High Cholesterol: The Silent Risk You Might Be Missing
Many people move through their daily routines without realizing that high cholesterol may be quietly undermining their health. This condition is extremely common, yet it rarely causes obvious warning signs until more serious problems develop. As a result, things like tiredness, mild discomfort, or shortness of breath are often dismissed as “normal,” while plaque continues to build up inside the arteries and raises the risk of heart disease over time.
The good news: by understanding how high cholesterol works, learning the possible indirect clues, and building simple monitoring habits, you can protect yourself far more effectively. Stay with this article to the end—you’ll discover an unexpected everyday strategy backed by research that may help improve your cholesterol levels.

What Is High Cholesterol and Why Does It Matter?
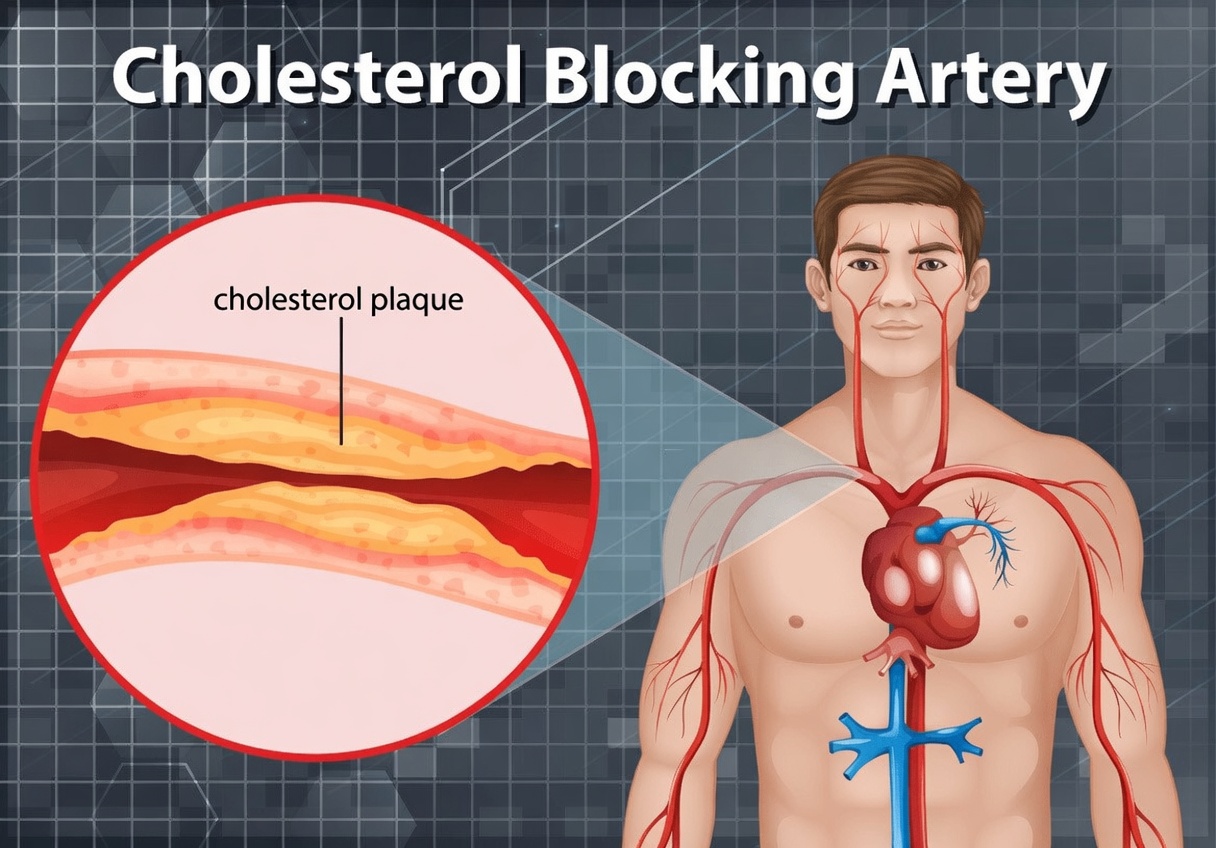
Cholesterol is a waxy, fat-like substance found in your blood. Your body needs it in reasonable amounts to build cell membranes and produce hormones. Problems begin when cholesterol levels—especially “bad” LDL cholesterol—become too high.
Excess LDL can:
- Stick to artery walls
- Form fatty deposits called plaque
- Narrow or stiffen blood vessels (atherosclerosis)
- Restrict blood flow to vital organs
This process usually develops slowly and silently. You can feel perfectly fine while plaque is quietly accumulating, which is why high cholesterol is often called a “silent” risk factor.
Large health organizations such as the Mayo Clinic report that millions of people worldwide live with elevated cholesterol levels, often without knowing it, simply because regular screening is overlooked. Understanding this foundation is essential before you can spot potential warning signs or take action.
Myths About High Cholesterol Symptoms
There are several common misunderstandings about how high cholesterol shows up in the body.
Myth 1: High cholesterol always causes noticeable symptoms.
Many people believe it leads to clear problems like constant headaches, stomach issues, or dramatic fatigue. In reality, as highlighted by sources such as the Cleveland Clinic, high cholesterol itself usually doesn’t produce direct, specific symptoms. Any discomfort you might feel typically comes from complications—like heart disease or circulation problems—that arise after years of buildup.
Myth 2: Only older people need to think about cholesterol.
It’s widely assumed that high cholesterol is solely a concern for seniors. However, the British Heart Foundation and other research groups emphasize that lifestyle factors—diet, lack of exercise, smoking, and obesity—can affect cholesterol levels at almost any age. Even younger adults can have unhealthy levels, especially if there is a family history.
Understanding what high cholesterol does not do can be just as important as knowing what it can cause. Accurate information gives you the power to act early, rather than waiting for dramatic warning signs that may never come.

Indirect Signs That May Be Linked to High Cholesterol Complications
While elevated cholesterol typically doesn’t cause symptoms on its own, the damage it creates can show up in subtle ways. These signs are not proof of high cholesterol, but they may be connected to its long-term effects on your arteries and circulation.
Possible indirect clues include:
-
Chest discomfort during activity
Reduced blood flow to the heart muscle—often due to narrowed coronary arteries—may cause chest tightness, pressure, or pain when you exert yourself. -
Shortness of breath with light effort
Feeling winded after climbing a few stairs or doing mild tasks can sometimes indicate that your heart is working harder because of restricted blood flow, according to the National Heart, Lung, and Blood Institute (NHLBI). -
Leg pain or cramping while walking
Aching, cramps, or fatigue in your calves, thighs, or hips when you walk (that improves with rest) may signal peripheral artery disease, where arteries in the legs are narrowed by plaque. -
Numbness or coldness in hands and feet
Poor circulation can lead to tingling, numb sensations, or unusually cold extremities, especially in one limb. -
Swelling in legs, ankles, or feet
Fluid buildup in the lower body might be related to circulation or heart function and can sometimes be associated with long-standing vascular issues. -
Unexplained cold sweats
Sudden cold, clammy sweating with no obvious cause can be a concern, particularly if it occurs alongside chest discomfort or shortness of breath. -
Severe headaches or dizziness
Although they have many possible causes, these symptoms can occasionally be linked to reduced blood supply to the brain. -
General fatigue or heaviness
Ongoing tiredness or a sense of heaviness in the body might reflect overall cardiovascular strain, even if it’s easy to brush off as “just being tired.” -
Blurred vision or visual disturbances
Changes in vision can sometimes accompany vascular problems and signal that something is affecting circulation to the eyes or brain. -
Visible skin or eye changes in rare cases
In people with very high cholesterol—often due to genetic conditions—MedlinePlus notes that:- Yellowish, fatty bumps may appear on the skin (xanthomas).
- A grayish or white ring around the cornea (arcus senilis) can develop.
None of these signs alone confirm high cholesterol, but they are reasons to take your cardiovascular health seriously and speak with a healthcare professional.
How to Test Your Cholesterol: Step-by-Step
If you want clear answers about your cholesterol levels, a simple blood test is the only reliable method. This test is usually called a lipid panel or cholesterol profile.
Follow these steps:
-
Book an appointment with a healthcare provider
Let them know you’d like your cholesterol checked. They may ask you to fast (avoid eating and drinking anything except water) for 9–12 hours beforehand to get the most accurate measurements. -
Have your blood sample taken
A small amount of blood is drawn from a vein in your arm. The procedure is quick and usually causes only mild discomfort. -
Review your lipid panel results
Your report will typically include:- Total cholesterol – Aim for under 200 mg/dL
- LDL (“bad”) cholesterol – Ideally below 100 mg/dL
- HDL (“good”) cholesterol – Preferably 60 mg/dL or higher
These target ranges are based on guidance from organizations such as the American Heart Association, though your personal goals may differ if you have other health conditions.
-
Discuss next steps if your levels are high
Your provider might recommend:- Dietary and lifestyle changes
- More frequent monitoring
- Additional tests (for example, to assess heart disease risk)
- Medication, if lifestyle measures aren’t enough or your risk is high
Regular testing gives you a clear picture of what’s happening inside your arteries long before symptoms appear.
Lifestyle Habits That Support Healthy Cholesterol Levels
You don’t need a dramatic overhaul to start improving your cholesterol profile. Small, consistent changes to your daily routine can add up to meaningful results.
1. Focus on a Heart-Healthy Diet
What you eat plays a major role in your LDL and HDL levels.
-
Choose more fiber-rich foods
Soluble fiber helps reduce the absorption of LDL cholesterol in the gut. Good sources include:- Oats and barley
- Beans and lentils
- Apples, pears, and other fruits
-
Emphasize healthy fats
Replace saturated fats with unsaturated fats to help protect your heart:- Avocados
- Olive oil and other vegetable oils
- Nuts and seeds (almonds, walnuts, chia seeds, flaxseeds)
-
Limit saturated and trans fats
Cut back on:- Fatty cuts of red meat
- Processed and fried foods
- Commercial baked goods made with hydrogenated oils
-
Consider foods with plant sterols
Fortified spreads and certain products contain plant sterols, which can help block the absorption of cholesterol in the intestines. -
Choose whole grains over refined grains
Options like brown rice, whole-wheat bread, and quinoa support overall heart health and help with weight management. -
Load up on fruits and vegetables
Colorful produce such as berries, citrus fruits, and leafy greens provides antioxidants that support cardiovascular health.
2. Move Your Body Regularly
Physical activity helps raise HDL (the “good” cholesterol) and can lower triglycerides and LDL.
Helpful exercise options include:
-
Aerobic exercise
Aim for about 150 minutes per week of moderate-intensity activities such as:- Brisk walking
- Cycling
- Swimming
-
Strength training
Include resistance exercises at least two days per week to build muscle, improve metabolism, and support weight control. -
Mind–body activities
Practices like yoga or tai chi can help manage stress, which indirectly benefits heart health and cholesterol. -
Daily walking
Even short walks throughout the day make a difference. Consistency is more important than perfection.
3. Address Other Key Lifestyle Factors
-
Maintain a healthy weight
The NHLBI notes that even modest weight loss can improve cholesterol and reduce cardiovascular risk. -
Quit smoking
Smoking damages blood vessels and worsens the impact of high cholesterol. Stopping can quickly improve HDL levels and overall heart health. -
Manage stress and sleep
Chronic stress and poor sleep habits can drive unhealthy behaviors and affect heart health over time. -
Track your habits
Using a simple app or journal to log your meals, exercise, and test results can help you stay accountable and notice progress.
Foods to Include in Your Daily Routine (Quick List)
- Soluble fiber sources: apples, beans, lentils, barley, oats
- Healthy fats: almonds, walnuts, pistachios, seeds, olive oil, avocado
- Plant sterols: fortified margarines and spreads, some fortified yogurts and juices
- Whole grains: brown rice, oatmeal, whole-wheat bread, quinoa
- Fruits and vegetables: berries, citrus fruits, leafy greens, cruciferous vegetables (broccoli, cauliflower, Brussels sprouts)
Exercises That Can Help Lower Cholesterol
- Aerobic activities: brisk walking, jogging, cycling, swimming
- Strength training: bodyweight exercises, resistance bands, weight machines, free weights
- Flexibility and balance work: yoga, pilates, tai chi
- Everyday movement: taking the stairs, walking meetings, active breaks during the day
Start with one or two changes you feel confident you can keep, then build from there.
Good vs. Bad Cholesterol: A Quick Comparison
Understanding the difference between HDL and LDL is crucial for managing your risk.
| Aspect | Good Cholesterol (HDL) | Bad Cholesterol (LDL) |
|---|---|---|
| Primary role | Carries excess cholesterol away from the blood and arteries to the liver for removal | Delivers cholesterol from the liver to cells and can deposit it in artery walls |
| Health impact | Helps protect against heart disease and stroke | Contributes to plaque buildup and artery narrowing |
| Ideal blood level | Above 60 mg/dL | Below 100 mg/dL (lower is generally better) |
| Common sources | Regular exercise, healthy fats (nuts, seeds, olive oil, fatty fish) | Diets high in saturated fat, trans fats, processed foods |
| Management strategy | Increase with physical activity and heart-healthy fats | Reduce by limiting saturated fats and eating more fiber-rich, plant-based foods |
Balancing these two types of cholesterol—raising HDL while keeping LDL in check—is a central goal of long-term heart health.
Genetics, Risk Factors, and Who Should Be Extra Cautious
Not everyone faces the same level of risk when it comes to high cholesterol. Some factors are within your control; others are not.
-
Family history
Conditions such as familial hypercholesterolemia—an inherited disorder mentioned by the British Heart Foundation—can cause very high LDL levels from a young age, even with a healthy lifestyle. -
Age and sex
Cholesterol levels tend to rise as people get older. After menopause, women often see an increase in LDL cholesterol. -
Ethnicity
Certain ethnic groups may have a higher likelihood of high cholesterol or related heart disease due to genetic and environmental factors. -
Lifestyle habits
A diet high in saturated and trans fats, physical inactivity, smoking, and excessive alcohol intake can all contribute to elevated cholesterol.
Knowing your personal risk factors helps you decide how aggressively to monitor and manage your cholesterol levels.
When to Seek Professional Medical Advice
You should contact a healthcare professional if:
- You experience persistent or recurring chest discomfort, pressure, or pain—especially during activity.
- You notice unexplained shortness of breath, dizziness, or fainting.
- You have leg pain or cramps when walking that improve with rest.
- You feel extreme, ongoing fatigue or see swelling in your legs, ankles, or feet.
- You observe unusual changes such as yellowish skin bumps or rings around your eyes.
In addition, routine cholesterol checks are recommended even if you feel well. Many experts, including the Mayo Clinic, suggest that adults aged 20 and older have their cholesterol tested every 4–6 years, or more often if they have additional risk factors like diabetes, high blood pressure, smoking, or a strong family history of heart disease.
Early detection means you can make adjustments before serious complications develop.
Key Takeaways—and One Simple Daily Snack Strategy
To recap:
- High cholesterol rarely causes obvious symptoms on its own.
- Indirect signs—such as chest discomfort with exertion, leg pain when walking, shortness of breath, numbness, or unusual fatigue—may be tied to complications from long-term plaque buildup.
- A cholesterol blood test (lipid panel) is the only reliable way to know your levels.
- Diet, exercise, weight management, and not smoking are powerful tools for improving your cholesterol and protecting your heart.
- Genetics and other risk factors influence how closely you should monitor your levels and how aggressively you should act.
And here’s the promised everyday tip:
Research from sources like the Cleveland Clinic suggests that adding a small handful of pistachios to your daily diet may help support healthier cholesterol management. Thanks to their mix of healthy fats, fiber, and plant compounds, pistachios can contribute to lowering LDL and supporting overall heart health when they replace less healthy snacks.
Combined with regular checkups and a heart-conscious lifestyle, this simple habit can be one more practical step toward keeping your cholesterol in a healthier range.