Living with Proteinuria: Why Lifestyle Changes Matter
Persistent lower back discomfort, crushing tiredness, and the sudden sight of foamy urine can be deeply unsettling when proteinuria is part of your daily reality. These symptoms can make ordinary tasks feel heavier and raise urgent questions about your kidney health and future.
Proteinuria—excess protein in the urine—is often a sign that your kidneys need extra care, especially after age 40. A growing body of research suggests that practical lifestyle adjustments may help support kidney function alongside medical treatment.
What if small daily choices could help you feel more stable, more energetic, and more in control while living with proteinuria? Below are six evidence-informed strategies that may offer meaningful support.
Strategy 6: Shift to a Kidney-Friendly Diet
If swelling in your legs or feet caused by proteinuria leaves you feeling uncomfortable and self-conscious, your plate is an important place to start supporting your kidneys.
A diet high in salt and processed foods can place added strain on kidneys already challenged by proteinuria. Studies in nephrology have found that reducing sodium intake may:
- Ease fluid retention and swelling
- Lower blood pressure, which is closely tied to kidney health
- Reduce the overall workload on your kidneys
Focus on:
- Fresh fruits and vegetables rich in antioxidants
- Whole grains instead of refined grains
- Plant-based proteins such as beans, lentils, and tofu, which are often gentler on the kidneys than frequent red meat
You might hesitate to cut back on some favorite salty or packaged foods, but the potential benefits for reducing inflammation and slowing kidney stress related to proteinuria can make these adjustments worthwhile. Remember, your diet is a powerful, daily tool in your kidney-care plan.

Strategy 5: Keep Blood Pressure Under Control
For many people over 40, worries about high blood pressure worsening proteinuria can feel relentless. Elevated blood pressure directly affects kidney function and can accelerate kidney damage when proteinuria is present.
Research from large clinical trials suggests that maintaining blood pressure within a target range—often around below 130/80 mmHg, as advised by your healthcare provider—may:
- Slow the progression of kidney damage
- Reduce the amount of protein lost in urine
- Improve long-term kidney outcomes
Practical steps include:
- Regular home monitoring with a blood pressure cuff
- Tracking your readings to spot trends and share with your doctor
- Following medical advice on medications, diet, and activity
Taking charge of your numbers can provide a sense of control and reassurance as you manage proteinuria.
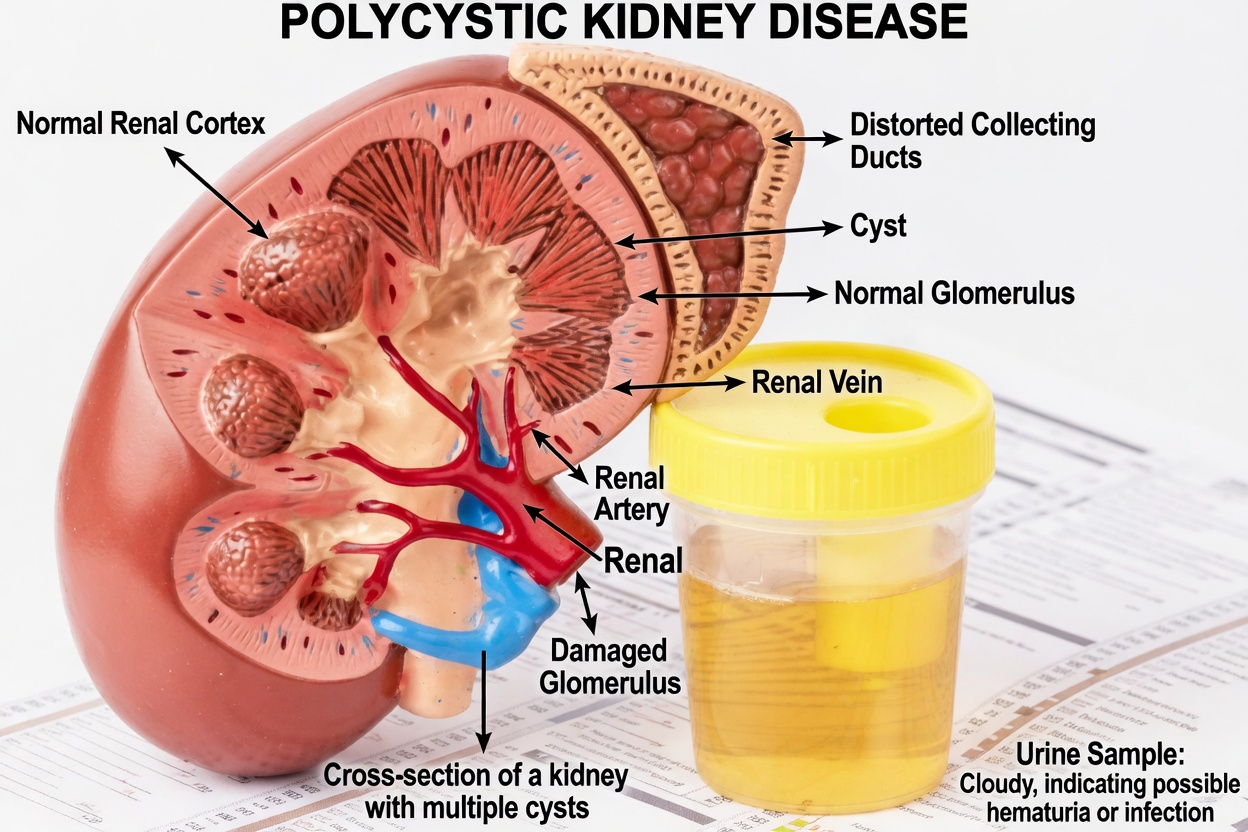
Strategy 4: Add Regular, Moderate Physical Activity
Fatigue linked to proteinuria can make the idea of exercise feel impossible—but gentle, consistent movement can actually help.
Moderate activities such as brisk walking, light cycling, or low-impact aerobics may:
- Improve circulation and blood flow to the kidneys
- Support healthy blood pressure levels
- Help reduce inflammation associated with proteinuria
- Boost energy and mood
Kidney research suggests aiming for about 150 minutes of moderate activity per week, spread across several days. You can start small:
- 5–10 minute walks, several times a day
- Gentle chair exercises if standing is difficult
- Light stretching to stay flexible
Picture a short, refreshing walk in the park that leaves you feeling a little more energized and clear-headed. Over time, these small efforts can support both kidney health and overall well-being.

Strategy 3: Stay Properly Hydrated
Concerns about thirst, dehydration, and changing urine appearance are very common when monitoring proteinuria. Hydration is a key piece of the puzzle.
Adequate fluid intake helps the kidneys:
- Flush out waste more effectively
- Maintain a healthier urine volume
- Potentially reduce the concentration of substances linked with proteinuria
Studies in kidney health suggest that drinking enough water may support kidney function, though your exact needs depend on your diagnosis and your doctor’s guidance.
A general starting point is about 8–10 glasses (around 2–2.5 liters) of fluid per day, unless your healthcare provider recommends otherwise. Each glass of water can feel like a small but meaningful step in your overall management plan for proteinuria.

Strategy 2: Include Omega-3 Rich Foods
Ongoing inflammation and discomfort are common themes for many people with proteinuria. Omega-3 fatty acids have been studied for their potential to support kidney health and help modulate inflammation.
Foods naturally rich in omega-3s include:
- Fatty fish: salmon, mackerel, sardines, trout
- Plant sources: flaxseeds, chia seeds, walnuts, hemp seeds
Some research, including meta-analyses, suggests that omega-3 intake may help reduce inflammatory markers and could be beneficial in conditions associated with proteinuria, though results are not identical in every study.
Integrating omega-3s into your diet might look like:
- Eating fatty fish 1–2 times per week
- Sprinkling ground flax or chia seeds on oatmeal or yogurt
- Adding walnuts to salads or snacks
These are relatively simple dietary shifts that may contribute to your kidney-care strategy, especially when combined with other healthy habits.

Strategy 1: Stop Smoking and Limit Alcohol
If you have a history of smoking, seeing proteinuria on your test results can intensify feelings of worry or regret. However, it is never too late to make changes that protect your kidneys.
Tobacco smoke:
- Damages blood vessels throughout the body, including in the kidneys
- Impairs circulation and oxygen delivery
- Can accelerate kidney damage and worsen proteinuria
Research aligned with public health guidelines indicates that quitting smoking may:
- Improve kidney blood flow
- Slow the decline in kidney function
- Support better overall cardiovascular health
Similarly, limiting alcohol to moderate levels—or avoiding it entirely if advised—helps avoid additional stress on both the liver and kidneys.
Imagine the long-term benefits of clearer lungs, improved circulation, and reduced toxin exposure while managing proteinuria. These changes can be among the most powerful steps you take for your kidneys.
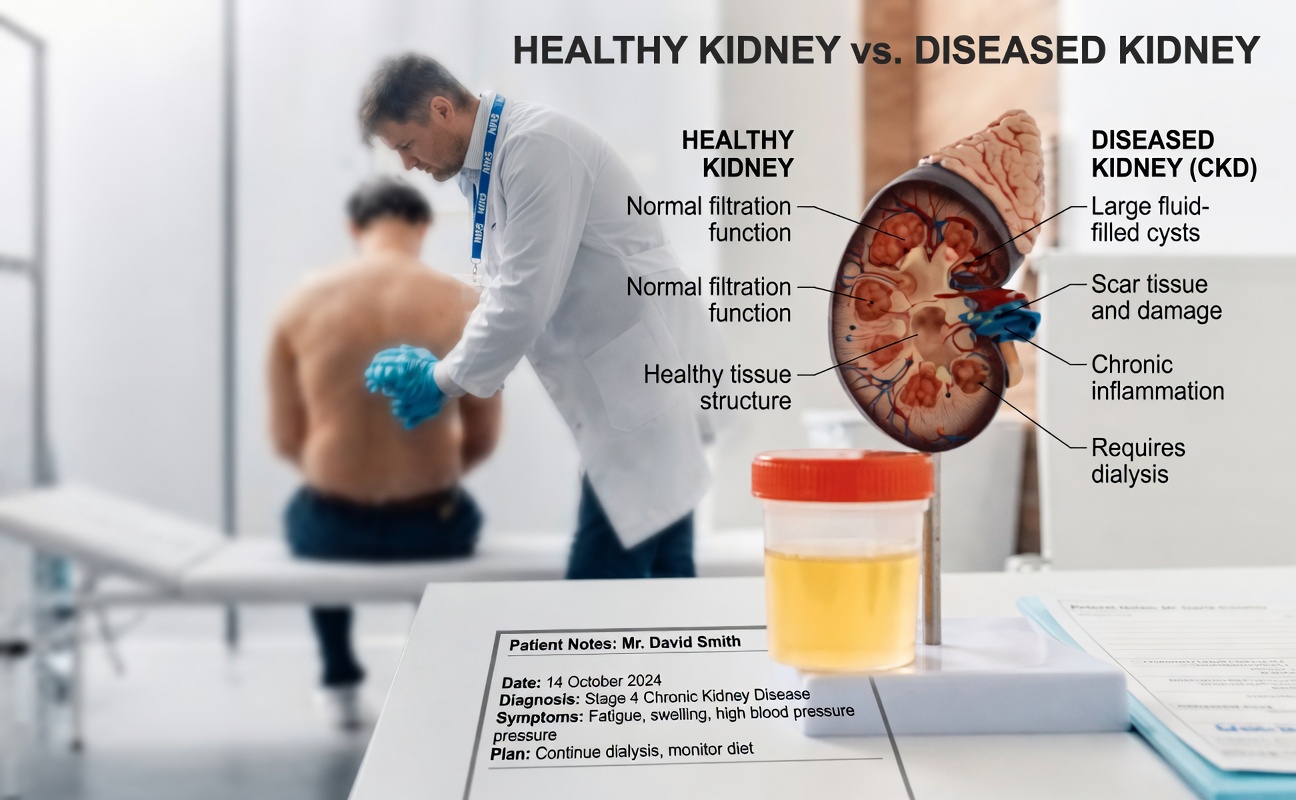
How These Strategies Work Together for Proteinuria
No single habit acts in isolation. Combining diet, exercise, hydration, and other lifestyle changes often provides stronger support than any one strategy alone.
Research from cohort studies suggests that people who adopt multiple healthy behaviors tend to have:
- Better blood pressure control
- Improved metabolic health
- More stable kidney function over time
Consider two examples:
- Sarah, a teacher who struggled with swelling and overwhelming fatigue due to proteinuria, committed to reducing salt, walking regularly, and monitoring her blood pressure. Over time, she reported feeling more energetic and less swollen.
- John began closely tracking his blood pressure, added daily walks, and cut back on processed foods. He describes feeling more empowered and involved in his own kidney care.
Everyone’s journey is different, but these stories highlight how small, consistent actions can add up.
Actionable Steps You Can Start Today
You do not need to change everything at once. Begin with manageable, realistic steps tailored to proteinuria:
-
Review your current habits
- Note how much salt you eat and how often you consume processed foods.
- Track how active you are during a typical day.
-
Set small, specific goals
- Add one 10–15 minute walk per day.
- Swap one processed snack for a fruit, vegetable, or unsalted option.
-
Monitor your symptoms
- Keep a simple journal of energy levels, swelling, and urine changes.
- Record any patterns or triggers you notice.
-
Talk to your healthcare provider
- Before major diet or exercise changes.
- For personalized guidance on managing proteinuria and adjusting medications if necessary.
Lifestyle Approaches vs. Medical Support for Proteinuria
Lifestyle changes and medical treatment are not opposites—they are partners. The right combination, under professional guidance, may offer the best protection for your kidneys.
Here is a simplified comparison:
| Benefit | Natural / Lifestyle Approach | Medication Support (Under Guidance) |
|---|---|---|
| Reduced inflammation | Omega-3–rich foods (e.g., salmon, flax) | Anti-inflammatory medications if prescribed |
| Better blood flow | Regular walking and moderate exercise | Blood pressure–lowering medications |
| Support for kidney function | Low-sodium, kidney-conscious diet | ACE inhibitors or similar drugs as advised |
| Enhanced hydration | Adequate water intake | Individualized fluid recommendations |
Lifestyle strategies can enhance, not replace, professional medical care. Always follow your doctor’s recommendations regarding tests, medications, and monitoring.
Step-by-Step Guide to Using These Strategies for Proteinuria
To put this into practice, consider this simple framework:
-
Diet Adjustment
- Emphasize vegetables, fruits, and whole grains.
- Aim to keep sodium at or below 2,300 mg per day, or lower if your provider recommends it.
-
Exercise Routine
- Work toward 30 minutes of moderate activity on most days of the week.
- Break it into shorter sessions if fatigue from proteinuria makes longer workouts difficult.
-
Hydration Goal
- Target around 64 ounces (about 2 liters) of water per day, adjusting based on your doctor’s advice and your symptoms.
-
Omega-3 Intake
- Include 1–2 servings per week of fatty fish or plant-based omega-3 sources.
Throughout these steps, stay in close communication with your healthcare team, especially if you notice changes in swelling, blood pressure, or urine patterns.
Conclusion: Small Changes, Real Possibilities
Overlooking lifestyle strategies may mean missing opportunities to feel more energetic and supported while living with proteinuria. Key themes include:
- Adopting a kidney-conscious, lower-sodium diet
- Keeping blood pressure in a healthy range
- Moving your body regularly, within your limits
- Staying hydrated as advised
- Incorporating omega-3–rich foods
- Quitting smoking and moderating alcohol
Even modest, consistent changes in these areas may contribute to better kidney health and quality of life.
One more gentle reminder: managing stress—something as simple as a few slow, deep breaths—can help calm your nervous system and support your overall efforts against the effects of proteinuria.
Share this with someone who might be struggling with proteinuria and could benefit from knowing they are not alone, and that practical steps are available.