Fatty Liver Disease: The Silent Threat Hiding in Plain Sight
Millions of adults in the United States are living with fatty liver disease without realizing it. In the early stages, this condition often causes no obvious symptoms, yet it quietly affects one of the body’s most important organs. Persistent tiredness, subtle skin changes, and vague aches or discomfort that many people blame on stress or aging may actually be early signs of a fatty liver.
Recognizing these clues and learning how to support your liver can help you work with your healthcare provider to protect your long-term liver health. Below, you’ll discover key warning signs, how common fatty liver disease really is, and everyday habits that may help support your liver.
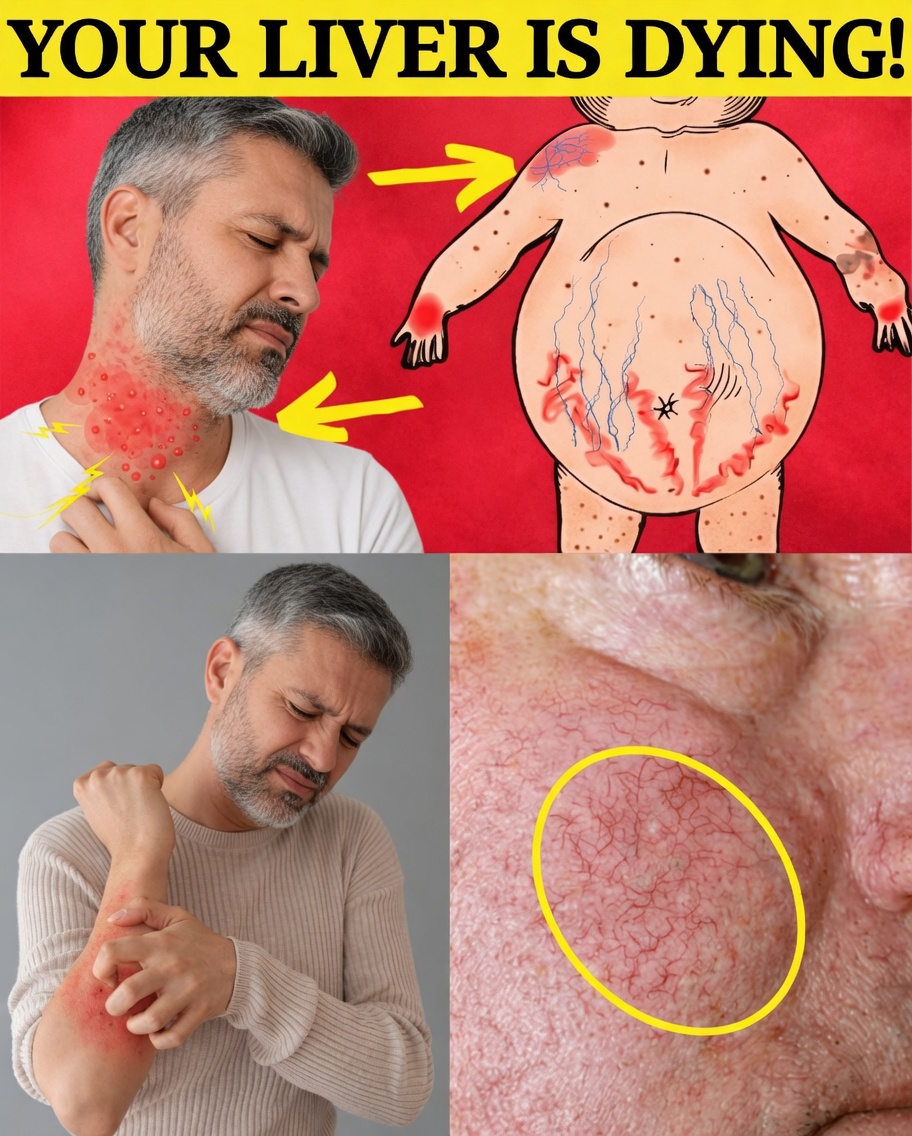
Why Fatty Liver Disease Is Known as a “Silent” Condition
Fatty liver disease has become one of the most common liver problems worldwide. It is closely associated with:
- Insulin resistance
- Excess abdominal (belly) fat
- Diets high in ultra-processed foods, refined carbohydrates, and added sugars
- Sedentary or low-activity lifestyles
These factors gradually promote fat buildup inside the liver. The challenge is that many people feel perfectly fine while this damage is developing. Symptoms often appear only when the condition progresses, which is why it’s so important to notice early warning signs and risk factors.
8 Subtle Signs That May Suggest Fatty Liver Disease
Many people with fatty liver disease report small but noticeable changes that can easily be dismissed or misattributed. Paying attention to these signals can prompt earlier discussions with your healthcare provider.
Here are eight signs that may be associated with fatty liver disease:
-
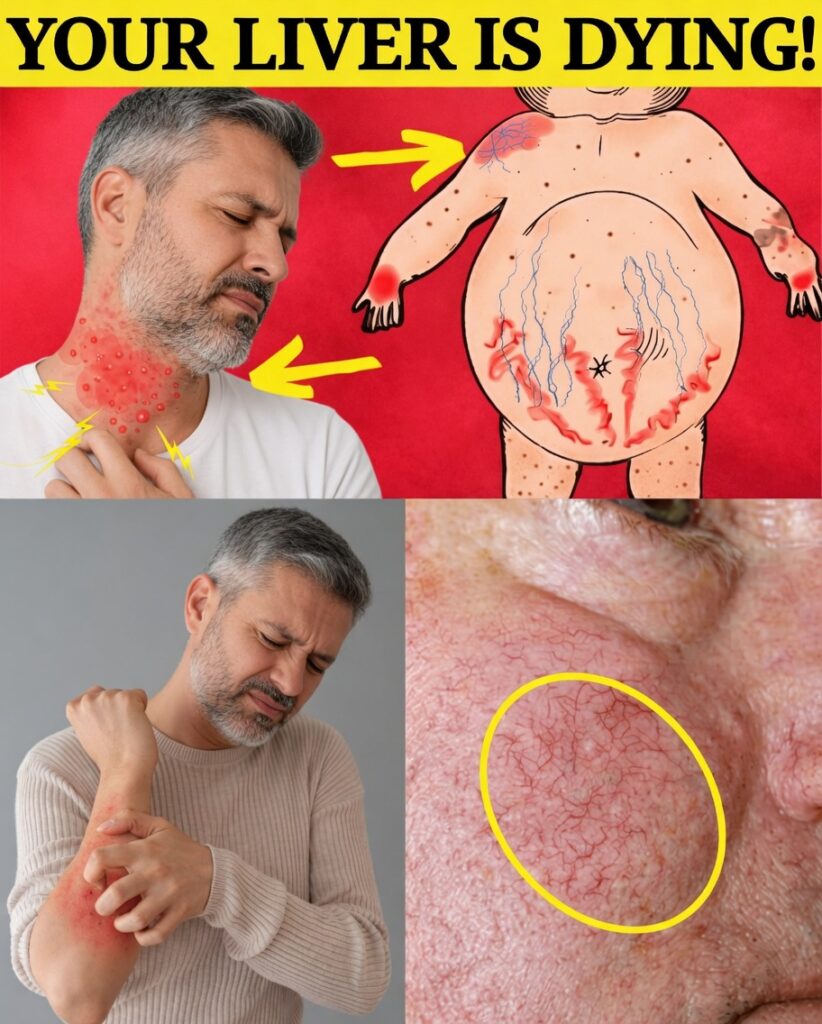
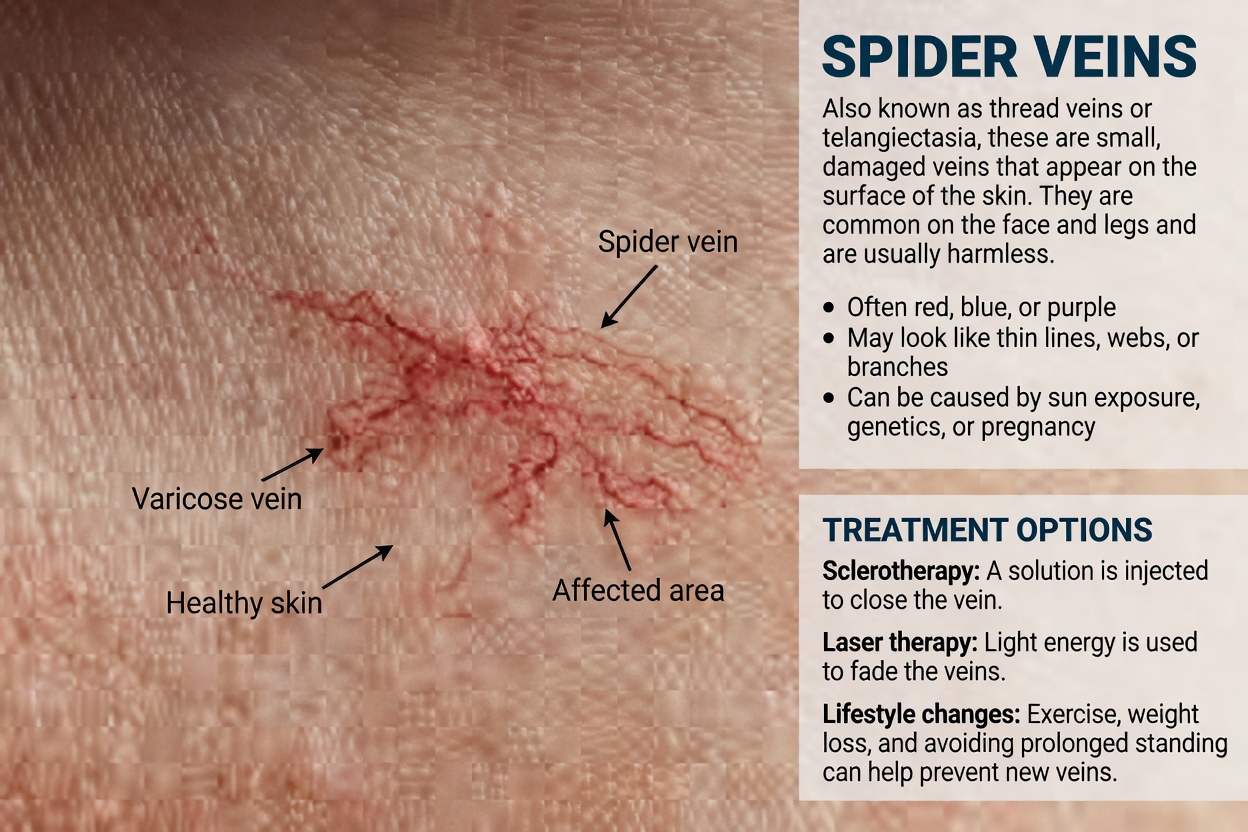
Spider-like blood vessels on the skin
Tiny red lines or web-shaped clusters (often called “spider veins”) can appear on the chest, face, or upper body due to liver-related changes in blood flow and hormones. -
Red or flushed palms
A reddish discoloration on the palms, especially at the base of the thumb and little finger, can sometimes be linked to liver dysfunction. -
Persistent abdominal bloating
Ongoing swelling or fullness in the abdomen—especially if it’s not explained by diet or digestion—may be a sign of fluid imbalance in more advanced liver disease. -
Noticeable veins on the abdomen
Enlarged or prominent veins on the belly can signal increased pressure in the blood vessels around the liver. -
Unexplained itching
Generalized itchiness without a clear rash or allergy may be related to changes in bile flow and liver processing. -
Discomfort under the right rib cage or between the shoulder blades
A dull ache or pressure in the upper right abdomen (where the liver sits) or referred pain into the back or shoulder area can occur when the liver becomes enlarged. -
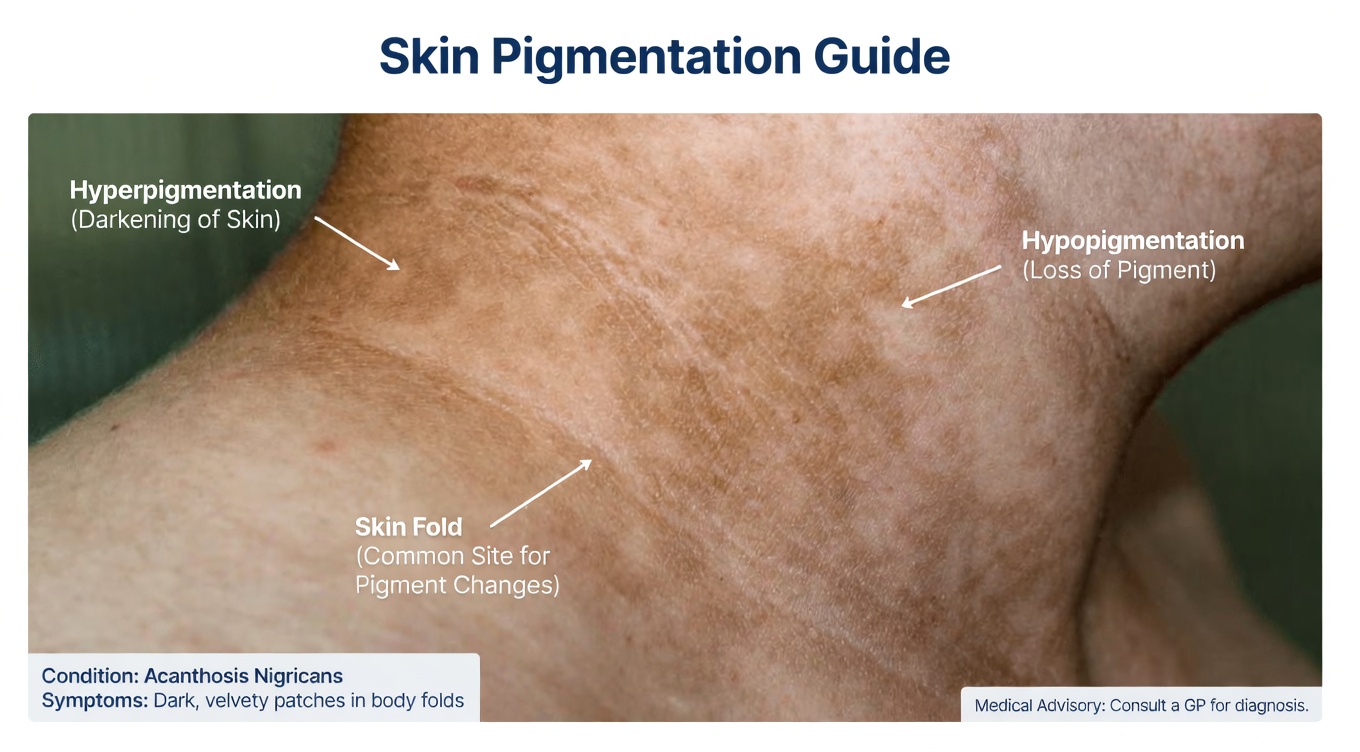
Dark, velvety skin patches
Areas of darker, thickened skin—commonly on the neck, armpits, or groin (acanthosis nigricans)—are often associated with insulin resistance, a key driver of nonalcoholic fatty liver disease. -
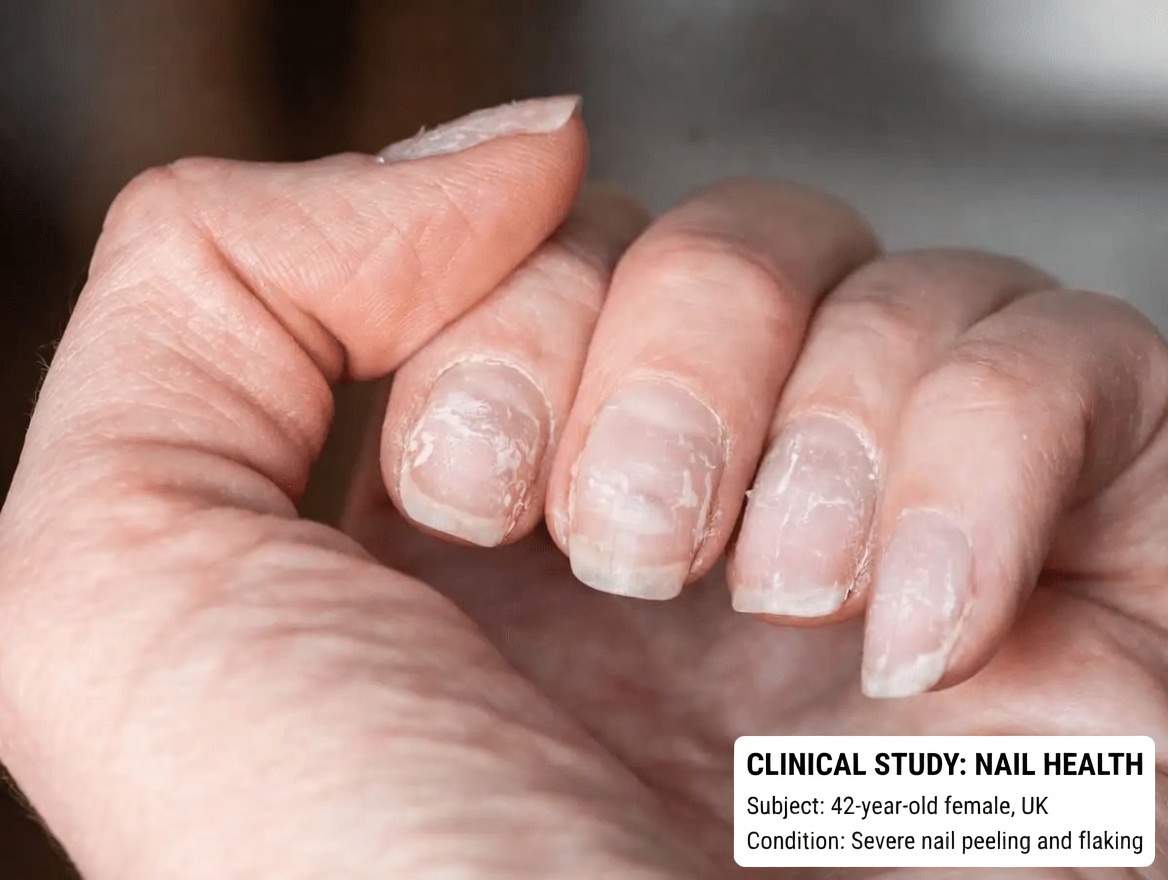
Changes in the nails
Brittle nails, ridges, or other alterations can sometimes reflect poor nutrient processing and absorption when the liver is not functioning optimally.
If several of these symptoms feel familiar, especially alongside risk factors like obesity, type 2 diabetes, or high cholesterol, it’s important to bring them up at your next medical appointment.
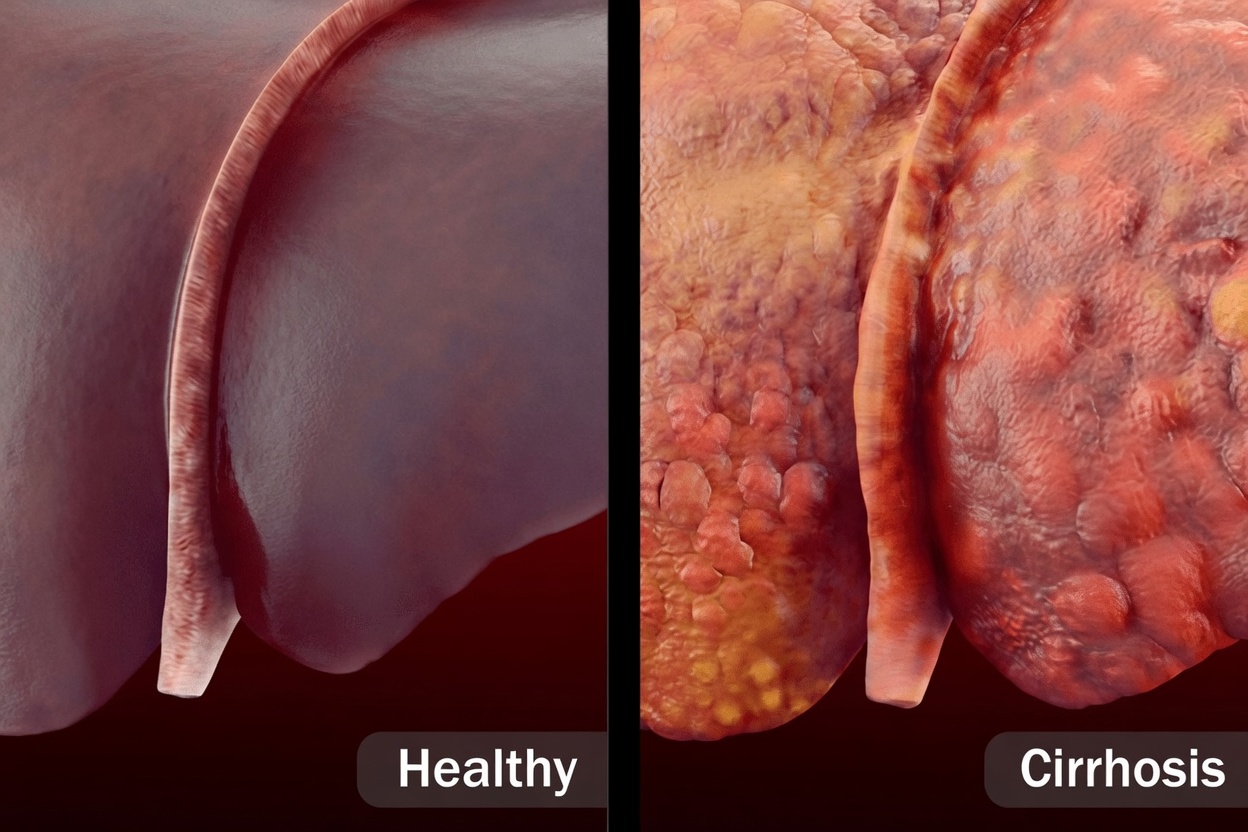
How Widespread Is Fatty Liver Disease?
Recent research suggests that tens of millions of adults in the U.S. are affected by fatty liver disease, many without a formal diagnosis. The condition has surged in step with:
- Rising rates of obesity and metabolic syndrome
- Increased intake of sugary drinks and processed foods
- Declining levels of daily physical activity
In many populations, fatty liver disease is now one of the leading causes of chronic liver problems. Because it develops gradually, everyday food choices and lifestyle patterns can quietly contribute to liver fat buildup over years.
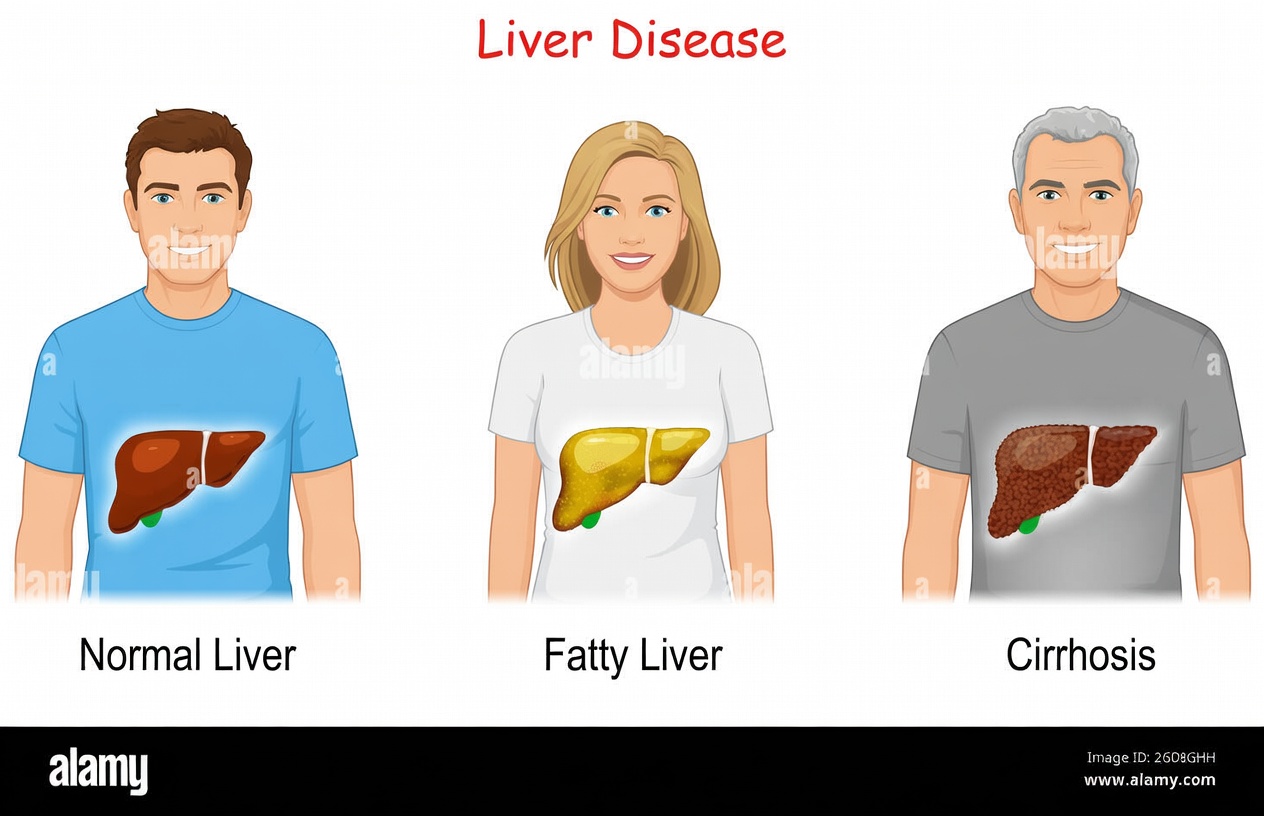
Real-Life Experiences With Managing Fatty Liver Disease
People who learn about their fatty liver disease and make targeted lifestyle adjustments often report meaningful improvements.
-
Case example 1: A woman in her 40s noticed steady fatigue and mild discomfort under her ribs. After being diagnosed with fatty liver disease, she shifted her focus to whole foods—such as vegetables, high-quality protein, and healthy fats—and added regular walking to her routine. Over time, she reported better energy and improved follow-up lab results.
-
Case example 2: Another individual experiencing abdominal bloating and poor sleep found relief after working with a healthcare provider to reduce added sugars and alcohol, increase physical activity, and support weight management. These changes were associated with fewer symptoms and better liver markers.
While each person’s experience is unique, these stories highlight that targeted lifestyle changes can support liver health and complement medical care.
5 Practical Strategies to Support Your Liver
Evidence suggests that certain lifestyle patterns can help improve liver fat levels and overall liver function in people with fatty liver disease. Consider discussing these approaches with your doctor:
-
Adopt a balanced, liver-friendly eating pattern
Emphasize whole, minimally processed foods:- Plenty of vegetables and high-fiber foods
- Lean proteins (such as fish, poultry, legumes)
- Healthy fats (such as olive oil, nuts, seeds, and avocado)
Reducing sugary drinks, refined carbohydrates, and fried foods can be particularly helpful.
-
Prioritize hydration
Drinking enough water throughout the day supports digestion, circulation, and overall metabolic health, which all influence liver function. -
Move your body regularly
Aim for a mix of aerobic activity (like brisk walking or cycling) and strength training. Physical activity helps improve insulin sensitivity and can reduce fat accumulation in the liver. -
Limit or avoid alcohol
Even moderate alcohol intake can add extra stress to a liver already dealing with excess fat. Many people with fatty liver disease benefit from cutting back significantly—or eliminating alcohol altogether—under medical guidance. -
Include supportive foods and spices
Certain foods are being studied for their potential liver-supportive properties, including:- Leafy green vegetables
- Berries
- Coffee (in moderation, if tolerated and approved by your doctor)
- Herbs and spices like turmeric (curcumin), garlic, and ginger
Always consult your healthcare practitioner before making major dietary or lifestyle changes, especially if you have existing health conditions or take medications.
Consistency is key: small, sustainable adjustments, maintained over time, usually offer more benefit than short-term, extreme changes.
The Impact of Small Daily Habits
When it comes to fatty liver disease, everyday habits can add up—either in support of liver health or against it. Many people find it helpful to:
- Track energy levels, sleep quality, and mood
- Note what they eat and how active they are
- Record one small positive step each day (such as an extra glass of water or a 10-minute walk)
This kind of simple journaling can increase awareness, highlight patterns, and make it easier to stay motivated as you work toward better liver health.
Frequently Asked Questions About Fatty Liver Disease
What causes fatty liver disease?
Fatty liver disease typically develops due to a combination of factors, including:
- Insulin resistance and metabolic syndrome
- Excess body weight, especially around the midsection
- Diets high in sugars, refined carbohydrates, and processed foods
- Low levels of physical activity
- Certain medications and medical conditions
Both alcoholic and nonalcoholic forms of fatty liver disease exist, and your healthcare provider can help determine which type you may have.
How is fatty liver disease usually detected?
Fatty liver disease often shows up during routine testing or when a person is evaluated for other health concerns. Common tools include:
- Blood tests to check liver enzymes and other markers
- Ultrasound to visualize fat in the liver
- Other imaging tests, such as CT scans, MRI, or specialized elastography, when needed
In some cases, a liver biopsy may be recommended to assess the severity of liver damage.
Can lifestyle changes really help fatty liver disease?
Yes. Research indicates that lifestyle changes can significantly improve fatty liver disease in many people. Beneficial strategies may include:
- Weight loss (even a modest amount can help)
- Healthier eating patterns, like a Mediterranean-style diet
- Regular physical activity
- Reducing alcohol intake
- Managing related conditions such as diabetes, high blood pressure, and high cholesterol
Always work with a healthcare professional to create a safe and personalized plan.
Taking the Next Step for Your Liver Health
Understanding fatty liver disease—and the subtle ways it can show up—is a powerful first step. By noticing potential signs, assessing your risk factors, and making small daily changes, you can have more informed conversations with your healthcare team and take an active role in protecting your liver.
You don’t need to overhaul your life overnight. Start with one manageable change: an extra serving of vegetables, a 15-minute walk, or a decision to skip sugary drinks today. Over time, these small choices can compound into meaningful support for your liver.
P.S. Try keeping a simple daily note of your energy level and one positive action you took for your liver—such as moving more, drinking water instead of soda, or cooking a homemade meal. Seeing your progress on paper can be encouraging as you work to manage or prevent fatty liver disease.