwise be easy to miss.
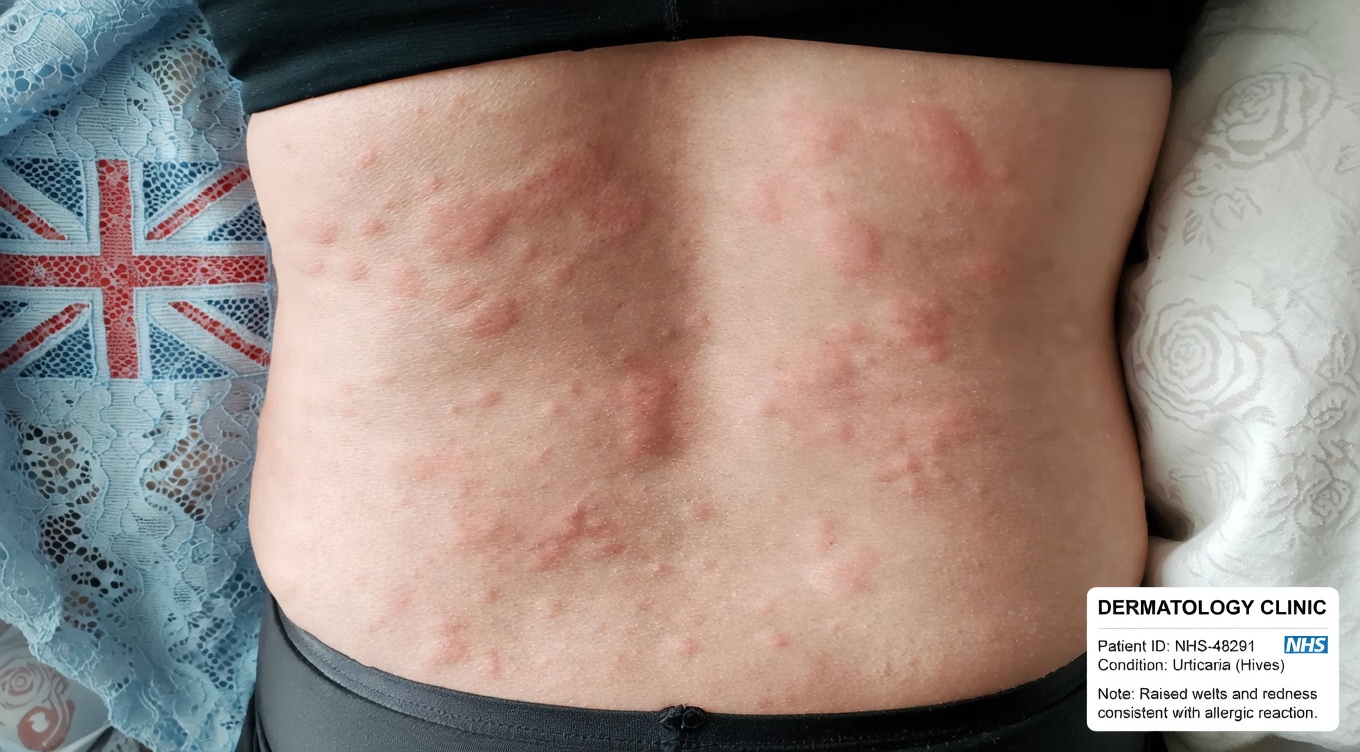
Surprising and Hidden Triggers You Might Miss
Here’s where things get more unexpected: not all hives are caused by allergies. Physical factors—things your skin experiences from the outside world—can trigger the same kind of itchy bumps with no food or drug involved at all.
Common “physical” triggers include:
- Heat: hot showers, saunas, or overheated rooms
- Cold: chilly wind, cold water, or ice packs
- Sunlight: direct sun exposure on uncovered skin
- Pressure: tight waistbands, snug watch bands, bra straps, backpack straps, or even sitting for long periods
- Vibration: from jogging, using power tools, or riding in certain vehicles
Exercise that raises your internal temperature, or even strong emotional reactions, can provoke histamine release in some people. In addition, infections are a major—and often overlooked—piece of the puzzle.
According to resources from the Mayo Clinic, common infections associated with hives can include:
- Colds or respiratory infections
- Strep throat
- Urinary tract infections
- Other viral or bacterial illnesses
Sometimes, an underlying health issue such as a thyroid imbalance or another internal condition can also contribute. These possibilities are best evaluated with a healthcare professional.
Even with careful investigation, up to half of chronic cases never reveal one clear cause. Specialists call these “idiopathic” hives, meaning the exact trigger remains unknown. That can be frustrating, but recognizing broader patterns still offers important guidance.
Everyday examples that catch people off guard
- Someone wears a snug fitness tracker all day and develops bumps exactly under the band.
- Another person finishes a stressful day at work, notices no new foods or medications, yet breaks out in itchy patches that evening.
These scenarios show how physical pressure, temperature changes, and stress—things that feel routine and harmless—can be key pieces of the story.
Is Stress – and Your Routine – Making It Worse?
Stress is one of the most underestimated triggers for itchy skin reactions. When your stress levels rise, your body releases a cocktail of chemicals that can include histamine or can influence how your immune system behaves. The result: emotional pressure becomes visible on your skin.
Other lifestyle-related triggers that raise body temperature or irritate the skin can have a similar effect, such as:
- Intense exercise or workouts in hot environments
- Hot baths or showers
- Spicy foods that cause flushing or sweating
- Tight or synthetic clothing that traps heat and rubs the skin
The Mayo Clinic also highlights how several physical factors—pressure, heat, cold, sunlight, and vibration—belong to a group of often overlooked triggers. Many people live with these influences daily without connecting them to their rashes.
This combination is what surprises so many people: your normal routine—your clothes, your stress level, your environment—may be quietly contributing to your itchy bumps.
Simple Ways to Track Your Personal Triggers
You don’t need complicated tools to start decoding your own patterns. A basic daily log can be incredibly revealing if you use it consistently.
Here’s a practical approach:
-
Record timing
- Note exactly when the bumps appeared.
- Write down what you did in the 1–2 hours before they started.
-
Track food and medication
- List everything you ate and drank.
- Include all medications and supplements, even over-the-counter ones.
-
Note environment and activity
- Weather details: hot, cold, humid, windy, sunny?
- Activities: exercise, hot shower, time in the sun, wearing a backpack, long drive, etc.
-
Rate your stress level
- Use a 1–10 scale to capture how stressed, anxious, or overwhelmed you felt that day.
- Add major events (deadlines, arguments, big presentations).
-
Check clothing and pressure points
- Record whether you wore tight clothing, belts, shoes, or accessories that press on your skin.
-
Take photos
- Photograph the bumps once a day or when they change noticeably.
- Note where they appear and how intense the reaction looks.
-
Review your week
- At the end of the week, scan your notes for repeated combinations: same food, same activity, same time of day, similar stress level, or ongoing pressure on the same area.
Experts at the ACAAI often recommend this kind of food and activity diary because it transforms guesswork into usable evidence. Many people discover that their flare-ups link back to something as simple as a hot soak in the tub, a tight waistband, or a consistently stressful meeting.
Another practical step: favor loose, breathable fabrics and try to avoid sudden changes in temperature when you can. These small adjustments can reduce irritation while you’re still figuring out your specific triggers.
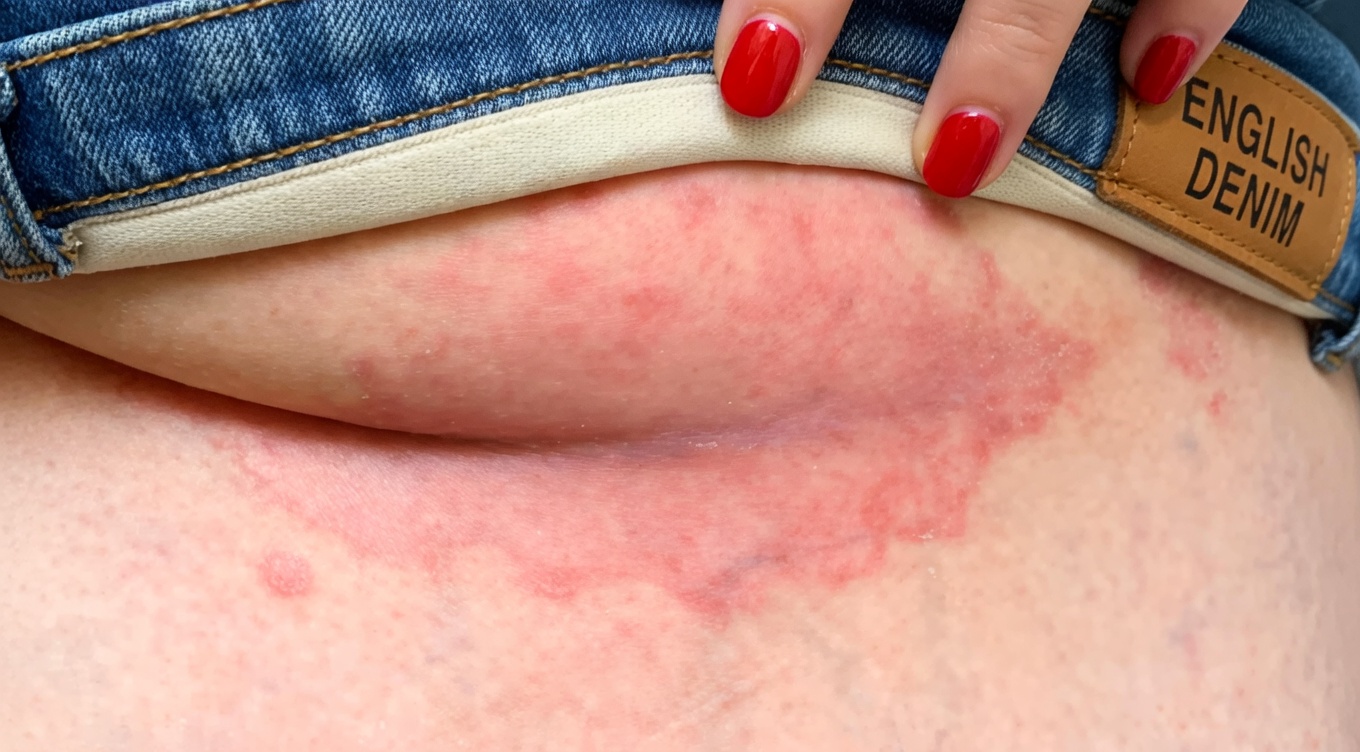
Patterns That Deserve Extra Attention
If your itchy bumps:
- Keep coming back regularly, or
- Persist on and off for more than a few weeks
it’s worth paying close attention to the patterns in your notes.
Often, repeated reactions relate to:
- Pressure on specific skin areas
- Regular exposure to heat, cold, or sunlight
- Ongoing stress at work or at home
- Recurrent infections or feeling “run-down” frequently
Most importantly, listen to your body. If the itching disturbs your sleep, interferes with daily activities, or leaves you feeling anxious or frustrated, sharing your observations with a healthcare professional can be extremely helpful. Bringing your diary and photos to an appointment gives your doctor or allergist a clearer picture and may lead to more targeted suggestions or testing.
Final Thoughts: Turning Confusion into Clarity
Itchy red bumps don’t have to remain a total mystery. Once you understand how many different factors can be involved—from food and medications to stress, pressure, infections, and temperature changes—you gain a better sense of what might be happening in your own life.
The goal is not instant perfection but steady awareness:
- Notice what your skin is trying to tell you.
- Watch for repeated patterns rather than chasing one single cause.
- Use small, practical changes to see how your skin responds.
One especially surprising trigger for many people? The combination of everyday emotional stress, tight clothing, and temperature shifts. On their own, each factor may seem minor. Together, they can tip your skin into a reaction. Recognizing that combination has helped countless people finally see the connection between their lifestyle and their skin.
Stay curious about your body’s signals. A little patience, attention, and tracking can make a meaningful difference in how comfortable you feel day to day.
Frequently Asked Questions
How long do these itchy bumps usually last?
Individual hives often fade within 24 hours, sometimes much sooner. However, new bumps can appear as old ones disappear, so the overall episode may last several days or even weeks. When this pattern continues on and off for longer than six weeks, doctors often refer to it as chronic hives, and tracking triggers becomes especially important.
Can certain foods or everyday activities really cause recurring skin reactions?
Yes. Many people discover clear patterns once they start writing things down. Foods such as nuts, shellfish, eggs, and dairy products frequently appear in reports from allergy organizations. At the same time, physical triggers—like heat, cold, pressure from clothing, intense exercise, or sun exposure—can cause repeated flare-ups even when no new foods or medications are involved.
What if the bumps keep coming back even after avoiding obvious triggers?
Recurring reactions are common and don’t always have a single identifiable cause. In some cases, the hives are idiopathic, meaning no clear trigger can be found. If your bumps persist, come back regularly, or are severe, it’s wise to:
- Share your symptom diary and photos with a healthcare professional or allergist
- Discuss possible hidden triggers, such as infections, thyroid issues, or other underlying conditions
- Ask whether allergy testing, blood work, or other evaluations might be appropriate
Professional guidance, combined with your own careful tracking, offers the best chance of understanding and managing these stubborn skin reactions.