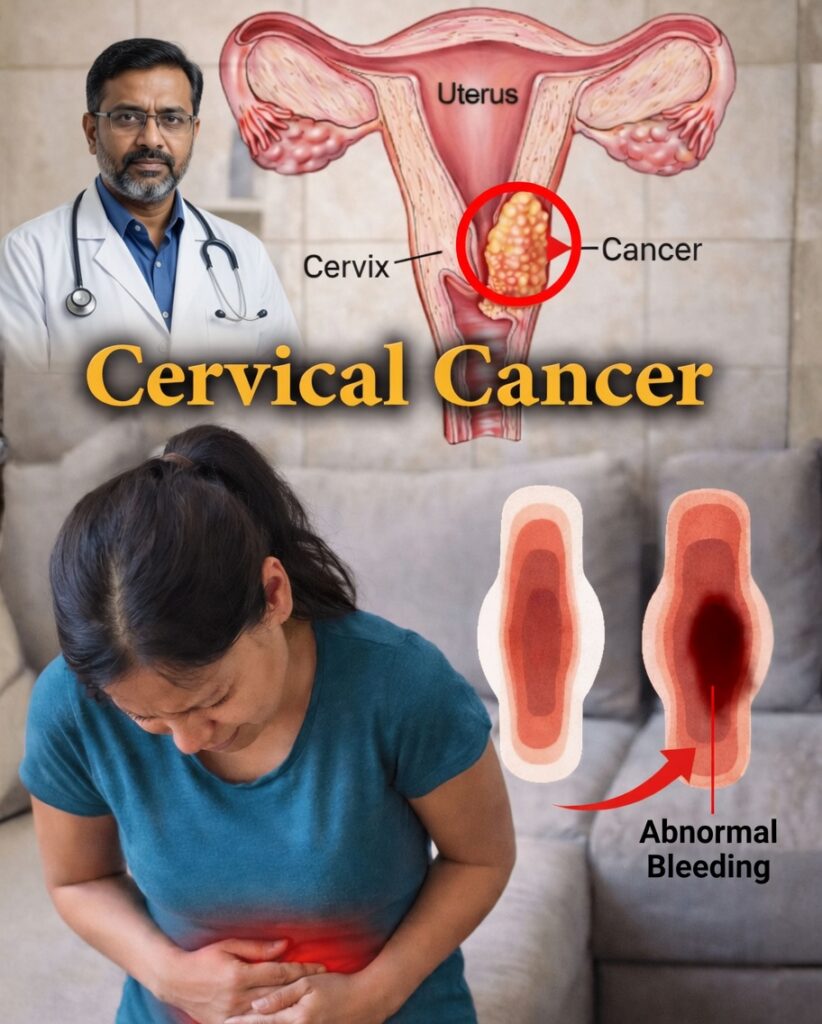
When Your Uterus Whispers: Subtle Signs You Shouldn’t Brush Off
Many women dismiss irregular bleeding, nagging pelvic aches, or strange discharge as “just hormones” or a side effect of stress and a hectic life. Only later do they realize those quiet changes were early warning signs their body was asking for help.
Living with constant doubt—wondering “Is this normal or should I be worried?”—can disturb your sleep, drain your energy, and overshadow everyday moments. The empowering truth is that recognizing these early shifts gives you options, control, and a better chance of protecting your long-term reproductive health.
There’s also one simple daily habit most women overlook that can dramatically change how in control they feel—keep reading to find it at the end.
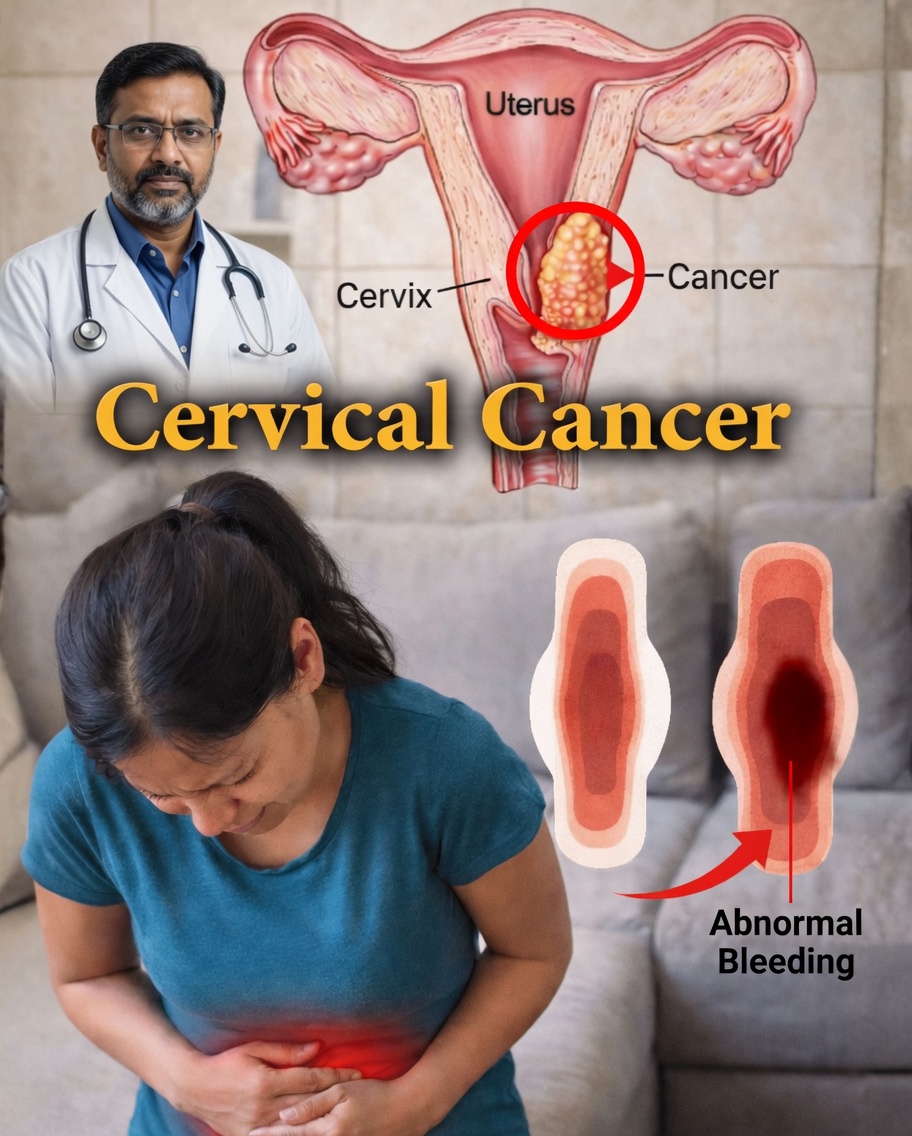
Bleeding Changes You Should Never Ignore
Your menstrual cycle is one of the clearest ways your uterus communicates. When your bleeding pattern changes unexpectedly, it’s often the first sign that something deserves a closer look.
1. Bleeding between periods
Light spotting or bleeding between your usual periods might seem minor at first. Still, many women later report this as the moment they first felt something was “not quite right.”
2. Bleeding after sex
If intercourse suddenly leaves blood on the sheets or on the tissue, your cervix or vaginal tissue may be irritated or undergoing changes. This is not a symptom to dismiss or wait out.
3. Bleeding after menopause
Once you have gone 12 months without a period, any vaginal bleeding—light or heavy—should be taken seriously. Postmenopausal bleeding is never considered normal and calls for medical evaluation.
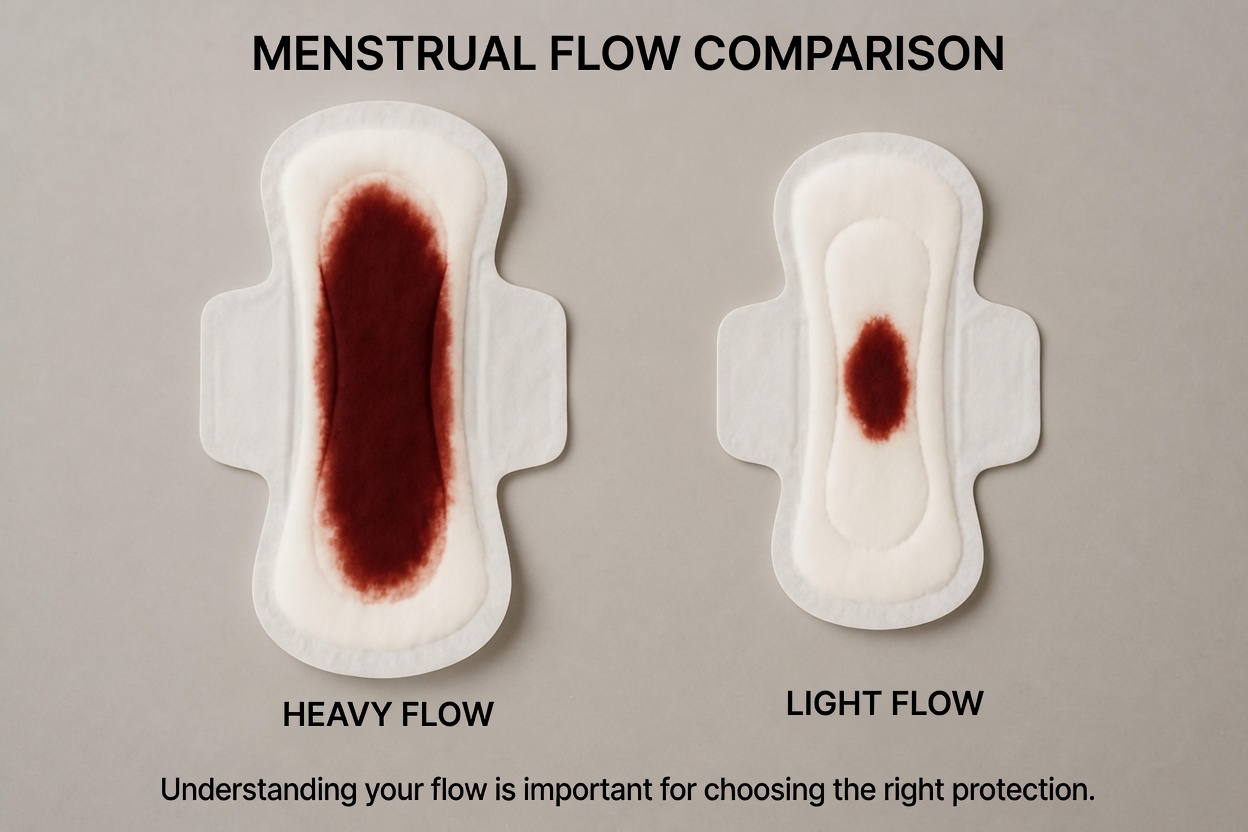
4. Periods that are heavier or longer than usual
Needing to change pads or tampons much more often, passing large clots, or bleeding for more than seven days can signal that your uterus is working harder than it should. These heavy periods can also lead to anemia and fatigue over time.
Bleeding is not the only way your body communicates. Your vaginal discharge carries important clues as well.

Discharge, Odor, and Other Quiet Signals
When what’s “normal” for you changes—whether it’s fluid, odor, or how your pelvis feels—your body may be sending a message you shouldn’t ignore.
5. Watery or pink-tinged discharge
Discharge that suddenly becomes very thin and watery, or takes on a pale pink tint, can feel unsettling. Even if it seems mild, this shift is worth noting and tracking over time.
6. Foul-smelling or unusual discharge
A strong, persistent odor or a noticeable change in color or texture is rarely just a “hygiene issue.” It can signal infection, inflammation, or other imbalances in the cervix, uterus, or vagina that need attention.
7. Ongoing pelvic or lower-back pain
Dull, dragging pain in the pelvic area that spreads to your lower back—and doesn’t fully go away with rest or over-the-counter pain relief—is a common complaint. If it lingers beyond your period or shows up regularly, it’s a sign to check in with a healthcare professional.
Pain, especially with intimacy or daily movement, is another clear red flag.
8. Pain or discomfort during intercourse
If sex that used to feel comfortable or pleasurable becomes sharp, deep, or consistently painful, your body is signaling that something has changed. This can be related to uterine, cervical, or pelvic floor issues and deserves an honest discussion with your doctor.
9. Unexplained fatigue that doesn’t improve with rest
Feeling unusually exhausted despite sleeping well can be tied to ongoing blood loss, anemia, inflammation, or chronic pelvic stress. When your uterus is under strain, your body may divert extra energy to cope—leaving you feeling depleted.
As changes progress, other organs and systems can start to react too.
10. Trouble urinating or frequent urges
Needing to pee all the time, feeling pressure on your bladder, or experiencing pain or burning when you urinate can sometimes be related to pelvic pressure from the uterus or nearby structures—not just a simple urinary tract infection.
11. Leg swelling or one-sided leg pain
Swelling, heaviness, or aching that appears mainly in one leg is less common but important to take seriously. In some cases, pelvic conditions can affect blood flow and increase the risk of clots or circulation issues.
12. Unexplained weight loss or persistent bloating
Sudden, unintentional weight loss, or ongoing bloating and abdominal fullness that doesn’t match your eating or menstrual cycle, is your body’s louder way of saying, “Pay attention.” These symptoms can be related to more advanced uterine or pelvic changes.
Individually, none of these signs mean you should panic. Together, they can form a pattern that deserves careful listening and professional evaluation.
What Research Says About These Warning Signs
Research shared by organizations such as the Mayo Clinic and the American Cancer Society has found that early symptoms like abnormal vaginal bleeding and unusual discharge are among the most common first clues of changes in the cervix or uterus.
The CDC also reports that many women feel completely well otherwise—no major pain or illness—until these symptoms appear. That’s why noticing and responding early matters. When you bring these changes to a healthcare provider, they can perform simple tests and exams that either reassure you or catch problems while they are easiest to manage.
5 Practical Steps You Can Start Today
You don’t need to wait for a major health scare to care for your reproductive system. These small, realistic habits can fit into any lifestyle:
-
Track your symptoms for at least two cycles
Use a phone app or notebook to record period start and end dates, flow intensity, spotting, discharge changes, and any pain or discomfort. -
Book an annual well-woman visit
Even if you feel fine, regular pelvic exams plus Pap and HPV testing (on the schedule your doctor recommends) can detect cervical and uterine changes long before serious symptoms appear. -
Support your body with nourishing choices
Eat iron-rich foods (such as leafy greens, beans, lean meats, or fortified cereals) and drink plenty of water, especially if your periods are heavy, to reduce fatigue and dizziness. -
Move your body gently every day
Walking, stretching, or yoga can ease pelvic tension, improve circulation, and help you become more aware of subtle shifts in how your body feels. -
Skip douching and heavily scented products
Douching, perfumed wipes, and strong vaginal sprays can disrupt your natural balance and mask important warning signs instead of addressing them.
And here is the “surprising” daily habit that helps many women feel more in control:
Regularly share what you notice with a trusted healthcare provider—don’t wait for things to get worse.
Simply speaking up about your symptoms, even if they feel small or embarrassing, is one of the most powerful actions you can take for your uterine and cervical health.
Why Paying Attention Early Makes a Big Difference
Tuning in to these 12 signals does not mean you’re expecting the worst; it means you’re giving your uterus and reproductive system the respect and care they deserve.
Most women who bring their concerns to a doctor discover that:
- The cause is manageable or minor, and
- The relief of knowing what’s going on is enormous.
By partnering with your healthcare provider early, you reduce anxiety, avoid unnecessary complications, and build a long-term foundation for reproductive wellness. Your body has carried you through every stage of life so far—responding to its early whispers helps you stay strong, informed, and confident in the years ahead.
Frequently Asked Questions
How often should women talk with their doctor about these signs?
Most experts recommend:
- An annual pelvic exam starting in early adulthood, and
- Pap and HPV screening every three to five years from age 21 onward, depending on your age, past results, and local guidelines.
If any of the 12 warning signs appear—especially abnormal bleeding or unusual discharge—schedule a visit sooner rather than waiting for your next routine check-up.
Are these symptoms always linked to something serious?
No. Many of these signs can be caused by common, treatable issues such as infections, benign fibroids, hormonal shifts, or cervical irritation. The important step is to rule out serious causes early so you can stop worrying and get the right treatment if needed.
Can everyday habits really affect uterine and cervical health?
Yes. Consistent symptom tracking, gentle daily movement, smart nutrition, and honest conversations with your doctor are simple habits that can:
- Catch changes sooner
- Reduce anxiety
- Support overall reproductive and hormonal balance
They might seem small, but over time, they create a powerful foundation for long-term health.
Disclaimer
This article is for educational and informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your healthcare provider with any questions you may have regarding symptoms, concerns, or medical conditions.