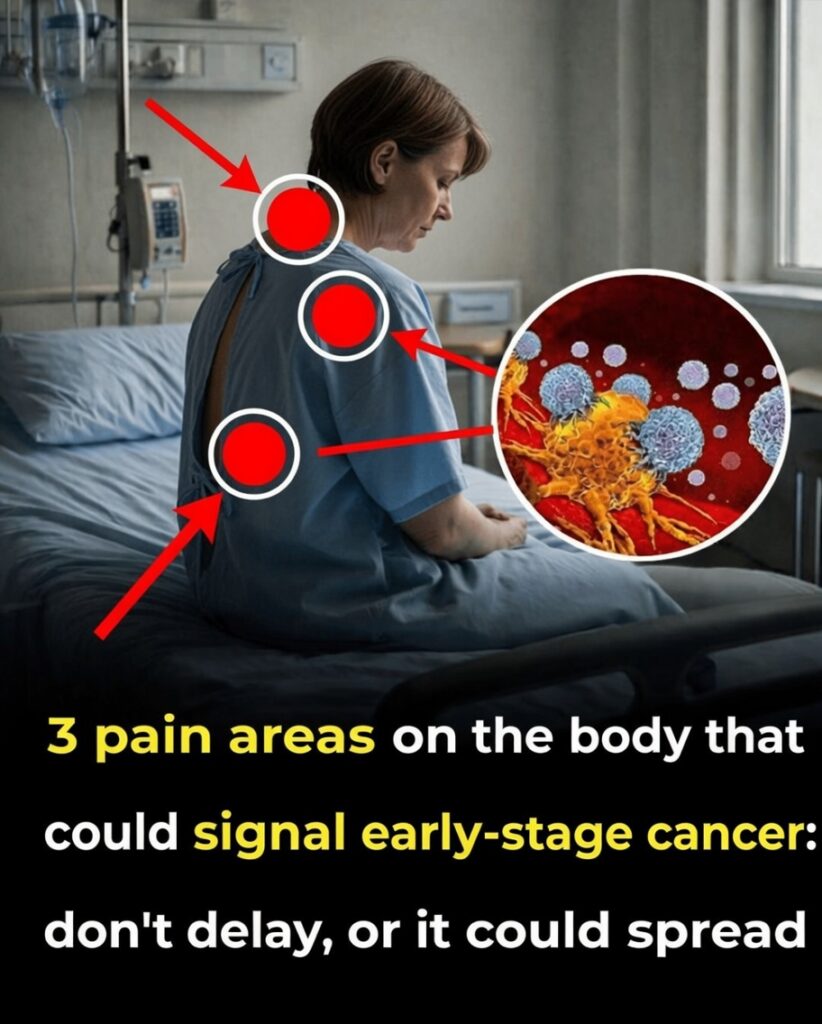
Many of us dismiss aches in certain pain areas as normal aging, poor posture, or a tough workout. However, when discomfort doesn’t go away, keeps returning, or begins to interfere with daily life, it may deserve more attention. In some cases, persistent, unexplained pain can be one of the early cancer warning signs—not a diagnosis, but a reason to check in with a healthcare professional.
Ongoing soreness can drain your energy, limit your routines, and create a constant undercurrent of worry about what’s happening inside your body. That stress can affect sleep, mood, and relationships. Learning which pain patterns to notice helps you better interpret your body’s signals and decide when it’s time to talk to a doctor. At the end, you’ll find a simple daily habit that can help you stay ahead of potential health issues.
Understanding Pain Areas as Potential Signals
Pain that may relate to early cancer warning signs often begins subtly. Because it doesn’t always arrive with dramatic symptoms, it can be easy to ignore—especially if life is busy or you assume it will pass. Yet major medical organizations, including the National Cancer Institute, emphasize that unusual, ongoing discomfort without a clear cause should be taken seriously.
Persistent pain can disrupt sleep and concentration, reduce physical activity, and leave you feeling isolated or frustrated. The good news is that knowing what to watch for puts you back in control. A key theme across many concerning pain patterns is persistence over weeks and a noticeable change from what’s normal for you.
1) Unexplained Back Pain
Back pain is extremely common, which is why it often surprises people when it becomes a potential red flag. Unexplained back pain—pain that persists even with rest and isn’t clearly tied to lifting, exercise, or an injury—can be one of the pain areas associated with early cancer warning signs.
Health information sources such as Healthline note that this type of pain may feel different from a typical strain and can sometimes worsen at night. When pain interrupts sleep, it often triggers a cycle of fatigue, irritability, and anxiety that makes everyday responsibilities feel heavier than they should.
In some cases, discomfort in the lower back may be related to pressure on nerves or surrounding tissues. Over time, people may compensate by changing posture or limiting movement, which can reduce quality of life even further.
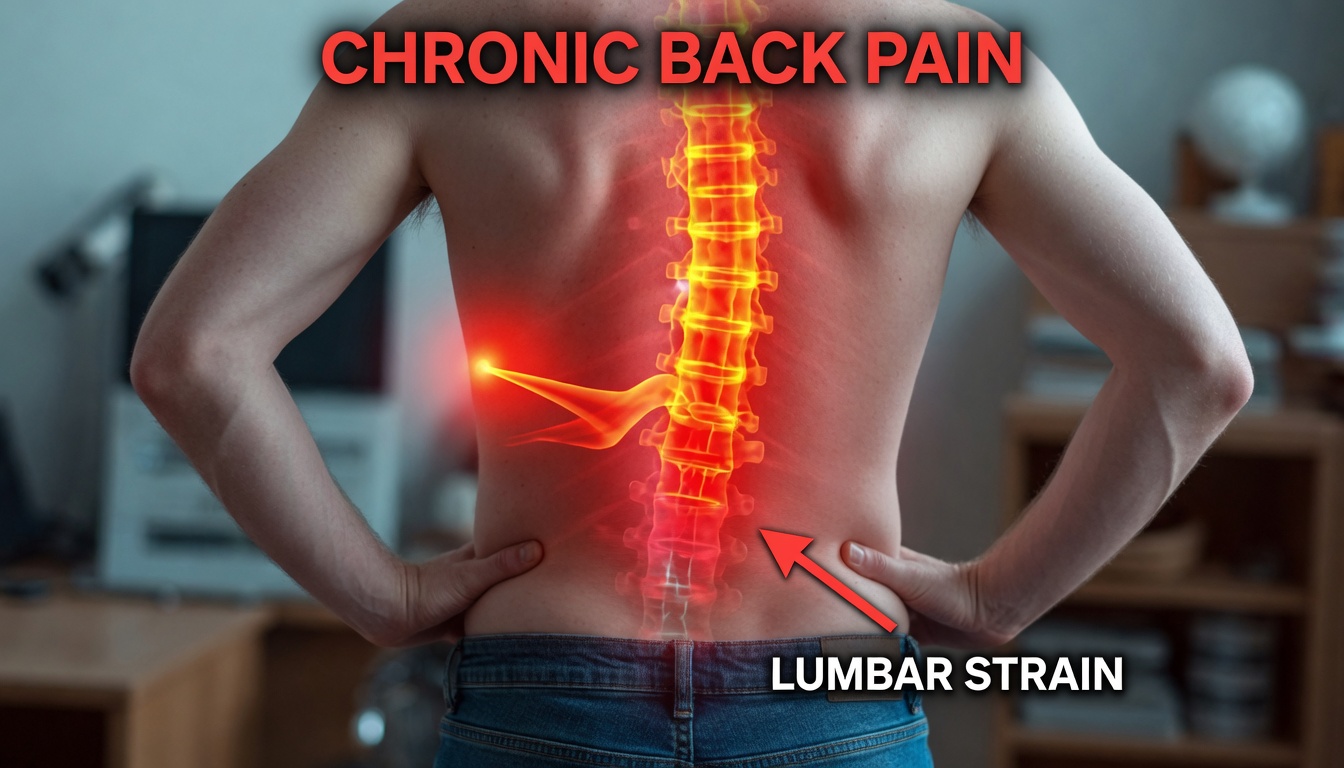
Why back pain stands out
Back pain becomes more concerning when it is:
- New or unusual for you
- Persistent for weeks
- Not improving with typical measures (rest, stretching, basic treatment)
- Disrupting sleep or worsening at night
The American Cancer Society also highlights that back pain paired with neurological or bowel/bladder changes should be assessed promptly.
Associated symptoms to note
Pay attention if back pain is accompanied by:
- Night pain that is stronger when lying down or wakes you repeatedly
- Unexplained weight loss along with persistent discomfort
- Tingling, numbness, or weakness in the limbs, making movement harder
These combinations don’t confirm anything on their own, but they are important context to share with a clinician.
2) Persistent Abdominal Pain
Another common yet important pain area involves the stomach and midsection. Persistent abdominal pain can make eating, working, and even sitting comfortably difficult. It may feel like bloating, pressure, cramping, or a dull ache that gradually intensifies. Guidance from sources such as WebMD notes that ongoing abdominal discomfort—especially without a clear digestive cause—should not be ignored.
When abdominal pain lingers, it can change appetite and energy levels. Some people begin avoiding meals or social situations because eating becomes stressful, which can affect relationships and mental well-being. For women, abdominal and pelvic sensations can overlap, making the experience more complicated and harder to describe.
Common patterns and variations
Abdominal pain that may warrant a medical conversation often has patterns such as:
- Bloating plus discomfort that persists
- Pain that worsens with meals or doesn’t follow typical food-related triggers
- A sensation of fullness or pressure that doesn’t resolve
Tracking patterns helps reduce uncertainty and makes medical visits more productive.
Related changes to watch
Consider seeking advice sooner if abdominal pain comes with:
- Ongoing bloating, affecting comfort and self-image
- Reduced appetite or difficulty eating, sometimes leading to unintended weight loss
- Nausea alongside pain, disrupting work and daily routines
Persistent abdominal symptoms can have many explanations, but the combination of duration and accompanying changes matters.
3) Headaches and Neurological Symptoms
Headaches can also be among the pain areas linked to early cancer warning signs, particularly when they are clearly different from your typical headaches. According to the Brain Tumour Charity, headaches that are worse in the morning or triggered by straining (such as coughing or bending) can be more concerning—especially if they increase over time.
These headaches may affect focus, mood, and productivity. Some people also experience visual changes such as flashes, blurred vision, or blind spots, which can add fear and confusion. When painkillers don’t help and the pattern keeps repeating, the emotional toll can be significant.

How potentially serious headaches differ
Headaches deserve closer attention when they are:
- New, intense, or progressively worsening
- More frequent over weeks
- Paired with neurological changes
- Triggered or aggravated by position changes (bending, coughing, straining)
If something feels distinctly “not normal” for you, that distinction is important.
Key accompanying signs
Seek medical guidance promptly if headaches come with:
- Vision disturbances (blind spots, double vision, sudden changes)
- Nausea or vomiting that follows the headache pattern
- A steady worsening trend over time, increasing distress and disruption
These signs are not meant to alarm you—they are meant to help you recognize when evaluation is appropriate.
Actionable Tips to Monitor Your Body
If you’re noticing persistent pain areas and wondering whether they could relate to early cancer warning signs, practical tracking can help you respond calmly and effectively.

What to record (and why it helps)
Use a notebook or phone note to track:
- Start date: when the pain first appeared
- Location: exact area(s), whether it spreads or stays fixed
- Intensity: a simple 1–10 rating
- Timing: morning vs. night, constant vs. intermittent
- Triggers: meals, movement, stress, coughing, position changes
- What helps: rest, heat, medication, stretching—and how much
- Other symptoms: fatigue, weight change, nausea, numbness, bowel/bladder changes
This information helps healthcare providers identify patterns and decide what steps (if any) are needed next.
When to talk to a doctor sooner
Consider making an appointment if pain:
- Lasts more than two to three weeks without improvement
- Wakes you at night or consistently worsens at night
- Is new and unexplained (not linked to injury or known condition)
- Comes with weight loss, persistent fatigue, neurological changes, or appetite changes
A Simple Habit That Helps You Stay Ahead
A straightforward daily routine can reduce uncertainty and make it easier to spot changes early: a 60-second body check-in.

Once a day—ideally at the same time—pause and ask:
- Where do I feel discomfort today?
- Is anything new, persistent, or worsening?
- Is this affecting sleep, appetite, movement, or mood?
If you notice a pattern developing over days or weeks, you’ll have clear notes and a calm, practical reason to seek medical advice. This habit doesn’t create fear—it creates clarity, so you can act early when something doesn’t feel right.