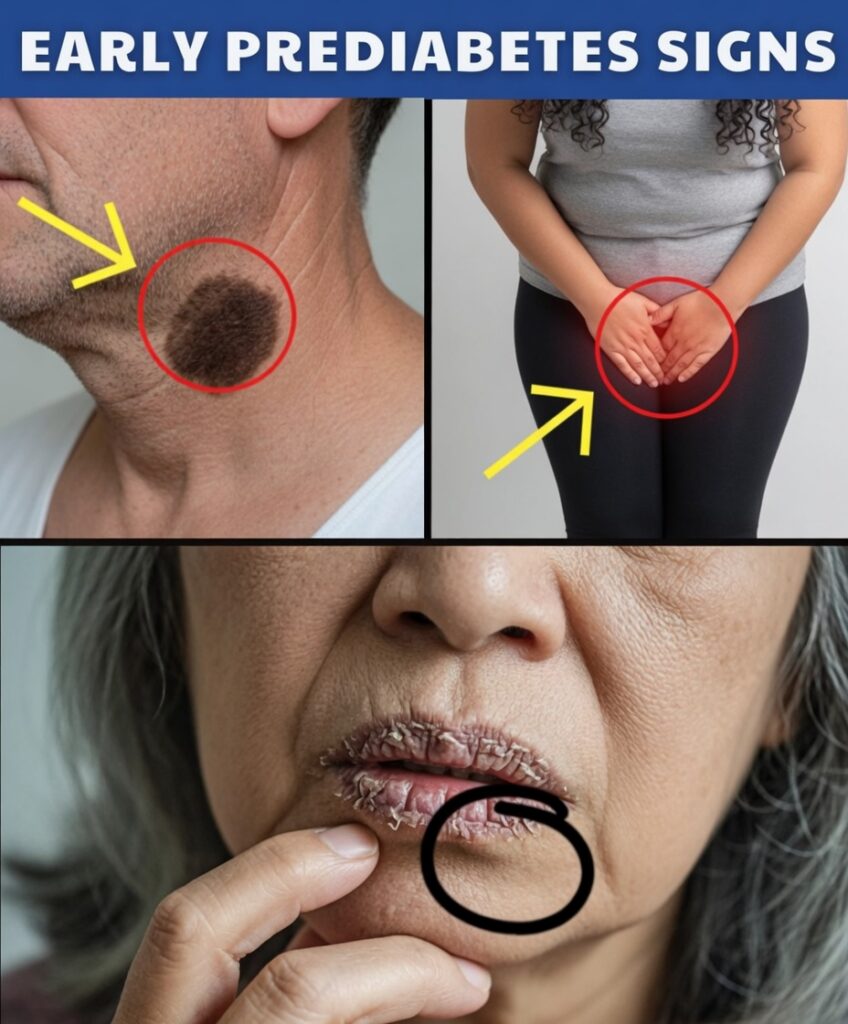
Prediabetes Can Start Silently—But Your Body Often Hints at It
Prediabetes affects millions of people and frequently develops with little to no obvious symptoms in the beginning. It describes a stage where blood sugar is above the healthy range but not yet high enough to qualify as type 2 diabetes. Even so, it meaningfully increases the likelihood of long-term health problems, including heart disease and stroke.
Because the early changes can resemble everyday life—stress, poor sleep, or “just aging”—many people ignore them, giving blood sugar issues time to progress.
Your body, however, may be signaling that something is off. Learning to recognize early prediabetes warning signs can help you take action sooner, potentially preventing type 2 diabetes and protecting your long-term health.
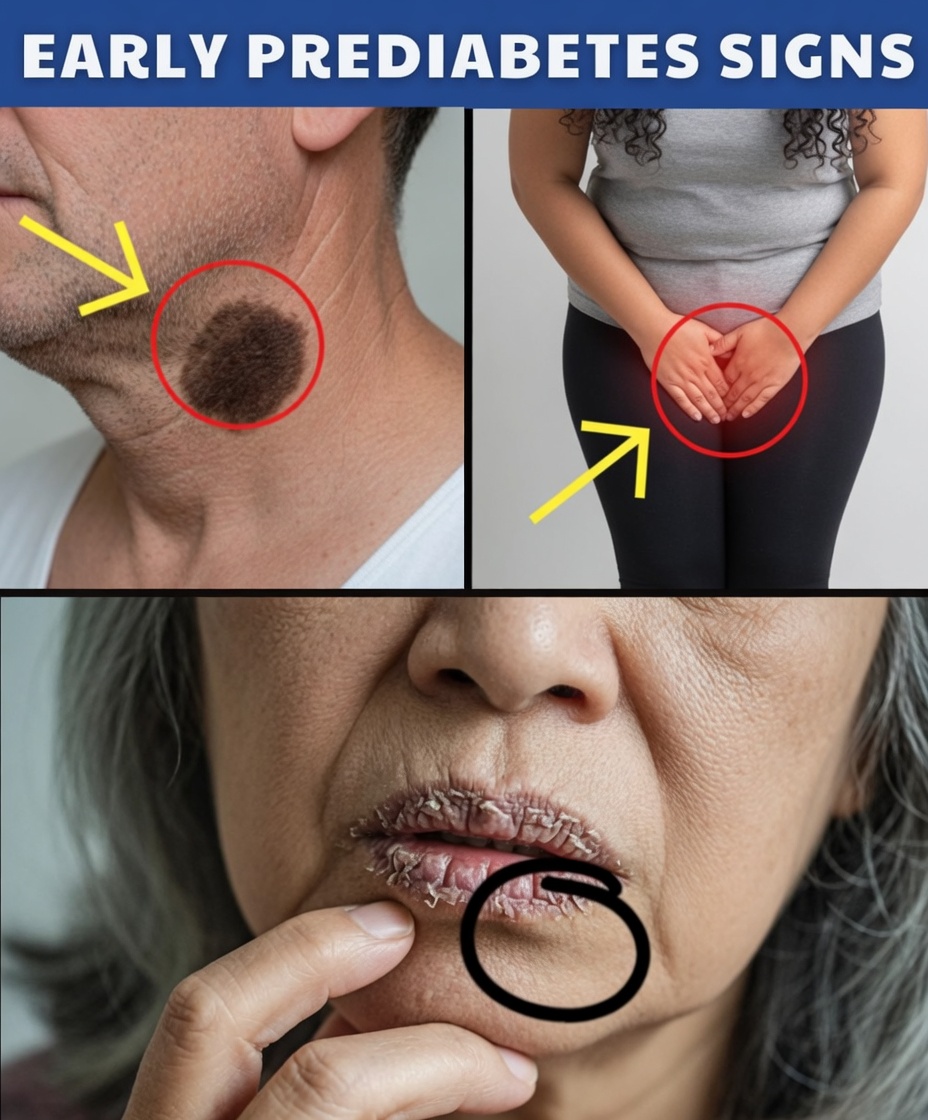
9 Early Prediabetes Warning Signs Many People Overlook
1. Ongoing Fatigue That Doesn’t Improve With Rest
If you feel consistently worn out despite sleeping enough, it may be more than a busy schedule. With insulin resistance, glucose has a harder time entering your cells to be used as energy, which can leave you feeling sluggish and mentally “foggy.” This lingering exhaustion can affect work performance, mood, and daily routines, and it often appears before blood sugar rises dramatically.

2. Thirst That Feels Hard to Quench
Drinking more water than usual yet still feeling thirsty can be an early clue. When blood sugar runs high, fluid is pulled from tissues, contributing to dehydration and a persistent dry mouth. This isn’t just annoying—it can disrupt focus and leave you feeling uncomfortable throughout the day.
3. Needing to Urinate More Often (Especially Overnight)
Frequent urination—particularly waking multiple times at night—can be an early prediabetes warning sign. As the body tries to remove excess glucose, the kidneys work harder, producing more urine and filling the bladder faster. Beyond inconvenience, this can interrupt sleep and lead to daytime fatigue.

4. Blurry or Changing Vision
If your vision becomes temporarily blurry or seems to fluctuate, blood sugar may be playing a role. Higher glucose levels can shift fluid balance in the eye’s lens, affecting how clearly you see. Many people assume it’s time for new glasses, but vision changes that come and go can be a meaningful signal—often improving once glucose is better controlled.
5. Cuts or Bruises That Heal More Slowly
Small wounds that take noticeably longer to heal may indicate that circulation and immune response aren’t working optimally. Elevated glucose can interfere with the body’s repair processes, turning minor injuries into lingering problems and increasing the risk of infection.

6. Tingling, “Pins and Needles,” or Numbness in Hands and Feet
Subtle nerve irritation can begin early. Over time, higher blood sugar may damage small nerves, sometimes first felt as tingling or numbness in the feet or hands. Even mild symptoms deserve attention, because nerve changes can worsen if insulin resistance progresses.
7. Unexplained Weight Gain or Weight Loss
Weight shifts that don’t match your eating habits or activity level can be a clue. Insulin resistance can affect metabolism in ways that lead to gradual weight gain (often around the midsection). In some cases, people may lose weight if the body struggles to use glucose effectively. Either change can feel discouraging and difficult to control without understanding the root cause.
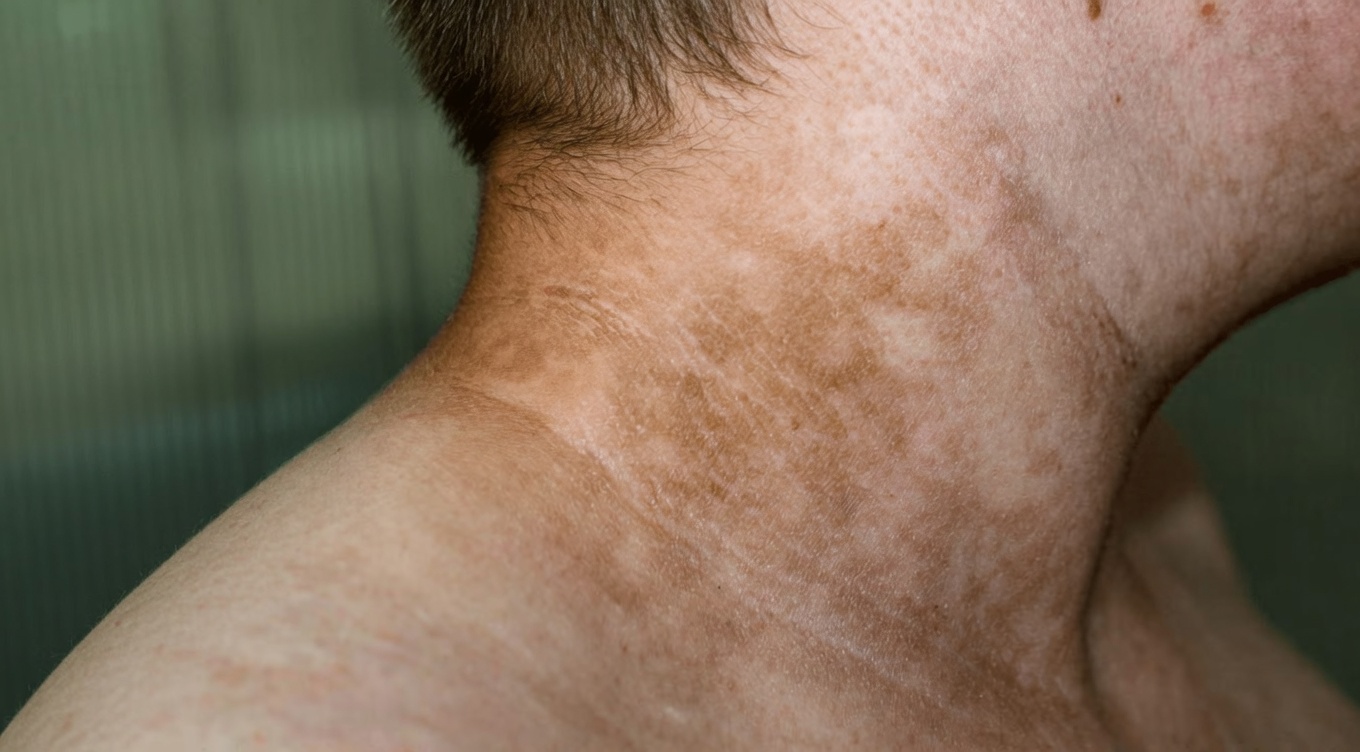
8. Dark, Velvety Skin Patches (Acanthosis Nigricans)
Thickened, darker patches of skin—commonly on the neck, armpits, or groin—are strongly associated with insulin resistance. This visible change can affect confidence, but it’s also one of the clearest outward signs that blood sugar regulation may be impaired.
9. Feeling Hungry Soon After Eating
If you’re hungry again shortly after a meal, your cells may not be accessing glucose efficiently. When the body can’t use glucose well, the brain may continue to signal hunger even when you’ve eaten enough. This can drive overeating and lead to energy “crashes,” making healthy routines harder to maintain.
What to Do If These Early Prediabetes Warning Signs Sound Familiar
Noticing a few symptoms doesn’t mean you should panic—think of it as a prompt to act. Many people can improve insulin sensitivity and reduce risk through consistent lifestyle adjustments. Consider these practical next steps:
-
Get tested
- Ask your clinician about A1C, fasting glucose, or an oral glucose tolerance test.
-
Build balanced meals
- Emphasize fiber-rich vegetables, lean protein, and whole grains to support steadier blood sugar.
-
Move every day
- Aim for about 30 minutes of moderate activity (such as brisk walking) on most days.
-
Protect sleep and manage stress
- Both sleep quality and chronic stress can influence insulin function and appetite regulation.
-
Track your progress
- Monitor symptoms, weight, and habits—small, consistent changes often add up over time.
Conclusion
These nine early prediabetes warning signs are often subtle, but they can be your body’s way of asking for attention. Recognizing them sooner gives you the opportunity to make informed changes and discuss testing and options with a healthcare professional. The steps you take today can meaningfully improve your health trajectory tomorrow.
Frequently Asked Questions
What is prediabetes, exactly?
Prediabetes is a condition where blood sugar is higher than normal but not high enough for a diabetes diagnosis. For many people, it can be improved—and sometimes reversed—through lifestyle changes.
How is prediabetes diagnosed?
Prediabetes is diagnosed using blood tests, such as:
- A1C (an A1C of 5.7% to 6.4% suggests prediabetes)
- Fasting plasma glucose
- Oral glucose tolerance test
Who is at higher risk for prediabetes?
Common risk factors include:
- Having overweight or obesity
- Age 45 and older
- A family history of type 2 diabetes
- Low physical activity (sedentary lifestyle)
- A history of gestational diabetes