
CAR-T Cell Therapy for Autoimmune Disease: What Current Research Means for Patients
Living with an autoimmune disorder can feel exhausting. Flare-ups may appear without warning, daily symptoms can interfere with normal routines, and the ongoing need for medication often adds emotional stress on top of physical discomfort. For many people, that constant uncertainty affects energy, independence, and overall well-being.
New advances in medical science, however, are creating reasons for hope. One of the most talked-about developments is CAR-T cell therapy, a personalized treatment strategy that researchers are now exploring for autoimmune diseases. Although this approach is still under investigation, early findings suggest it may offer a new path toward longer-lasting disease control.
What Is CAR-T Cell Therapy?
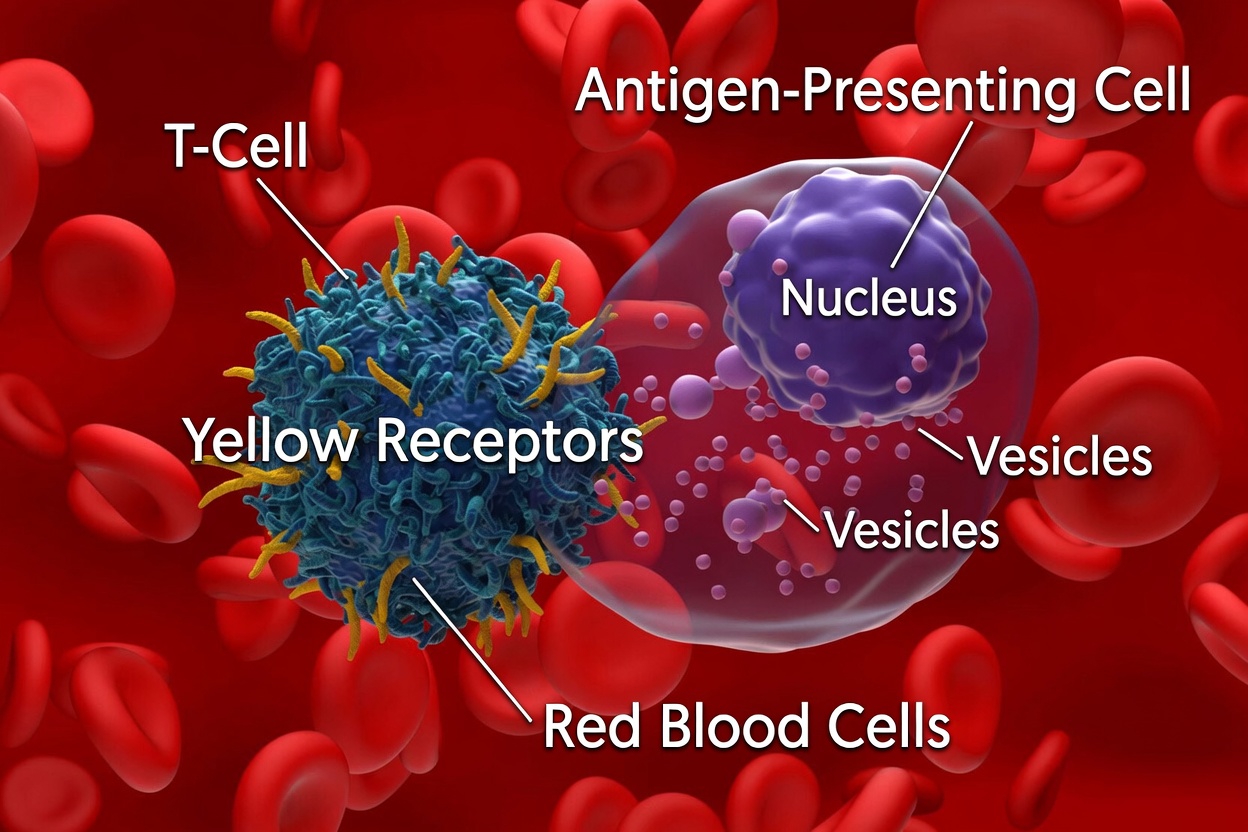
CAR-T cell therapy is a customized cell-based treatment made from a patient’s own immune cells. Doctors first collect immune cells called T cells, then alter them in a specialized laboratory so they can better identify and attack a specific target. After that, the modified cells are infused back into the patient.
This technique was first developed and tested in cancer care. Now, scientists are studying whether the same principle can help people with autoimmune diseases, where the immune system mistakenly attacks healthy tissues.
The goal is different from traditional broad immune suppression. Instead of calming the immune system in a general way, CAR-T research aims to target the deeper source of immune dysfunction more precisely.
How CAR-T Therapy Is Being Used in Autoimmune Research
In many autoimmune conditions, B cells play a major role because they can produce harmful autoantibodies. Researchers are designing CAR-T cells to recognize and eliminate these overactive B cells.
Once returned to the body, the engineered T cells can multiply and begin removing the problem cells. The hope is that this creates an opportunity for the immune system to rebuild in a healthier way.
Early reports, including studies published in journals such as Nature Medicine, describe this process as a kind of immune reset. In some early-phase trials, participants experienced meaningful reductions in disease activity that lasted well beyond the treatment itself.
A major reason this research is drawing attention is that CAR-T is being studied as a single treatment procedure, followed by observation and follow-up, rather than as a medication taken every day.
Autoimmune Conditions Being Studied With CAR-T
Researchers are currently evaluating CAR-T cell therapy in several autoimmune diseases, especially those in which B cells appear to be central to the disease process. Most of this work is happening in Phase 1 and Phase 2 clinical trials, where safety and early effectiveness are closely monitored.
Conditions under investigation include:
- Systemic lupus erythematosus (SLE), including lupus with kidney involvement
- Systemic sclerosis, also called scleroderma
- Idiopathic inflammatory myopathies (IIM), including forms of myositis
- Myasthenia gravis and some related neuromuscular disorders
- Certain difficult-to-treat cases of rheumatoid arthritis
These studies mainly focus on patients whose disease has not responded well to standard therapies.
What Recent Clinical Trials Have Found
Some of the most promising updates have come from basket trials and disease-specific studies reported in 2025 and early 2026. One example is the CASTLE trial, which tested a CD19-targeted CAR-T therapy in people with treatment-resistant lupus, systemic sclerosis, and myositis.
According to reported results, many trial participants met key response goals by 24 weeks. During the observation period, a number of them also did not require continued immunosuppressive medication.
Other research programs, including those using mRNA-based CAR-T platforms or dual-targeting strategies, have shown a similar pattern:
- Depletion of harmful B cells
- Gradual return of more immature or naïve immune cells
- Improvement in disease measures in some patients
Participants in these studies often reported better day-to-day functioning. Even so, results are not identical for everyone, and longer follow-up is still needed.
One of the most striking findings from several independent research groups is the possibility of longer symptom-free periods. In some reported cases, autoantibodies became undetectable and disease severity scores dropped substantially after treatment.
Step-by-Step: What the CAR-T Process Usually Looks Like
For anyone wondering how CAR-T treatment is handled in a research setting, the pathway is usually structured and closely supervised.
1. Screening and Eligibility
Doctors review:
- Medical history
- Current disease activity
- Prior treatments
- Bloodwork and other test results
This helps determine whether a person qualifies for a specific trial.
2. Cell Collection
T cells are collected from the patient through:
- A standard blood draw, or
- Apheresis, a process that separates and collects certain blood components
3. Laboratory Engineering
The collected cells are sent to a specialized lab, where they are modified to express receptors that can identify the targeted immune cells. This stage typically takes several weeks.
4. Pre-Treatment Preparation
Before infusion, patients may receive a short course of lymphodepleting chemotherapy. This step helps make room in the immune system for the engineered cells to expand.
5. Infusion and Early Monitoring
The CAR-T cells are given back through an IV infusion. Afterward, patients are monitored carefully, often in the hospital or in a specialized treatment center, especially during the first days or weeks.
6. Long-Term Follow-Up
Ongoing follow-up may continue for months or years and usually includes:
- Blood tests
- Immune system monitoring
- Symptom tracking
- Assessment of disease activity
This careful structure helps researchers collect dependable data while prioritizing patient safety.
Questions to Ask Your Doctor About CAR-T Research
Even though CAR-T for autoimmune disease is still investigational, it may be helpful to start a conversation with your specialist now. If you are interested in future options, consider asking questions such as:
- Are any cell therapy clinical trials currently enrolling near me?
- Would my diagnosis and treatment history fit the criteria for any ongoing study?
- What kind of testing and monitoring would be required?
- What risks should I understand before considering a trial?
- Are there lifestyle habits I should focus on while waiting for new treatment options?
Many large hospitals and academic centers maintain access to trial registries. Looking together at resources like ClinicalTrials.gov can help identify the latest studies.
Daily Habits That Still Matter While Research Continues
While emerging treatments are exciting, basic self-care remains an important part of autoimmune disease management. Supportive lifestyle habits can improve resilience and may help you feel better day to day.
Consider focusing on:
- Regular sleep routines to support immune regulation
- Gentle physical activity such as walking, stretching, or yoga
- Anti-inflammatory foods like leafy greens, berries, and fatty fish
- Stress-management practices including mindfulness or deep breathing
- Preventive care, including recommended vaccinations and routine checkups
These steps are not a replacement for medical treatment, but they can complement the care plan you already have.
Safety Considerations and What Studies Have Reported So Far
Every new treatment comes with important risks and limitations, and CAR-T is no exception. So far, autoimmune-focused studies have generally reported less severe side effects than those often seen when CAR-T is used in cancer treatment.
Among the more commonly described side effects are:
- Low-grade cytokine release syndrome
- Temporary changes in immune cell levels
- Mild, short-term flu-like symptoms
- Brief changes in blood counts
Most reported reactions have been manageable with standard supportive care.
Researchers have also observed some newer effects, including temporary localized inflammation in affected organs. These events have usually been short-lived, but they reinforce the importance of expert monitoring.
A key message from the 2025–2026 data is that success depends heavily on:
- Careful patient selection
- Treatment at specialized centers
- Close follow-up by experienced teams
A Promising Future for Autoimmune Care
CAR-T cell therapy is still in the research stage for autoimmune disease, but the direction of the data is encouraging. Across multiple early trials, scientists are seeing signs that targeted immune resetting may be possible in ways that were difficult to imagine just a few years ago.
For people living with severe or treatment-resistant autoimmune conditions, this research offers something meaningful: real scientific momentum. It is not yet a standard treatment, but it is becoming an important area to watch.
Staying informed, asking questions, and working closely with your care team can help you make decisions that support your long-term health goals.
Frequently Asked Questions
Is CAR-T cell therapy available for autoimmune diseases outside clinical trials?
No. At this time, CAR-T therapy for autoimmune conditions remains investigational and is available only through approved clinical studies. Speak with your specialist if you want to explore trial eligibility.
What side effects have been reported in autoimmune CAR-T studies?
Most side effects reported so far have been short-term and manageable. They may include mild flu-like symptoms, temporary blood count changes, and low-grade cytokine release syndrome. Clinical trials use strict safety monitoring throughout the process.
Why are B cells targeted in these studies?
B cells are involved in many autoimmune diseases because they can produce autoantibodies that attack healthy tissues. By removing harmful B cells, researchers hope to reduce disease activity and allow the immune system to rebuild in a healthier way.
Is CAR-T considered a one-time treatment?
In current autoimmune research, CAR-T is being studied as a single infusion-based procedure followed by ongoing monitoring. However, long-term durability is still being evaluated, so more data are needed.
Which autoimmune diseases are showing the most promising early results?
The strongest early signals have been reported in systemic lupus erythematosus, systemic sclerosis, myositis, and myasthenia gravis, particularly in patients whose disease has been difficult to control with standard treatment.



