Why Common Oral Infections May Feel Bigger Than “Just a Mouth Problem”
A sudden lip tingle, a sore that keeps coming back, or gums that bleed when you brush can seem like routine oral irritation. Still, many adults—especially over 40—worry these oral infections in your mouth could affect more than comfort, confidence, or appearance. When smiling for photos or enjoying food becomes stressful, it’s understandable to wonder whether something deeper is going on.
New research is exploring possible connections between common oral infections and long-term brain health topics, including Alzheimer’s disease. While this science is still developing, the most encouraging takeaway is practical: simple, consistent oral care habits can support everyday wellbeing and may help reduce ongoing inflammation and recurring issues.
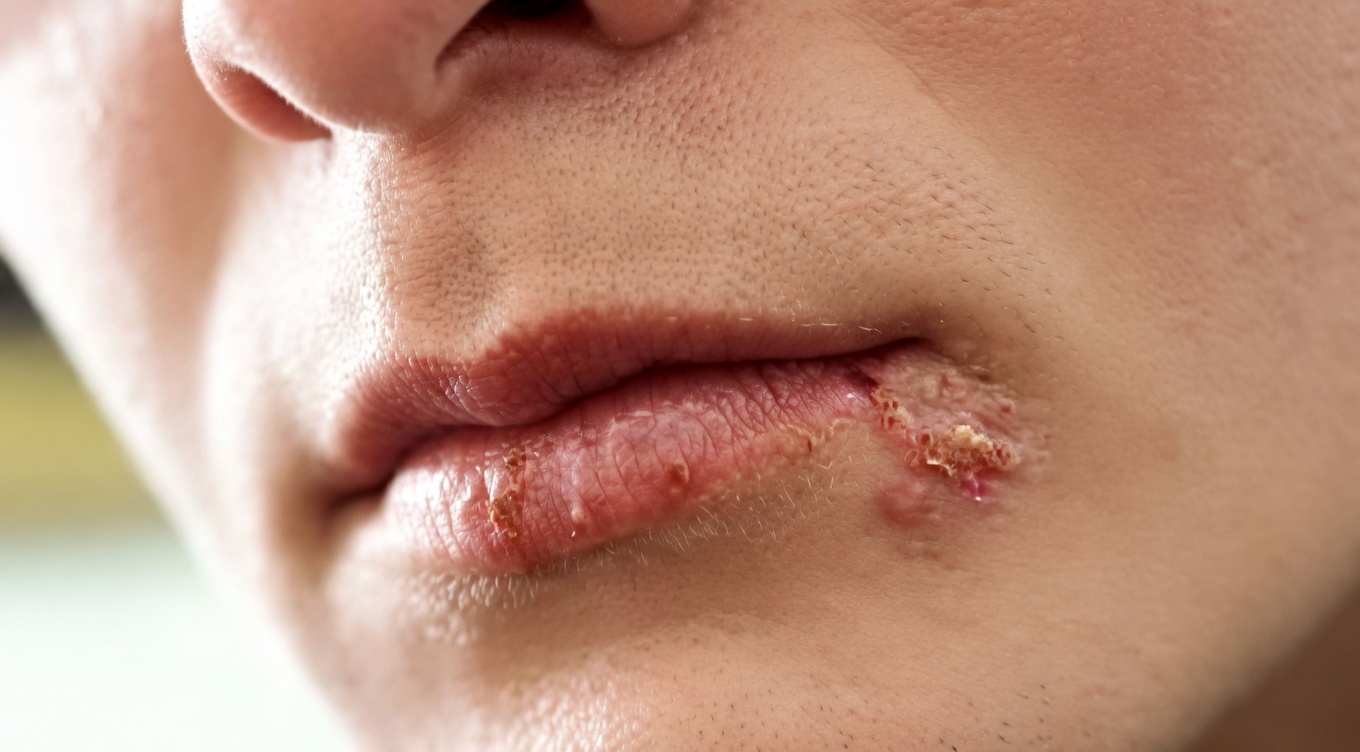
Cold Sores: A Common Viral Oral Infection in Your Mouth
Cold sores—also called fever blisters—often start with a familiar warning sign: itching, tingling, or burning near the lips. Most are caused by herpes simplex virus type 1 (HSV-1), although HSV-2 can occasionally be involved through close contact.
Because the virus can spread through saliva and skin-to-skin contact, outbreaks can make everyday moments—sharing a drink, kissing, or close contact—something to handle more carefully until symptoms settle. Recognizing the early “tingle stage” helps many people respond sooner and reduce the chance of spreading the infection.
What recent studies are asking about HSV-1 and dementia risk
Some medical publications in 2025 have examined whether a history of HSV-1 infection may be associated with higher dementia rates over time. These findings do not prove that cold sores cause dementia, but they have increased interest in early management of oral infections and keeping inflammation under control.
Gum Disease: A Quiet Bacterial Oral Infection Worth Taking Seriously
Bleeding, redness, and swelling along the gumline are common signs of gum disease, another major category of oral infections in your mouth. In long-term periodontitis, one bacterium often discussed is Porphyromonas gingivalis.
A widely cited 2019 study in Science Advances reported finding this bacterium and its toxic enzymes (called gingipains) in brain tissue samples from people with Alzheimer’s disease. That discovery raised new questions about whether chronic oral bacteria and inflammation could play a role beyond the mouth—or influence other body systems.
Even if you’ve tried to ignore gum symptoms, they often worsen over time, leading to more discomfort and self-consciousness. Although the science is still evolving and not every case is connected, these findings have reinforced a prevention-first message from dental professionals.

Cold Sores vs. Gum Disease: Quick Comparison
-
Type
- Cold sores: Viral (most often HSV-1)
- Gum disease: Bacterial (commonly involving P. gingivalis)
-
Typical signs
- Cold sores: Tingling and fluid-filled blisters near the lips
- Gum disease: Red, swollen, or bleeding gums
-
Common triggers
- Cold sores: Stress, sun exposure, lowered immunity
- Gum disease: Plaque buildup, inconsistent brushing/flossing
-
What research has explored
- Cold sores: 2025 studies examining HSV-1 history and dementia association
- Gum disease: 2019 research detecting P. gingivalis/gingipains in Alzheimer’s brain samples
-
Everyday impact
- Cold sores: Embarrassment and disruption during outbreaks
- Gum disease: Pain, bad breath, discomfort while eating or smiling
This side-by-side view highlights why balanced oral care matters for both comfort and peace of mind.

What Emerging Alzheimer’s Research Says About Oral Infections in Your Mouth
For many people over 50, the idea that everyday oral problems could relate to brain health can feel unsettling—especially when memory concerns are already a sensitive topic.
Research has investigated several possible pathways, including:
- Inflammation that persists over time
- Immune system responses to chronic infection
- Bacterial toxins and their potential effects beyond the gums
In the 2019 research mentioned earlier, gingipain levels were linked with changes associated with Alzheimer’s pathology (including tau-related findings). In animal models within that work, infection with P. gingivalis contributed to brain changes that resembled Alzheimer’s features. However, human outcomes vary, and experts emphasize that the evidence points to association—not confirmed causation.
Similarly, 2025 studies have reported higher dementia rates among people with documented HSV-1 infections, but these findings still stop short of proving a direct cause-and-effect relationship. The consistent theme is that reducing and managing oral infections may help people feel more proactive about long-term wellness.
Simple Daily Steps to Support Oral Health and Reduce Recurring Oral Infections
If recurring cold sores or gum irritation keeps interrupting your routine, these practical habits can help support oral health:
- Brush twice daily using a soft-bristled toothbrush and fluoride toothpaste for two full minutes
- Floss daily (or use interdental brushes) to clean areas a toothbrush can’t reach
- Use an antimicrobial mouthwash if your dentist recommends it
- Schedule dental checkups and cleanings about every six months
- Reduce cold sore triggers by managing stress and using SPF lip balm during sun exposure
Consistency matters: small steps done daily often make the biggest difference in preventing flare-ups and reducing inflammation.
A Simple Weekly Routine You Can Stick With
- Monday–Friday: Brush morning and night + floss once daily
- Weekend focus: Gentle tongue cleaning + regular SPF lip balm use
- Monthly check: Track new symptoms (lip tingling, gum bleeding, swelling) in a quick note or journal
Many people feel more confident simply by following a steady routine for a couple of weeks.
3 Common Questions About Oral Infections and Alzheimer’s Studies
-
Do cold sores automatically mean a higher Alzheimer’s risk?
No. Some 2025 findings report an association between HSV-1 history and dementia rates, but most people with occasional cold sores do not develop dementia. Managing viral flare-ups remains a smart general health step. -
Is gum disease proven to cause Alzheimer’s?
No. Research involving P. gingivalis and gingipains suggests a possible relationship, but experts still emphasize correlation rather than proven causation. Preventive dental care is beneficial either way. -
What if I get frequent oral infections in my mouth?
Book appointments with both your dentist and medical clinician. They can check for underlying causes, recommend targeted treatment, and help you interpret research without jumping to conclusions.
Final Thoughts: Stay Proactive Without Panic
Worry tends to shrink when your plan is clear. Whether you’re dealing with cold sores or gum sensitivity, steady oral hygiene, regular dental care, and early attention to symptoms can improve daily comfort and help you feel more in control as research on oral health and Alzheimer’s continues to develop.
Important note: This article is for informational purposes only and does not replace medical or dental advice. Always consult a qualified healthcare provider or dentist—especially if you have persistent oral infections, worsening symptoms, or memory concerns.