Recognizing Subcortical Vascular Dementia Before It Advances
Watching someone you love gradually slow down can be deeply painful—especially when those changes look like “normal aging” and everyone feels unsure whether to worry or wait. Subtle shifts in movement, mood, or thinking often slip by unnoticed, postponing important conversations and delaying support.
Understanding the early signs of subcortical vascular dementia can help you act sooner, reduce confusion, and ease some of the emotional weight on the whole family. Keep reading—sign #5 is one of the most frequently misunderstood symptoms.

Why Subcortical Vascular Dementia Often Goes Unnoticed
Subcortical vascular dementia typically begins quietly. At first, it can resemble everyday slowing down with age, leaving families wondering if they are overreacting or imagining things.
This form of dementia affects the deeper structures of the brain rather than the outer layers, so the earliest changes are not always about memory. Instead, loved ones may just seem “off,” more withdrawn, or physically slower, without being able to explain what feels wrong.
Large medical centers, including the Mayo Clinic, note that early subcortical vascular dementia symptoms tend to involve thinking speed, coordination, and movement. For families, it can be heartbreaking to watch a parent or partner struggle with routine tasks, not knowing what is causing the change. Recognizing the pattern earlier unlocks better planning and management.

What “Subcortical” Means—and Why the Symptoms Feel Different
In subcortical vascular dementia, tiny blood vessels deep in the brain become damaged. This disrupts communication between brain regions, especially in the white matter—the “wiring” that connects different areas. As a result, everything can start to feel slower, less coordinated, and harder to organize.
Unlike Alzheimer’s disease, which often starts with clear memory loss, subcortical vascular dementia usually affects planning, speed of thinking, and movement first. Families may notice:
- A growing risk of falls
- Trouble with multi-step tasks
- Withdrawal from activities that once brought joy
The National Institute on Aging explains that these changes stem from reduced blood flow to key white matter pathways. When personality shifts, daily abilities decline, or independence slips away without explanation, relationships can become strained. Knowing how these pieces fit together can help families “name” what they are seeing much earlier.
The 8 Early Signs (Most People Miss #5)
No single sign can confirm subcortical vascular dementia, but recognizing clusters of changes can prompt timely medical evaluation and more focused support. Symptoms usually appear gradually and add up over time, which is why they are so easy to dismiss at first.
Cleveland Clinic and other expert sources emphasize how these small changes accumulate. Many families later wish they had connected the dots sooner. Here are eight signs to watch for.
⏳ Sign #8: Slowed Thinking and Mental Processing That Does Not Bounce Back
One of the most common early symptoms is a persistent slowdown in thinking. Conversations may take longer, responses are delayed, and decision-making that used to be quick now feels effortful and tiring.
This is not the usual end-of-day fatigue. It is a deeper, ongoing change that can make social gatherings, phone calls, or problem-solving feel overwhelming. Research suggests that attention and thinking speed are affected before memory. For relatives, the silence or hesitation where there used to be quick wit can feel like a quiet loss—but understanding the cause can help you respond with more patience and support.
📅 Sign #7: Executive Function Problems (Planning, Organizing, Following Steps)
“Executive functions” are the brain’s management skills: planning, organizing, prioritizing, and carrying out multi-step tasks. In subcortical vascular dementia, these often erode early.
You might notice:
- Unpaid bills or repeated late payments
- Missed medications or confusion about schedules
- Difficulty preparing meals or following recipes
- Trouble completing tasks that involve several steps
NHS guidance highlights executive dysfunction as an important early marker. Loved ones may appear careless or “irresponsible,” but in reality, their brain is struggling to sequence tasks. Stepping in to help can feel uncomfortable or intrusive, yet identifying this pattern can shift the focus from blame to understanding.
🚶 Sign #6: Motor Slowing and a New, Shuffling Walk
Changes in movement and gait are another hallmark of subcortical vascular dementia. Walking may become:
- Slower and more hesitant
- Shuffling, with short steps
- Unsteady, especially when turning or starting to walk
This altered gait increases the risk of falls and can make family members constantly worried about accidents. Over time, fear of falling may lead a person to limit their activity, fueling isolation and physical decline.
Johns Hopkins Medicine connects these movement changes to damage in small blood vessels affecting brain regions that coordinate motor control. Simple strategies—like removing tripping hazards, using assistive devices, and encouraging safe movement—can lower risk while preserving dignity.

😔 Sign #5: Apathy That Looks Like Depression (Most Often Overlooked)
Sign #5 is one of the most commonly missed: apathy. A person may lose motivation, show little initiative, or seem emotionally “flat.” Hobbies, social visits, and interests that once mattered may simply disappear.
From the outside, this can look exactly like depression, and it often gets labeled that way. The difference is that in apathy:
- The person may not feel particularly sad
- They usually do not complain about feeling hopeless
- They seem indifferent rather than distressed
The Alzheimer’s Society in the UK notes that apathy in dementia is subtle and frequently misinterpreted. Families can feel hurt by the emotional distance, or assume their loved one is “not trying” or pulling away on purpose. Recognizing apathy as a brain-based symptom—not a character flaw—can ease blame on all sides and lead to more appropriate support.
👀 Sign #4: Short, Fragile Attention and Concentration
Subcortical vascular dementia often makes it hard to stay focused, especially in busy or noisy environments. You may notice that your loved one:
- Cannot follow a long story or TV show
- Loses track of conversations easily
- Becomes overwhelmed by background noise or multiple people talking
- Needs things repeated several times
Reviews in journals indexed on ScienceDirect highlight attention problems as a core feature of this condition. For families, the constant need to re-explain or simplify can be draining, and shared activities may feel less enjoyable. Creating calmer spaces and breaking information into smaller pieces can help maintain connection.
🗣️ Sign #3: Slower, Less Precise Speech (More Slurred or Monotone)
Because subcortical vascular dementia can affect the brain pathways that control movement, speech may also change. Common signs include:
- Slower speech pace
- Slight slurring of words
- Reduced variation in tone, sounding more monotone
- Difficulty getting words out smoothly
Dementia UK notes that speech and motor changes can appear relatively early in this type of dementia. When conversations become harder to follow, both sides can feel frustrated or sad. Misunderstandings, repeated questions, and the loss of lively back-and-forth can weigh heavily on relationships. Calm pacing, allowing extra time, and avoiding interruptions can help bridge some of these gaps.
🧩 Sign #2: Complex Thinking Declines While Simple Skills Remain
A classic pattern in subcortical vascular dementia is that simple, routine tasks stay fairly intact, while more complex thinking declines. For example, a person may:
- Manage basic self-care independently
- Still recognize family and recall major life facts
- Yet struggle with finances, travel, technology, or medical decisions
MedLink and other neurology sources describe this “complex versus simple” split as typical. To families, this can be confusing: “They seem fine sometimes, then suddenly can’t manage something basic.” Understanding that higher-level reasoning is more affected than everyday habits can guide you to offer targeted help—especially with decisions involving money, safety, or health.
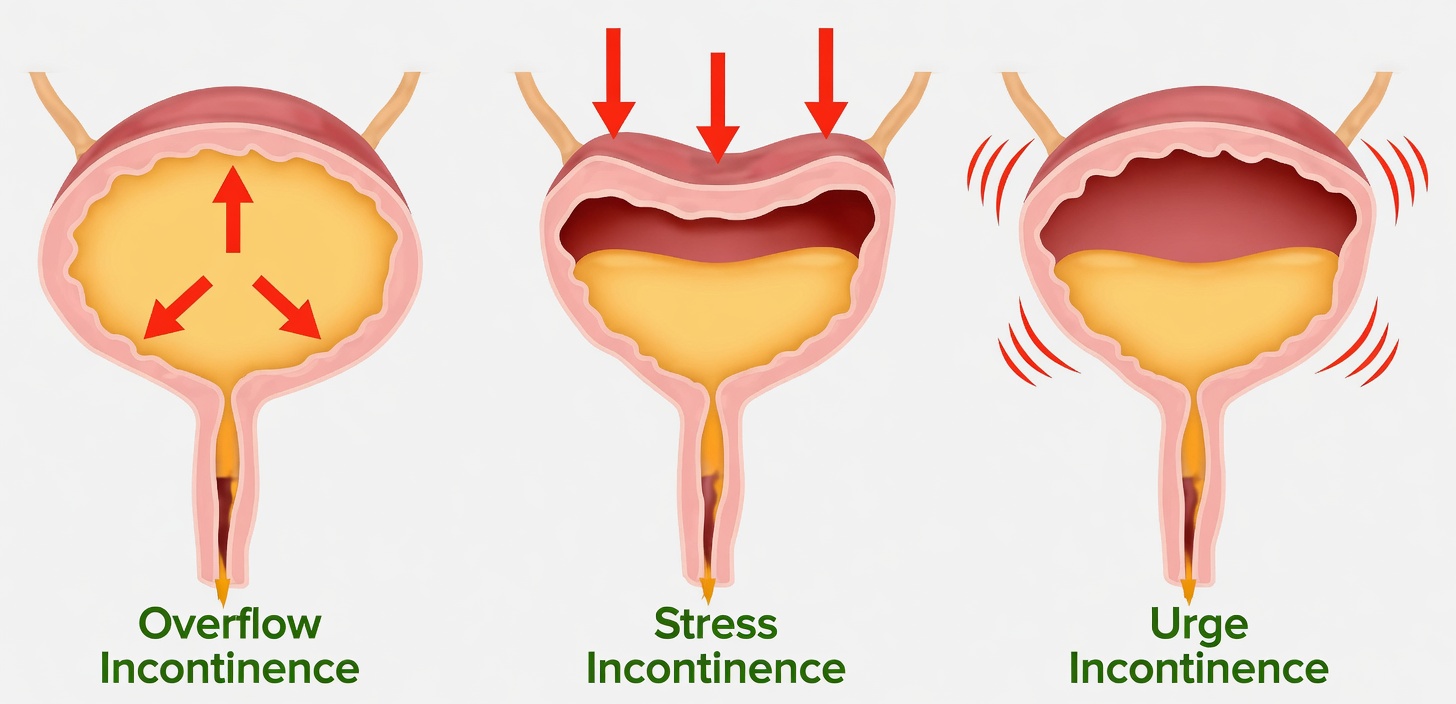
🚽 Sign #1: Urinary Urgency or Incontinence Without a Clear Bladder Cause
One of the more surprising signs is urinary urgency or incontinence without a straightforward urinary or prostate explanation. You may notice:
- A sudden need to rush to the bathroom
- More frequent accidents
- Difficulty holding urine even when the person seems otherwise well
Penn Medicine lists urinary problems as an important clue in subcortical vascular dementia, because brain pathways that control bladder function can be affected. This symptom is often embarrassing for the person involved and emotionally and practically demanding for caregivers. Recognizing it as a neurological issue rather than “just aging” can prompt proper medical workup and more compassionate care.
Quick Reference Guide: What to Watch and What to Record
To make these subcortical vascular dementia symptoms more actionable, use this summary table to track real-life examples. Writing things down can reduce the mental load when emotions are high and appointments are short.
| Sign | How It May Show Up Day-to-Day | Why Families Often Misinterpret It | What to Document Clearly |
|---|---|---|---|
| Slower processing | Long pauses, delayed answers, decisions take much longer | “He’s just tired or getting older” | When it started, specific situations, frequency |
| Executive difficulties | Bills unpaid, meds missed, meals or chores half-finished | “She’s distracted or disorganized lately” | Missed steps, safety concerns, real-world examples |
| Gait and movement change | Shuffling steps, short stride, unsteady turns | “It must be arthritis or joint pain” | Videos (if possible), fall history, near-misses |
| Apathy | No initiative, loss of interest, emotional “flatness” | “They’re depressed or not making an effort” | Differences between sadness vs lack of drive |
| Attention problems | Can’t follow conversations, easily overwhelmed by noise | “He’s not listening or doesn’t care” | How long they can focus, triggers, patterns |
| Motor speech changes | Slower, slightly slurred, or monotone speech | “She’s just quieter now” | Audio notes, when it happens, how it’s changed |
| Complex > simple split | Multi-step tasks fail while basic routines remain fine | “They’re only confused sometimes” | Which tasks are easy vs difficult in detail |
| Urinary urgency | Rushing to the toilet, accidents, frequent bathroom trips | “Normal aging or weak bladder” | Time of day, frequency, triggers, related events |
Having this information ready can make medical visits more productive and help clinicians see patterns that are easy to miss in a brief appointment.
What to Do Next: A Calm, Practical Action Plan
Suspecting subcortical vascular dementia can feel frightening and overwhelming, but a step-by-step approach can restore a sense of control.
-
Start a symptom log
Write down 5–7 clear examples of changes you’ve noticed, with dates, what happened, and how it differed from the person’s usual behavior. This moves concerns from “something seems wrong” to specific, concrete observations. -
Monitor vascular and lifestyle factors
Because this is a vascular condition, note blood pressure readings, sleep patterns, smoking status, and any history of stroke, heart disease, or diabetes. The National Institute on Aging stresses the role of these factors in progression. -
Seek a professional evaluation
- Contact a primary care doctor, neurologist, or memory clinic.
- Ask about cognitive screening and, if appropriate, more detailed neuropsychological testing.
- Bring your notes and table to the appointment to help guide the discussion.
Getting evaluated does not lock anyone into a label; it simply opens the door to better information, support, and planning.
Home Safety and Day-to-Day Support While You Wait
Even before you have a firm diagnosis, small changes at home can reduce risk and ease stress for both the person affected and their caregivers.
-
Reduce fall hazards
Remove loose rugs, secure cords, improve lighting in hallways and stairs, and place frequently used items within easy reach. -
Simplify routines
Use pill organizers, written checklists, or visual cues for daily tasks. Keeping routines predictable can lower frustration and support independence. -
Encourage gentle movement
Short, regular walks or light exercises—approved by a healthcare professional—can help maintain balance, circulation, and mood, and may reduce withdrawal.
These adjustments can provide immediate relief while you pursue further medical guidance.

Vascular Risk Controls That May Slow Progression (Even After 65)
While there is currently no cure for subcortical vascular dementia, managing vascular risk factors can sometimes help slow further damage, even in older adults.
Work with healthcare providers to focus on:
-
Blood pressure control
Keeping blood pressure within recommended ranges is one of the most important steps to protect small blood vessels in the brain. -
Diabetes management
Good blood sugar control can reduce additional vascular injury. This may involve medication adjustments, diet, and monitoring. -
Cholesterol and lipid management
Treating high cholesterol or other lipid problems can support healthier blood flow and reduce the risk of strokes and further vessel damage. -
Stopping smoking and limiting alcohol
Smoking and heavy drinking both increase vascular stress and brain damage risk. Support for quitting or cutting down can make a real difference. -
Regular physical activity
Even modest, doctor-approved exercise—like walking, stretching, or chair exercises—supports circulation, mood, and overall brain health. -
Heart and stroke follow-up
If there is a history of stroke, mini-strokes (TIAs), or heart disease, keeping follow-up appointments and taking prescribed medications consistently is crucial.
Managing these “vascular levers” will not reverse existing damage, but it may help slow further decline and improve quality of life. Combined with safety adjustments, emotional support, and informed medical care, early recognition gives families more time to adapt, plan, and stay connected.